## Distinguishing Acute Cholecystitis from Biliary Colic **Key Point:** Gallbladder wall thickening (>3 mm) is the hallmark imaging sign of acute cholecystitis and differentiates it from uncomplicated biliary colic, where the wall remains normal (≤2 mm). ### Comparative Features | Feature | Acute Cholecystitis | Biliary Colic | |---------|-------------------|---------------| | **GB wall thickness** | >3 mm (edematous) | ≤2 mm (normal) | | **Gallstones** | Present (90%) | Present (100%) | | **Murphy's sign** | Positive (sonographic) | Negative | | **Pericholecystic fluid** | Present (severe cases) | Absent | | **CBD dilation** | Variable (if obstruction) | Absent | **High-Yield:** Wall thickening occurs due to inflammation and edema of the gallbladder mucosa and submucosa. This is the single most sensitive and specific ultrasound finding for acute cholecystitis. **Clinical Pearl:** Biliary colic is a functional disorder caused by gallstone impaction in the cystic duct, producing pain without inflammation. The gallbladder itself remains structurally intact on imaging, hence normal wall thickness. **Mnemonic:** **WALL** — Wall thickness >3 mm = **A**cute cholecystitis; **L**ess than 3 mm = **L**ithiasis (stones alone, no inflammation). ### Why Wall Thickening is the Best Discriminator 1. **Gallstones are present in both conditions** — not discriminatory 2. **Pericholecystic fluid is late finding** — only in severe/complicated cases 3. **CBD dilation is variable** — depends on stone location, not inflammation status 4. **Wall thickening is early, sensitive, and specific** — reflects acute inflammatory response [cite:Sabiston Textbook of Surgery Ch 53] 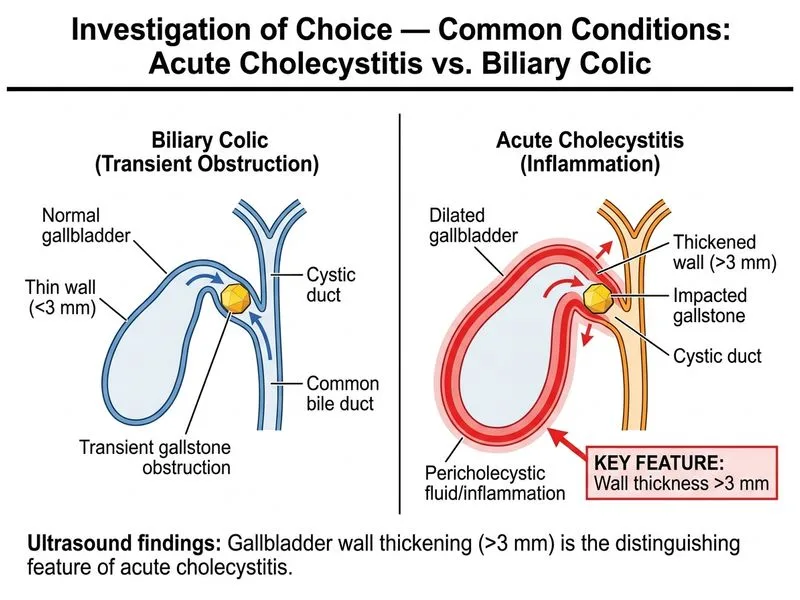
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.