## Investigation of Choice for Assessing Placental Insufficiency Severity in IUGR ### Clinical Context This patient has **early-onset IUGR (EOFR) at 28 weeks** with maternal hypertension (likely preeclampsia) and abnormal umbilical artery Doppler (elevated PI with preserved AEDF). The next critical step is to assess **fetal compensation and predict risk of decompensation**. ### Rationale for Correct Answer **Key Point:** In early-onset IUGR with abnormal UA Doppler, **cerebroplacental ratio (CPR) and venous Doppler assessment** are the most appropriate investigations to: 1. **Quantify fetal compensation:** CPR = MCA PI / UA PI. A normal CPR (>1.0) indicates preserved brain-sparing; CPR <1.0 signals loss of cerebral autoregulation and imminent fetal decompensation. 2. **Detect late decompensation signs:** Abnormal venous Doppler (reversed ductus venosus [DV] flow, absent umbilical vein pulsations) indicates severe placental insufficiency and fetal acidosis; these mandate delivery regardless of gestational age. 3. **Guide delivery timing:** - **CPR >1.0 + normal venous Doppler** → intensive surveillance, consider delivery at 32–34 weeks. - **CPR <1.0** → delivery at 30–32 weeks (if steroids given). - **Abnormal venous Doppler** → delivery within 48 hours (give steroids + magnesium sulphate if <34 weeks). 4. **Predict adverse outcomes:** Abnormal CPR and venous Doppler correlate with neonatal acidosis, NICU admission, and perinatal mortality. ### Doppler Algorithm in Early-Onset IUGR ```mermaid flowchart TD A[IUGR at <34 weeks<br/>Elevated UA PI]:::outcome --> B{MCA PI and CPR?}:::decision B -->|CPR >1.0<br/>Normal MCA| C[Brain-sparing present]:::outcome B -->|CPR <1.0<br/>Decreased MCA| D[Loss of autoregulation]:::urgent C --> E{Venous Doppler?}:::decision E -->|Normal DV<br/>Normal UV| F[Intensive surveillance<br/>Deliver at 32-34 weeks]:::action E -->|Abnormal DV<br/>or absent UV pulsations| G[Severe decompensation]:::urgent D --> H[High-risk group<br/>Deliver at 30-32 weeks]:::action G --> I[Deliver within 48 hours<br/>Give steroids + MgSO4]:::urgent ``` ### Doppler Thresholds in IUGR | Parameter | Normal | Mild IUGR | Severe IUGR | |---|---|---|---| | **UA PI** | <1.4 | 1.4–2.0 | >2.0 or ARED | | **MCA PI** | >1.5 | >1.5 | <1.5 | | **CPR** | >1.0 | >1.0 | <1.0 | | **DV flow** | Normal a-wave | Normal a-wave | Reversed a-wave | | **UV pulsations** | Absent (normal) | Absent | Present (abnormal) | **High-Yield:** In early-onset IUGR, **CPR <1.0 is the single best predictor of adverse neonatal outcome** and mandates delivery at 30–32 weeks (after steroids). **Abnormal venous Doppler** (reversed DV flow, pulsatile UV) indicates fetal acidosis and requires delivery within 48 hours. **Clinical Pearl:** A fetus with elevated UA PI but **preserved CPR and normal venous Doppler** can be managed expectantly with twice-weekly Doppler surveillance until 34 weeks, reducing unnecessary preterm delivery. **Mnemonic: VENOUS DOPPLER SEVERITY** — **V**enosus (ductus) reversed, **E**nd-diastolic flow absent (UA), **N**ormal MCA lost, **O**xygen deprivation imminent, **U**mbilical vein pulsatile, **S**evere acidosis likely. --- ## Why Each Distractor Is Wrong ### Distractor 0: Maternal urine protein estimation and liver function tests - **Reason:** While these tests assess maternal preeclampsia severity (relevant for maternal management), they do NOT assess fetal placental insufficiency or predict fetal decompensation. Fetal Doppler studies, not maternal labs, determine the urgency of delivery in IUGR. Maternal preeclampsia severity and fetal IUGR severity are discordant; a severely preeclamptic mother may have a mildly growth-restricted fetus with preserved Doppler. ### Distractor 2: Fetal echocardiography to rule out cardiac anomalies - **Reason:** Fetal echocardiography is indicated if structural cardiac anomalies are suspected (e.g., on standard ultrasound, family history of congenital heart disease, or syndromic features). In isolated IUGR with abnormal UA Doppler, echocardiography does not assess placental insufficiency severity or guide delivery timing. It is not the next appropriate investigation. ### Distractor 3: Cordocentesis for fetal blood gas analysis - **Reason:** Cordocentesis is an invasive procedure with miscarriage risk (1–2%) and is rarely used in modern practice. Non-invasive Doppler ultrasound (CPR, venous Doppler) provides equivalent prognostic information without fetal risk. Cordocentesis is reserved for specific indications (e.g., suspected fetal infection, isoimmunization) and is not indicated for IUGR assessment. --- ## Clinical Summary **Key Point:** In early-onset IUGR with abnormal UA Doppler, the investigation of choice is **cerebroplacental ratio (CPR) and venous Doppler assessment**. This combination: - Quantifies fetal compensation (CPR >1.0 = preserved; <1.0 = lost). - Detects late decompensation (reversed DV flow, pulsatile UV). - Guides delivery timing (CPR <1.0 or abnormal venous Doppler → earlier delivery). - Predicts neonatal outcomes (acidosis, NICU admission, mortality). [cite:Williams Obstetrics 26e Ch 42; RCOG Green-top Guideline 31] 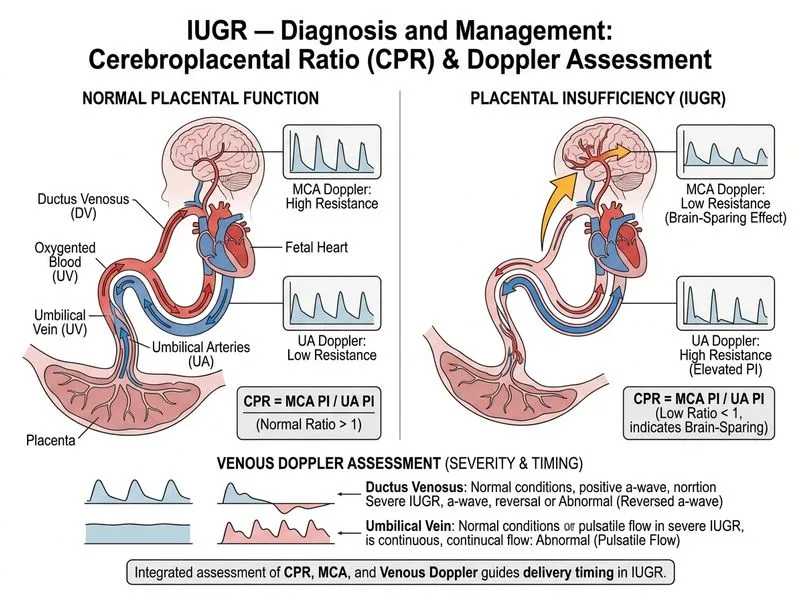
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.