## Investigation of Choice for Iron Deficiency Anemia ### Clinical Context The patient presents with classic features of iron deficiency anemia (IDA): microcytic hypochromic anemia (MCV 62 fL, Hb 7.2 g/dL), low serum ferritin (8 ng/mL), and mucosal changes (glossitis, angular cheilitis) indicating chronic iron depletion. The question asks for the **most appropriate investigation to confirm the diagnosis and assess iron stores** in this clinical scenario. ### Why Serum Iron and TIBC is the Most Appropriate Answer **Key Point:** In a patient with already low ferritin and microcytic anemia, **serum iron and TIBC (total iron-binding capacity)** is the most appropriate next investigation to confirm iron deficiency anemia and assess iron kinetics. This is the standard investigation recommended in NEET PG and clinical practice guidelines. **High-Yield:** In iron deficiency anemia: - **Serum iron** is decreased (< 60 µg/dL) - **TIBC** is increased (> 400 µg/dL) — reflects upregulation of transferrin - **Transferrin saturation** (serum iron/TIBC × 100) is decreased (< 16%) - Together, these findings **confirm IDA** and assess the iron transport compartment ### Diagnostic Criteria for IDA (Park's Textbook of Preventive and Social Medicine) | Parameter | Normal | Iron Deficiency Anemia | |---|---|---| | Serum ferritin | 12–150 ng/mL | **< 12 ng/mL** (diagnostic) | | Serum iron | 60–170 µg/dL | **Decreased** | | TIBC | 250–400 µg/dL | **Increased** | | Transferrin saturation | 20–50% | **< 16%** | | MCV | 80–100 fL | **< 80 fL** (microcytic) | ### Why Bone Marrow Aspiration (Option A) is NOT the Answer Here **Clinical Pearl:** Bone marrow aspiration with Prussian blue staining is the **gold standard** for assessing iron stores, but it is **invasive and NOT indicated** as the first-line or most appropriate investigation when: - Ferritin is already clearly low (< 12 ng/mL) — this alone is diagnostic of depleted iron stores - The clinical picture is straightforward (microcytic anemia + low ferritin + mucosal signs) Bone marrow examination is reserved for: 1. Diagnostic uncertainty (borderline ferritin with concurrent inflammation/infection) 2. Suspected bone marrow pathology (myelodysplasia, sideroblastic anemia) 3. Refractory anemia not responding to iron supplementation 4. Research/academic settings ### Why Other Options are Incorrect - **Option C (Serum B12 and folate):** These are relevant for macrocytic/megaloblastic anemia. This patient has microcytic anemia (MCV 62 fL), making B12/folate deficiency unlikely as the primary cause. - **Option D (Peripheral smear and reticulocyte count):** While useful for characterizing anemia morphologically, these do not directly assess iron stores and are not the most appropriate investigation to confirm IDA. **High-Yield for NEET PG:** Serum ferritin < 12 ng/mL is diagnostic of IDA in non-inflammatory states. Serum iron + TIBC provides complementary confirmation and is the standard investigation pair used in clinical practice and exam scenarios to "confirm diagnosis and assess iron stores." (Reference: Park's Textbook of PSM, 26th edition; Harrison's Principles of Internal Medicine, 21st edition) 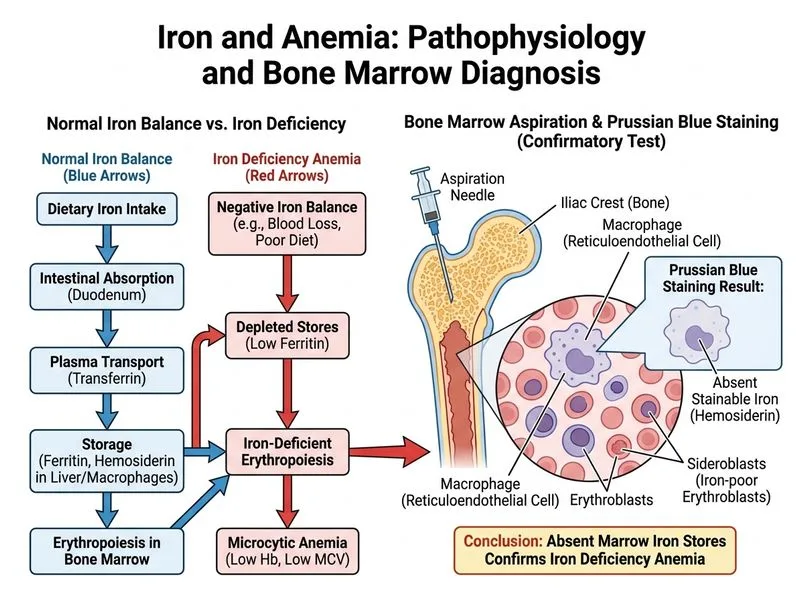
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.