## Investigation Strategy for Iron Deficiency Anemia with Occult Blood Loss ### Clinical Context **Key Point:** This patient has confirmed iron deficiency anemia (low ferritin, elevated TIBC, microcytic hypochromic indices) with **no obvious source of bleeding** despite normal upper GI endoscopy and colonoscopy. The next step is to identify occult blood loss, particularly from the small bowel. ### Diagnostic Algorithm for IDA with Occult Bleeding ```mermaid flowchart TD A[Iron Deficiency Anemia Confirmed]:::outcome --> B{Obvious source of bleeding?}:::decision B -->|Yes: GI/GYN bleeding| C[Treat source]:::action B -->|No: Occult bleeding| D[Upper GI endoscopy]:::action D --> E{Lesion found?}:::decision E -->|Yes| F[Treat lesion]:::action E -->|No| G[Colonoscopy]:::action G --> H{Lesion found?}:::decision H -->|Yes| I[Treat lesion]:::action H -->|No| J[Small bowel evaluation]:::action J --> K[Fecal occult blood test]:::action K --> L{Positive?}:::decision L -->|Yes| M[Capsule endoscopy or enterography]:::action L -->|No| N[Consider non-GI sources]:::action ``` ### Why Fecal Occult Blood Test (FOBT) and Small Bowel Capsule Endoscopy? **High-Yield:** After upper GI and lower GI endoscopy are negative, the small bowel is the next most common site of occult bleeding in IDA. The small bowel accounts for 5–10% of GI bleeding sources and is often missed by conventional endoscopy. 1. **Fecal Occult Blood Test (FOBT):** - Non-invasive screening for ongoing blood loss - Positive FOBT confirms GI source of bleeding - Negative FOBT suggests either: - Intermittent bleeding (may need repeat testing) - Non-GI source (malabsorption, dietary insufficiency, rare in adult men) 2. **Small Bowel Capsule Endoscopy:** - Gold standard for small bowel evaluation - Can visualize mucosa of entire small bowel (duodenum, jejunum, ileum) - Diagnostic yield: 40–70% in IDA with negative upper/lower endoscopy - Common findings: - Angiodysplasia (most common, 40–50%) - Meckel's diverticulum - Small bowel tumors (lymphoma, adenocarcinoma) - Crohn's disease - Celiac disease (if not already excluded) **Clinical Pearl:** In men > 50 years with IDA and negative upper/lower endoscopy, small bowel pathology is found in 50–70% of cases. Capsule endoscopy is the investigation of choice. ### Why Not the Other Options? **Bone Marrow Biopsy (Option 1 — Incorrect):** - Bone marrow shows hypercellularity with erythroid predominance in IDA (compensatory erythropoiesis) - Iron staining shows **absent iron stores** (no stainable iron in macrophages) - However, bone marrow biopsy is **not needed for diagnosis** — ferritin already confirms iron deficiency - Bone marrow is invasive and does not identify the source of blood loss - It is useful only if diagnosis is uncertain or to rule out other causes (e.g., sideroblastic anemia, aplasia) **Hemoglobin Electrophoresis (Option 2 — Incorrect):** - Used to diagnose hemoglobinopathies (sickle cell, thalassemia, HbC disease) - This patient's microcytic anemia is due to iron deficiency, not a hemoglobinopathy - Hemoglobin electrophoresis is not indicated when iron studies confirm iron deficiency - Thalassemia trait would have normal/elevated ferritin and normal TIBC **Serum Transferrin Receptor Level (Option 3 — Incorrect):** - Transferrin receptor is elevated in iron deficiency (reflects erythroid activity and iron demand) - It is useful to **differentiate IDA from ACD** when ferritin is in the intermediate range (30–100 ng/mL) - In this case, ferritin is very low (6 ng/mL), making diagnosis of IDA certain - Transferrin receptor does not identify the **source** of blood loss - It is not the next appropriate investigation for finding occult bleeding ### Laboratory Interpretation in This Patient | Test | Value | Interpretation | |------|-------|----------------| | Ferritin | 6 ng/mL | Diagnostic of iron deficiency (< 12) | | Serum iron | 28 μg/dL | Low (normal 60–170) | | TIBC | 450 μg/dL | Elevated (normal 250–425) | | Transferrin saturation | 6% | Very low (normal 20–50%) | | MCV | 68 fL | Microcytic | | RBC count | 6.2 × 10¹²/L | Elevated (compensatory) | **Key Point:** The diagnosis of iron deficiency is **already confirmed**. The next step is to find the source of iron loss. ### Mnemonic: Investigation Sequence in IDA **FOBT-SCOPE:** - **F** — Ferritin (confirms diagnosis) - **O** — Occult blood test (screens for GI loss) - **B** — Both upper and lower endoscopy (visualize proximal and distal GI tract) - **T** — Then capsule endoscopy (if upper/lower negative, evaluate small bowel) - **S** — Small bowel imaging (enterography, MR enterography as alternative) - **C** — Consider non-GI sources (malabsorption, dietary, rare) - **O** — Ongoing monitoring (repeat FOBT, follow-up endoscopy) - **P** — Proceed with iron supplementation (while investigating source) - **E** — Exclude other causes (celiac disease, H. pylori) 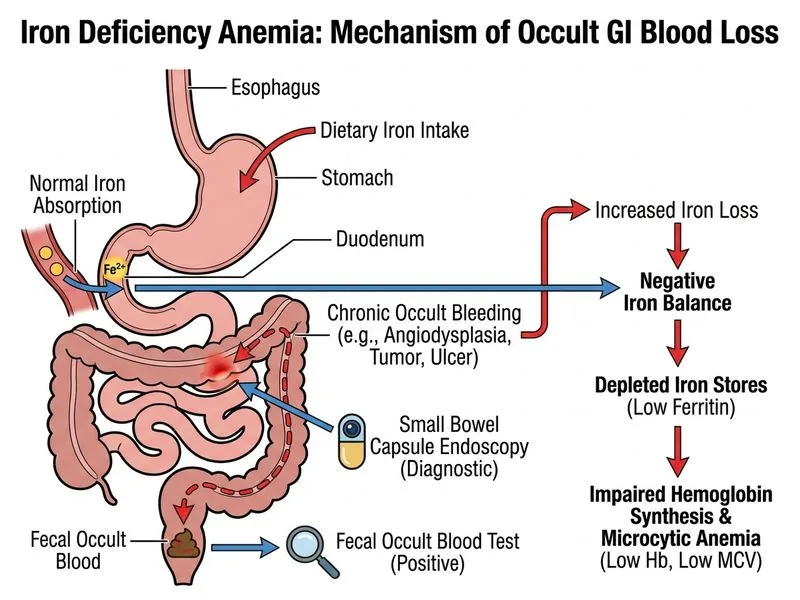
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.