## Clinical Diagnosis This child has **nutritional iron deficiency anemia** with clear etiology: - **Hemoglobin 9.8 g/dL** (mild-to-moderate anemia in a 5-year-old; normal Hb for age ~12–14 g/dL) - **MCV 68 fL** (microcytic) - **Serum ferritin 12 ng/mL** (depleted iron stores) - **Serum iron 35 µg/dL** (low; normal ~60–170 µg/dL) - **Dietary history:** Excessive cow's milk (low bioavailable iron), minimal meat (heme iron source), poor vegetable intake **Key Point:** Cow's milk is a major risk factor for IDA in young children because: - Very low iron content (~0.1 mg/L) - Calcium and phosphate inhibit iron absorption - Milk protein can cause occult GI bleeding in susceptible children - Displaces iron-rich foods from diet ## Management in Pediatric Nutritional IDA ```mermaid flowchart TD A[Pediatric IDA Confirmed]:::outcome --> B{Etiology Clear?}:::decision B -->|Yes: Nutritional| C[Oral Iron + Dietary Counseling]:::action B -->|No: Unclear| D[Investigate: Celiac, Bleeding, Malabsorption]:::action C --> E[Reassess Hb in 4-6 weeks]:::action E --> F{Response?}:::decision F -->|Good response| G[Continue iron, Reinforce diet]:::action F -->|Poor response| H[Investigate cause, Consider IV iron]:::action D --> I[Endoscopy, Serology, Imaging as indicated]:::action ``` ## Why Oral Iron + Dietary Counseling is Correct **High-Yield:** In a child with clear nutritional etiology and stable hemoglobin, the first-line approach is: 1. **Oral iron supplementation** - Ferrous sulfate syrup: 3–6 mg/kg/day elemental iron (divided doses) - Expected response: Reticulocytosis in 3–5 days; Hb rise 0.5–1 g/dL per week - Reassess at 4–6 weeks 2. **Dietary counseling (CRITICAL in pediatric IDA)** - Reduce cow's milk to <500 mL/day (adequate for calcium, but not excessive) - Introduce **heme iron sources:** meat, poultry, fish (2–3 times per week) - Add **plant iron sources:** fortified cereals, legumes, leafy greens - Pair iron-rich foods with **vitamin C** (citrus, tomato) to enhance absorption - Avoid tea, coffee, and calcium supplements with meals (inhibit absorption) **Clinical Pearl:** In children, dietary modification alone may not be sufficient if iron stores are severely depleted; iron supplementation + dietary change is synergistic and most effective. ## Why This Approach Addresses Root Cause Unlike adults with IDA (where GI bleeding is common), **nutritional IDA in children is almost always dietary**. Correcting the diet prevents recurrence after iron therapy is stopped. | Aspect | Nutritional IDA | Bleeding-Related IDA | |--------|-----------------|---------------------| | Ferritin | Low | Low | | Serum iron | Low | Low | | TIBC | Elevated | Elevated | | Cause | Diet | GI bleeding, other | | First-line | Oral iron + diet | Investigate bleeding source | | Prognosis | Excellent with diet change | Depends on bleeding control | **Tip:** Always ask about milk intake, meat consumption, and pica in children with IDA. Dietary history often reveals the diagnosis. 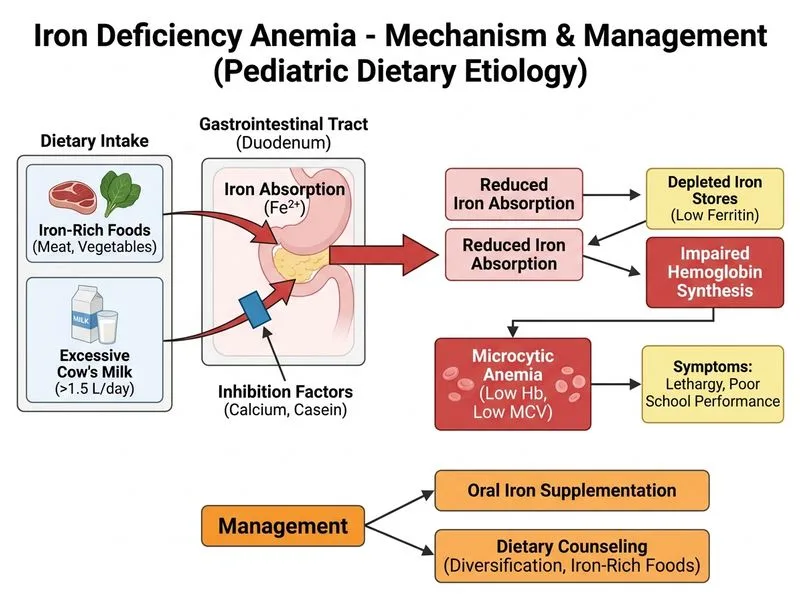
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.