## Clinical Context This is a case of **asymmetric IUGR** (AC <10th centile, normal AFV, normal amniotic fluid) with evidence of **placental insufficiency** (elevated umbilical artery PI). The fetus is at 32 weeks with abnormal Doppler findings but no signs of fetal distress on CTG. ## Management Algorithm for IUGR with Abnormal Umbilical Artery Doppler ```mermaid flowchart TD A[IUGR diagnosed on ultrasound]:::outcome --> B{Umbilical artery Doppler}:::decision B -->|Normal| C[Expectant management<br/>Weekly monitoring]:::action B -->|Elevated PI/RI<br/>but diastolic flow present| D{Gestational age?}:::decision D -->|< 34 weeks| E[Admit for close monitoring<br/>Twice-weekly CTG + Doppler<br/>Corticosteroids]:::action D -->|≥ 34 weeks| F[Deliver after corticosteroids]:::action B -->|Absent/Reversed<br/>diastolic flow| G[Deliver immediately<br/>Cesarean section]:::urgent E --> H{Deterioration on monitoring?}:::decision H -->|Yes| I[Deliver immediately]:::urgent H -->|No| J[Continue monitoring<br/>Deliver at 34 weeks]:::action ``` ## Key Decision Points **High-Yield:** - **Umbilical artery PI 1.8** is elevated but **diastolic flow is still present** (not absent/reversed) - At **32 weeks** with abnormal but not critically abnormal Doppler, expectant management with intensive monitoring is standard - **Corticosteroids** should be given for fetal lung maturity - **Delivery planned at 34 weeks** or earlier if signs of fetal compromise emerge **Key Point:** - Absent or reversed end-diastolic flow (AREDF) in umbilical artery is an indication for **immediate delivery** regardless of gestational age - Elevated PI with preserved diastolic flow allows for **expectant management** with close surveillance ## Why Expectant Management Here? 1. **Gestational age 32 weeks** — morbidity/mortality from prematurity still significant 2. **Preserved diastolic flow** — indicates compensatory mechanisms still intact 3. **No acute fetal distress** — CTG normal, decreased movements may be constitutional 4. **Twice-weekly monitoring** allows early detection of deterioration 5. **Corticosteroids** reduce neonatal respiratory distress and intraventricular hemorrhage ## When to Deliver Immediately - Absent or reversed diastolic flow in umbilical artery - Abnormal ductus venosus Doppler (reversed flow in atrial contraction phase) - Repetitive late decelerations or prolonged bradycardia on CTG - Maternal hypertension crisis or preeclampsia with severe features [cite:Williams Obstetrics 26e Ch 42] [cite:RCOG Green-top Guideline 31] 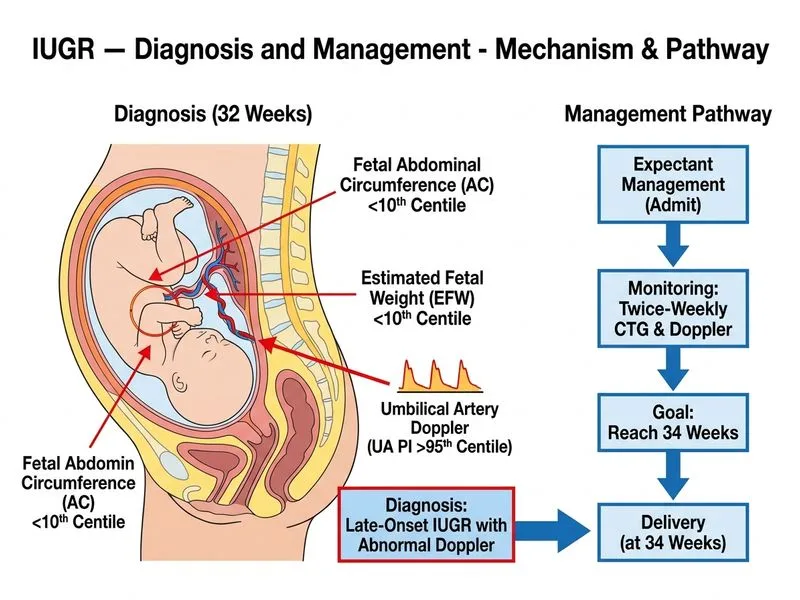
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.