## Distinguishing Iron Deficiency Anemia from Anemia of Chronic Disease ### The Core Discriminator **High-Yield:** Total iron-binding capacity (TIBC) is the single best discriminating feature between iron deficiency anemia (IDA) and anemia of chronic disease (ACD). In IDA, the body attempts to maximize iron absorption, so TIBC is **elevated**. In ACD, hepcidin-mediated iron sequestration suppresses iron absorption, so TIBC is **low or normal**. ### Comparative Laboratory Profile | Feature | Iron Deficiency Anemia | Anemia of Chronic Disease | |---------|------------------------|---------------------------| | **Serum Ferritin** | ↓ Low (<12 ng/mL) | ↑ Normal or elevated (>100 ng/mL) | | **Serum Iron** | ↓ Low (<50 µg/dL) | ↓ Low (<50 µg/dL) | | **TIBC** | ↑↑ **Elevated (>400 µg/dL)** | ↓ Low or normal (<250 µg/dL) | | **Transferrin Saturation** | ↓ Low (<16%) | ↓ Low (<16%) | | **Bone Marrow Iron** | Absent | Present | **Key Point:** Both IDA and ACD present with low serum iron and microcytic anemia, making these features non-discriminatory. However, the **TIBC response differs fundamentally** because: - In IDA: iron stores are depleted → body upregulates iron absorption machinery → TIBC rises - In ACD: iron is sequestered (not depleted) → hepcidin suppresses absorption → TIBC stays low ### Why Serum Ferritin Alone Is Insufficient While low ferritin strongly suggests IDA, ferritin is an acute-phase reactant. In chronic inflammation (ACD), ferritin may be normal or elevated *despite* low iron availability. This overlap makes ferritin less reliable as a sole discriminator. **Clinical Pearl:** In mixed IDA + ACD (e.g., chronic kidney disease with GI bleeding), ferritin may be misleadingly normal, but TIBC remains the most reliable marker of true iron depletion. ### Mnemonic **TIBC = True Iron Body Capacity** - **T**rue iron need (IDA) → TIBC ↑ - **C**hronic disease (ACD) → TIBC ↓ [cite:Park 26e Ch 7] 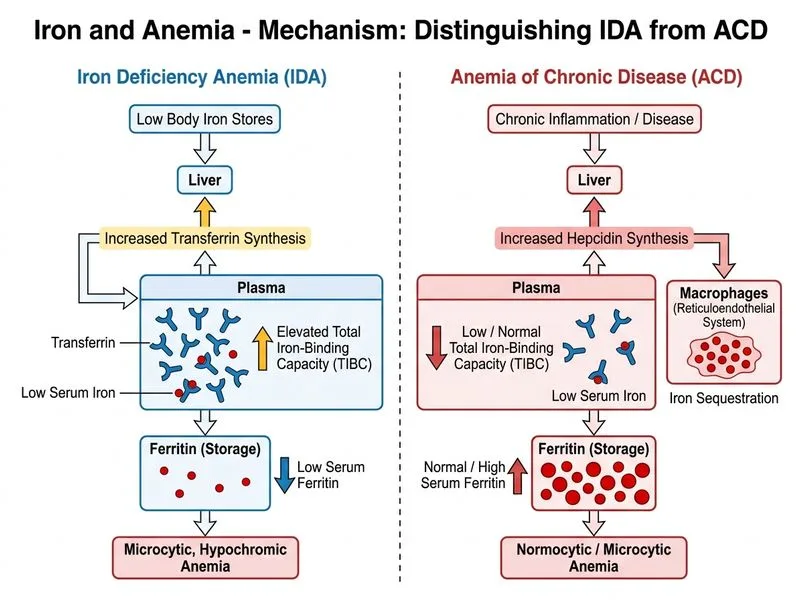
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.