## Clinical Presentation Analysis The patient presents with acute brainstem/cerebellar syndrome: - **Vertigo and ataxia** → cerebellar dysfunction - **Left facial numbness** → trigeminal nerve involvement (brainstem or CN V) - **Timeline:** 4 hours (within thrombolytic window) ## Anatomical Localization **Key Point:** The combination of vertigo, ataxia, and ipsilateral facial sensory loss is classic for **PICA (Posterior Inferior Cerebellar Artery) territory infarction**, also known as **Wallenberg syndrome** when it involves the lateral medulla. | Artery | Territory | Clinical Features | |---|---|---| | **PICA** | Cerebellar hemisphere + lateral medulla | Vertigo, ataxia, ipsilateral facial numbness, Horner syndrome | | **AICA** | Lateral pons + cerebellum | Facial weakness, hearing loss, ataxia | | **SCA** | Midbrain + superior cerebellum | Tremor, dysarthria, ataxia | | **Basilar** | Pons + midbrain | Bilateral signs, locked-in syndrome | ## Imaging Interpretation **High-Yield:** - **DWI hyperintensity** in cerebellar hemisphere = acute infarction (cytotoxic edema) - **Normal MRA** (patent vertebral and basilar arteries) = rules out large-vessel occlusion - **Normal NCCT** = excludes hemorrhage and posterior fossa mass The small DWI lesion in the cerebellum with patent major vessels indicates **small-vessel occlusion** (likely atherosclerotic or embolic to a small PICA branch). ## Differential Diagnosis Reasoning ```mermaid flowchart TD A[Acute cerebellar/brainstem syndrome]:::outcome --> B{DWI lesion location?}:::decision B -->|Cerebellar hemisphere| C[PICA territory infarction]:::action B -->|Lateral medulla| D[Wallenberg syndrome]:::action B -->|Pons| E[AICA territory infarction]:::action C --> F[Check MRA for vertebral patency]:::decision F -->|Patent| G[Small-vessel PICA occlusion]:::outcome F -->|Occluded| H[Vertebral artery dissection or thrombosis]:::urgent ``` **Clinical Pearl:** Cerebellar infarction can rapidly deteriorate due to **edema and mass effect**, potentially causing obstructive hydrocephalus and brainstem compression. Close monitoring and neurosurgical consultation may be needed if edema progresses. ## Why DWI is Superior Here - NCCT is **normal** in 80% of acute posterior circulation strokes in the first 24 hours - DWI detects infarction within **minutes**, enabling early intervention - MRA simultaneously assesses large-vessel patency and guides management (thrombolysis vs. antiplatelet therapy) 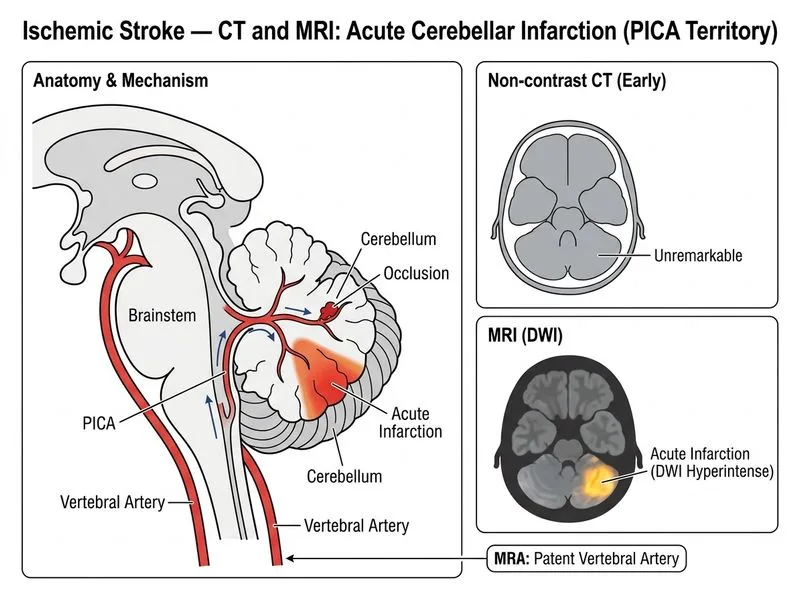
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.