## Discriminating Anemia of CKD from Iron Deficiency Anemia ### The Core Distinction **Key Point:** The best laboratory finding that distinguishes anemia of CKD from iron deficiency anemia (IDA) secondary to malabsorption is **normal or elevated serum ferritin with low transferrin saturation** (Option D). This pattern is characteristic of CKD, where iron stores are preserved but functional iron availability is restricted by elevated hepcidin. In contrast, IDA from malabsorption shows **low serum ferritin** (depleted stores) with low transferrin saturation and elevated TIBC. ### Comparative Iron Metabolism Table | Parameter | Anemia of CKD | Iron Deficiency Anemia (Malabsorption) | |-----------|---------------|----------------------------------------| | **Serum Ferritin** | Normal or ↑ elevated | ↓ Low (<30 ng/mL) | | **Serum Iron** | ↓ Low | ↓ Low | | **TIBC** | ↓ Low or normal | ↑ Elevated | | **Transferrin Saturation** | ↓ Low | ↓ Low | | **Hepcidin** | ↑ Elevated (uremia + inflammation) | Normal or ↓ low | | **EPO Level** | ↓ Low (primary defect) | Normal or ↑ elevated | | **RDW** | Normal or mildly ↑ | ↑ Elevated | ### Pathophysiologic Basis **High-Yield:** CKD anemia is primarily due to **EPO deficiency** (failing kidneys cannot produce adequate EPO) and **hepcidin elevation** (due to uremia and chronic inflammation), which sequesters iron in macrophages and hepatocytes. This results in preserved iron stores (normal/elevated ferritin) but impaired iron delivery to erythroid precursors (low transferrin saturation). Conversely, celiac-induced IDA results from mucosal damage and malabsorption of dietary iron, leading to true iron depletion — low ferritin, low serum iron, elevated TIBC, and low transferrin saturation. ### Why Option D Is the Best Discriminator **Clinical Pearl:** Both conditions share **low transferrin saturation**, so that parameter alone does not distinguish them. The critical differentiator is **serum ferritin**: - **CKD:** Ferritin is normal or elevated (iron stores intact; hepcidin blocks release) → low transferrin saturation despite adequate stores. - **IDA (malabsorption):** Ferritin is low (iron stores depleted) → low transferrin saturation with compensatory elevation of TIBC. Option D captures this pattern: "Normal or elevated serum ferritin with low transferrin saturation" is the hallmark of CKD anemia and is absent in IDA. ### Why Other Options Are Incorrect - **Option A (Elevated creatinine/low eGFR):** Confirms CKD diagnosis but does NOT distinguish the *type* of anemia — a CKD patient can have superimposed iron deficiency, making this an unreliable discriminator of anemia etiology. - **Option B (Elevated reticulocyte count with hypochromic microcytic indices):** Both CKD anemia and IDA typically show a **low or inappropriately normal** reticulocyte count (hypoproliferative pattern). An elevated reticulocyte count would suggest hemolysis or recovery, not either of these conditions. - **Option C (Low serum EPO):** While EPO deficiency is the primary mechanism in CKD anemia, serum EPO levels are not routinely measured in clinical practice and are not the standard discriminating test. Moreover, EPO levels can be difficult to interpret without context. [cite: Harrison's Principles of Internal Medicine, 21e, Ch 99 (Anemia of Chronic Kidney Disease); KD Tripathi Essentials of Medical Pharmacology, 8e, Ch 12; Robbins & Cotran Pathologic Basis of Disease, 10e, Ch 14] 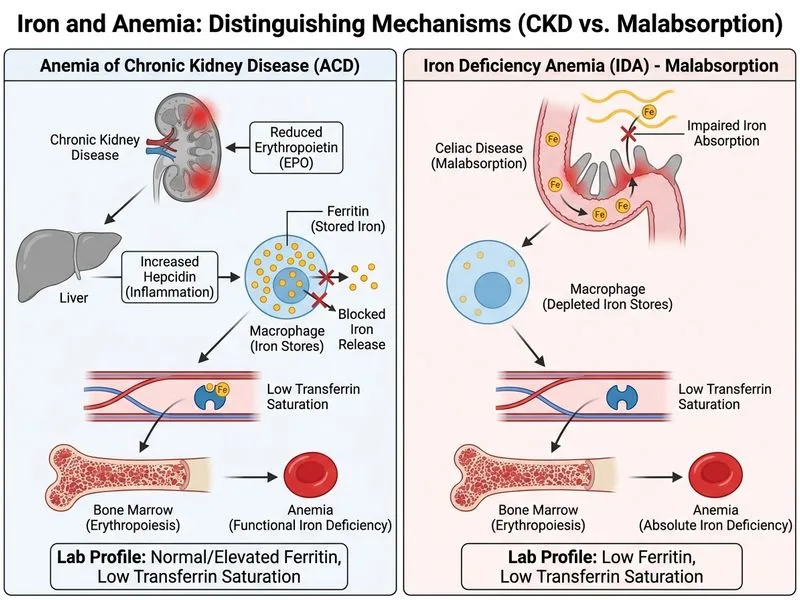
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.