## Distinguishing Iron Deficiency Anemia from Thalassemia Trait ### The Critical Discriminator: Hemoglobin Electrophoresis **High-Yield:** Hemoglobin A2 (HbA2) level on high-performance liquid chromatography (HPLC) is the **single definitive discriminator** between iron deficiency anemia (IDA) and beta-thalassemia trait (BTT). In BTT, HbA2 is **elevated (>3.5%)** due to compensatory upregulation of δ-globin chains. In IDA, HbA2 is **normal (<3.5%)**. ### Comparative Laboratory and Clinical Profile | Feature | Iron Deficiency Anemia | Beta-Thalassemia Trait | |---------|------------------------|------------------------| | **Hemoglobin A2 (HbA2)** | Normal (<3.5%) | **↑ Elevated (3.5–7%)** | | **Hemoglobin F (HbF)** | Normal (<1%) | Normal or slightly ↑ | | **RDW** | ↑ Elevated (>15%) | Normal or low (<15%) | | **Mentzer Index (MCV/RBC)** | >13 | <13 | | **Serum Ferritin** | ↓ Low | Normal/elevated | | **Serum Iron** | ↓ Low | Normal | | **Target Cells** | Few | Many | | **Bone Marrow Iron** | Absent | Present | | **Clinical History** | Menorrhagia, poor diet, GI loss | Family history, ethnicity (Mediterranean, Asian, African) | ### Why Other Features Fail to Discriminate **Target cells** appear in both IDA and BTT because both cause hypochromia and reduced hemoglobin content. Target cells are a morphologic consequence of reduced MCHC, not a diagnostic feature. **RDW** is elevated in IDA (heterogeneous RBC population due to variable iron availability) but often **normal or low in BTT** (homogeneous microcytic population). While RDW can suggest IDA, it is not pathognomonic and overlaps with other conditions. **Microcytic hypochromic morphology** is present in both conditions and reflects reduced hemoglobin synthesis, not the underlying etiology. ### Pathophysiology of HbA2 Elevation in BTT ```mermaid flowchart TD A[Beta-Thalassemia Trait]:::outcome --> B[Reduced β-globin synthesis]:::outcome B --> C[Relative excess of α-globin chains]:::outcome C --> D{Compensatory mechanism}:::decision D -->|δ-globin upregulation| E[HbA2 elevation]:::action D -->|γ-globin upregulation| F[HbF elevation]:::action E --> G[HbA2 > 3.5%]:::outcome F --> H[HbF mildly elevated]:::outcome ``` **Key Point:** In IDA, all globin chains are produced normally; iron is the limiting factor. Therefore, the ratio of HbA2 to HbA remains normal. In BTT, β-globin synthesis is intrinsically reduced, forcing compensatory δ-globin synthesis and HbA2 elevation. ### Clinical Pearl A young woman with microcytic anemia and menorrhagia is more likely to have IDA, but **family history of thalassemia, ethnic origin (Mediterranean, Southeast Asian, African), and normal serum ferritin** should raise suspicion for BTT. **HPLC is the gold standard** for definitive diagnosis. ### Mnemonic **HbA2 = Hereditary Abnormality 2** - Elevated in **β-thalassemia trait** (δ-chain compensation) - Normal in **iron deficiency anemia** (normal globin synthesis) [cite:Harrison 21e Ch 99; Park 26e Ch 7] 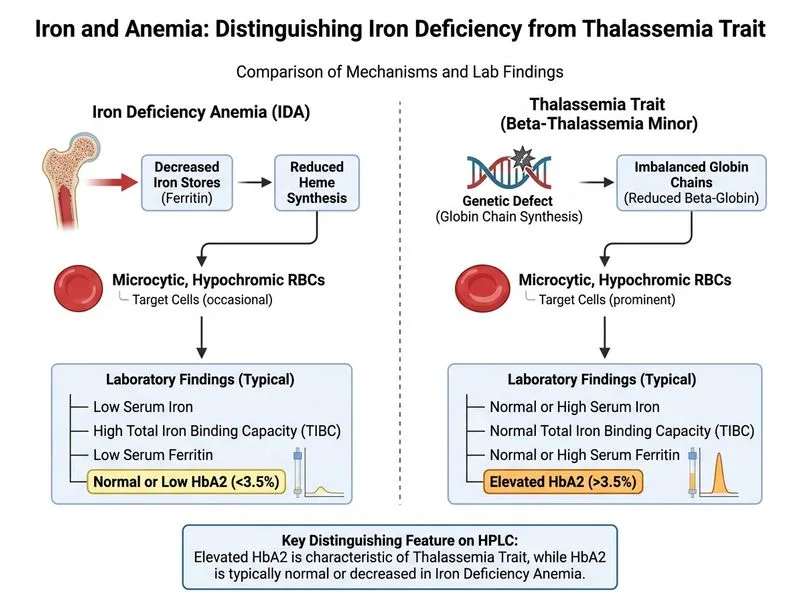
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.