## Investigation of Choice for Source Identification in Iron Deficiency Anemia with Overt GI Bleeding ### Clinical Context The patient has: - **Overt GI bleeding** (melena for 2 years) - **Severe iron deficiency anemia** (Hb 6.8 g/dL, MCV 68 fL, ferritin 5 ng/mL) - **Chronic blood loss** (weight loss, prolonged symptoms) Once iron deficiency is confirmed, the **next step is to identify the source** of chronic blood loss. ### Why Upper GI Endoscopy (OGD) is the Investigation of Choice **Key Point:** In a patient with **confirmed iron deficiency anemia and overt melena**, upper gastrointestinal endoscopy (OGD) is the **gold standard investigation** to visualize, identify, and potentially treat the bleeding lesion. **High-Yield:** Melena (black tarry stools) indicates **upper GI bleeding** (proximal to ligament of Treitz). OGD is: - **Direct visualization** of esophagus, stomach, and duodenum - **Diagnostic accuracy >95%** - **Therapeutic capability** (hemostasis, variceal ligation, polypectomy) - **First-line investigation** for suspected upper GI bleed ### Diagnostic Algorithm for Iron Deficiency with Chronic GI Bleeding ```mermaid flowchart TD A[Iron deficiency anemia confirmed]:::outcome --> B{Site of bleeding?}:::decision B -->|Melena/hematemesis| C[Upper GI source]:::outcome B -->|Hematochezia/occult| D[Lower GI source]:::outcome C --> E[OGD - gold standard]:::action D --> F[Colonoscopy]:::action E --> G{Lesion found?}:::decision G -->|Yes: ulcer/varices/polyp| H[Treat + iron supplementation]:::action G -->|No: negative OGD| I[Consider small bowel imaging]:::action ``` ### Comparison of Investigations for Source Identification in IDA | Investigation | Indication | Sensitivity | Specificity | Therapeutic Capability | |---|---|---|---|---| | **OGD (Upper GI endoscopy)** | Melena, hematemesis, upper GI symptoms | >95% | >95% | **Yes** (hemostasis, polypectomy, ligation) | | **Colonoscopy** | Hematochezia, lower abdominal symptoms | 90–95% | 95% | **Yes** (polypectomy, hemostasis) | | **FOBT** | Screening for occult bleeding | 50–60% | 90% | **No** (screening only, non-specific) | | **Capsule endoscopy** | Negative OGD + colonoscopy, obscure GI bleed | 70–80% | 85% | **No** (diagnostic only) | | **CT angiography** | Acute hemorrhage, hemodynamic instability | 85–90% | 80–85% | **No** (diagnostic; requires intervention) | **Clinical Pearl:** The **location of bleeding guides the investigation**: - **Melena** → Upper GI (OGD first) - **Hematochezia** → Lower GI (colonoscopy first) - **Occult blood loss** → FOBT screening, then OGD/colonoscopy based on clinical suspicion ### Why OGD is Superior in This Case 1. **Melena is pathognomonic for upper GI bleeding** → OGD is the gold standard 2. **Direct visualization** allows identification of: - Peptic ulcer disease (most common cause in India) - Esophageal varices (if cirrhosis suspected) - Gastric malignancy - Angiodysplasia - Mallory-Weiss tear 3. **Therapeutic intervention** possible during same procedure (hemostasis, variceal ligation) 4. **Diagnostic accuracy >95%** — superior to any non-invasive test **Mnemonic for Upper GI Bleeding Causes: "CHAMP"** - **C** — Cirrhosis (varices) - **H** — Hiatus hernia, Hemorrhagic gastritis - **A** — Aspirin/NSAIDs (ulcers) - **M** — Mallory-Weiss tear, Malignancy - **P** — Peptic ulcer disease ### Why This Patient Needs OGD (Not FOBT) - **FOBT is a screening test**, not a diagnostic investigation - Patient already has **overt melena** (not occult bleeding) → FOBT is redundant - FOBT has low sensitivity (50–60%) and cannot identify the lesion - OGD is the definitive next step after IDA is confirmed **Tip:** In clinical practice, the investigation sequence for IDA is: 1. **Confirm IDA** (ferritin, iron studies, peripheral smear) 2. **Identify source of blood loss** (OGD if melena; colonoscopy if hematochezia; FOBT if occult) 3. **Treat the underlying cause** + iron supplementation 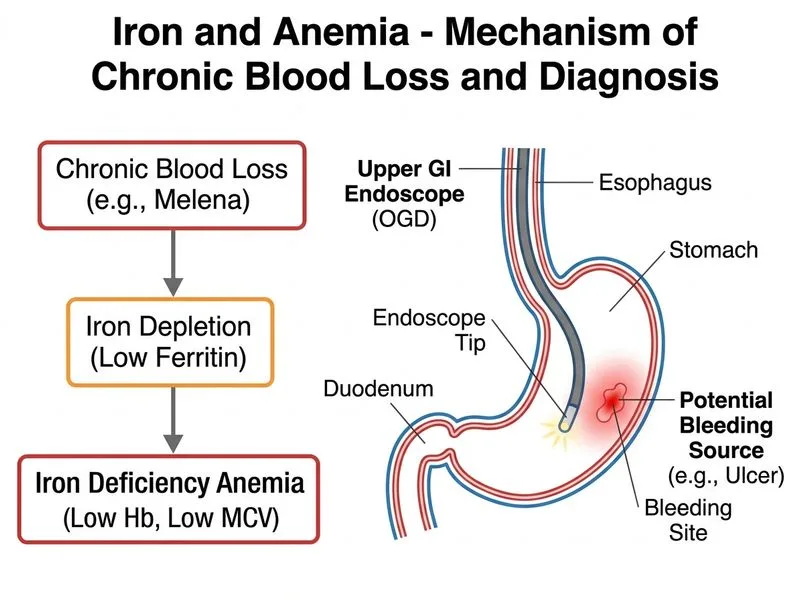
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.