## Clinical Context: Iron Deficiency in Early Childhood **Key Point:** Iron deficiency anemia (IDA) in children aged 6 months to 3 years is a critical window for neurodevelopment. Iron is essential for myelination, neurotransmitter synthesis, and mitochondrial function in the developing brain. ### Why This Child Is at High Risk | Risk Factor | Present in Case | Impact | |-------------|-----------------|--------| | Age 6 years | Yes | Critical period for cognitive development (myelination ongoing until age 8) | | Severe IDA (Hb 9.8, ferritin 12) | Yes | Prolonged iron deprivation of CNS | | Pica (mud/chalk eating) | Yes | Indicates severe iron hunger; also risk for lead/parasitic exposure | | Developmental delay (speech, motor) | Yes | Already showing neurodevelopmental lag | | Socioeconomic deprivation | Yes (1-room tenement) | Compounded malnutrition, poor healthcare access | | Elevated lead level (18 µg/dL) | Yes | **Synergistic neurotoxicity with iron deficiency** | **Clinical Pearl:** Lead and iron deficiency are synergistic neurotoxins. Lead competes with iron for intestinal absorption and impairs iron-dependent enzyme function. Together, they cause greater cognitive damage than either alone. ### Mechanisms of Iron Deficiency–Induced Neurotoxicity ```mermaid flowchart TD A[Iron Deficiency in Early Childhood]:::outcome --> B[Reduced CNS Iron Availability]:::outcome B --> C1[Impaired Myelination<br/>Oligodendrocyte dysfunction]:::outcome B --> C2[Reduced Cytochrome c oxidase<br/>Mitochondrial ATP production ↓]:::outcome B --> C3[Impaired Dopamine synthesis<br/>Monoamine oxidase dysfunction]:::outcome B --> C4[Reduced Myelin Basic Protein<br/>Axonal growth inhibition]:::outcome C1 --> D[Slowed neural conduction<br/>Reduced white matter volume]:::outcome C2 --> E[Energy failure in neurons<br/>Apoptosis risk]:::outcome C3 --> F[Behavioral abnormalities<br/>Attention deficits]:::outcome C4 --> G[Impaired axonal myelination<br/>Synaptic plasticity ↓]:::outcome D --> H[Cognitive Impairment<br/>Developmental Delay]:::urgent E --> H F --> H G --> H H --> I[**Persistent even after<br/>iron repletion in older children**]:::urgent ``` ### Critical Window: Reversibility vs. Irreversibility **High-Yield:** The **critical period for reversibility** is **0–24 months of age**. After age 3 years, cognitive deficits from IDA become increasingly **irreversible**, even with iron repletion. | Age Group | IDA Duration | Cognitive Outcome After Iron Therapy | |-----------|--------------|---------------------------------------| | 0–12 months | Weeks to months | Fully reversible if caught early | | 12–24 months | Months | Mostly reversible; some deficits persist | | **2–3 years** | **Months to years** | **Partial reversibility; lasting deficits** | | > 3 years | Chronic | **Largely irreversible** | **This 6-year-old is beyond the critical window.** He has had 8 months of IDA with developmental delay already evident. Even with aggressive iron repletion now, the cognitive and motor deficits are likely to persist. ### Why the Other Options Are Wrong **Recurrent infections (Option B):** While iron is important for immune function, IDA does NOT typically cause recurrent severe infections or sepsis. Immune deficits in IDA are mild and reversible with iron repletion. This is not the primary long-term concern. **Cardiac hypertrophy (Option C):** Chronic IDA can cause high-output cardiac failure (due to increased CO to maintain O₂ delivery), but this is reversible with iron repletion and is not the most serious long-term outcome in a 6-year-old. Cardiac complications are more common in severe, prolonged anemia (Hb < 5) in older children/adults. **Hemolysis and renal dysfunction (Option D):** IDA does not cause hemolysis or secondary renal disease. This is a distractor based on confusion with hemolytic anemias or chronic kidney disease. ### Management Implications 1. **Urgent iron therapy:** Ferrous sulfate 3–6 mg/kg/day elemental iron (e.g., 200 mg ferrous sulfate syrup daily for a 6-year-old). 2. **Lead exposure mitigation:** Identify and remediate lead sources (old paint, contaminated soil in tenement). 3. **Nutritional counseling:** Iron-rich foods (fortified cereals, legumes, leafy greens), vitamin C co-administration. 4. **Developmental assessment:** Refer to pediatric neuropsychologist for formal cognitive and speech evaluation — early intervention (speech therapy, occupational therapy) may help partially compensate for deficits. 5. **Socioeconomic support:** Link family to public health programs (ICDS, nutrition supplementation schemes). **Mnemonic: IRON BRAIN WINDOW — Iron deficiency, Reversible (< 2 yrs), Ongoing myelination, Neurotransmitter synthesis, Brain plasticity, Reduced after age 3, Age matters, Irreversible in older children, Neurodevelopmental lag, Window closes** 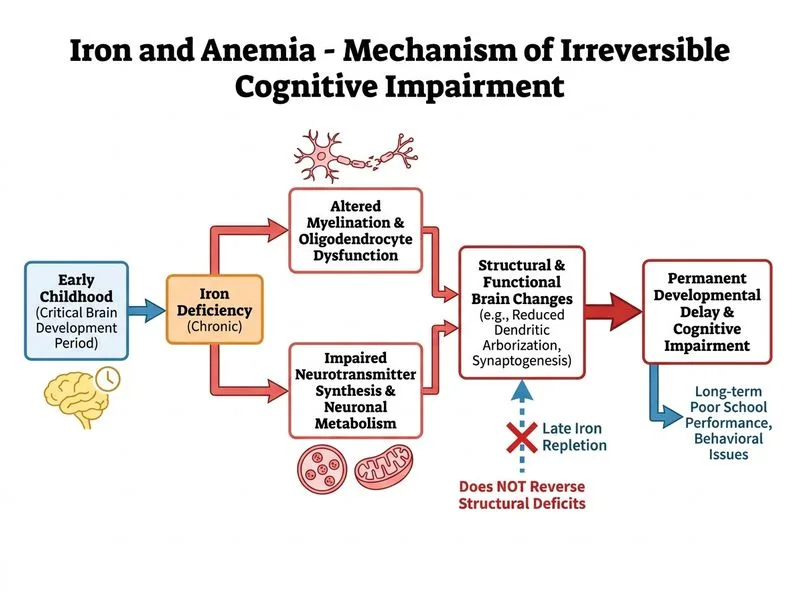
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.