## Management of Severe IUGR with Abnormal Doppler and Preeclampsia ### Clinical Scenario: High-Risk Features | Finding | Severity | Implication | |---------|----------|-------------| | AEDF in UA | Severe placental insufficiency | High risk of stillbirth and neonatal death | | Oligohydramnios (AFI 6) | Moderate | Indicates fetal compromise | | Preeclampsia (BP 148/96 + 2+ proteinuria) | Severe | Maternal and fetal risk escalated | | 32 weeks gestation | Preterm | Neonatal morbidity significant but manageable | | Normal FHR variability | Reassuring | No acute fetal distress at this moment | **Key Point:** The combination of **AEDF + oligohydramnios + preeclampsia at 32 weeks** is a **high-risk scenario requiring urgent delivery**, but not immediate cesarean section in a stable fetus with normal heart rate variability. ### Pathophysiology of AEDF **High-Yield:** Absent end-diastolic flow (AEDF) indicates: - Increased placental resistance - Severely reduced placental perfusion - Risk of intrauterine death: **5–10% if expectant management** - Neonatal mortality: **10–15%** if delivered at 32 weeks (but survivable with NICU support) ### Management Algorithm for AEDF at 32 Weeks ```mermaid flowchart TD A[AEDF + Oligohydramnios + Preeclampsia at 32 weeks]:::outcome A --> B{Fetal Status Stable?}:::decision B -->|Yes - normal HR variability| C[Admit for inpatient monitoring]:::action B -->|No - abnormal variability/decelerations| D[Immediate cesarean section]:::urgent C --> E[Administer betamethasone]:::action E --> F[Plan delivery within 48 hours]:::action F --> G[Delivery by 32+2 weeks]:::action G --> H[Neonatal intensive care]:::outcome ``` ### Rationale for 48-Hour Window 1. **Corticosteroid benefit**: Betamethasone reduces neonatal mortality by ~30% and RDS by ~40% when given 24 hours before delivery 2. **Fetal maturation**: Even 48 hours at 32 weeks improves outcomes (lung maturity, IVH risk) 3. **Maternal stabilization**: Allows time to optimize BP control and assess for eclampsia 4. **Fetal monitoring**: Continuous CTG to detect acute deterioration (loss of variability, repetitive decelerations) → immediate delivery **Clinical Pearl:** AEDF is an indication for **delivery within 48–72 hours** in a stable fetus. If fetal heart rate variability becomes abnormal or decelerations appear, deliver **immediately by cesarean section**. ### Why NOT Immediate Cesarean Section? - Fetal heart rate is **normal (140 bpm) with normal variability** — no sign of acute distress - Immediate delivery denies the benefit of corticosteroids (which require 24 hours to act) - 48-hour delay allows fetal maturation with acceptable risk (AEDF is chronic, not acute) - Maternal preeclampsia is severe but not yet eclamptic; inpatient monitoring is safe **Warning:** If at any point during inpatient monitoring the fetus develops **loss of variability, repetitive late decelerations, or bradycardia**, delivery must be expedited immediately. [cite:RCOG Green-top Guideline 31; ACOG Practice Bulletin 204 — Fetal Growth Restriction] 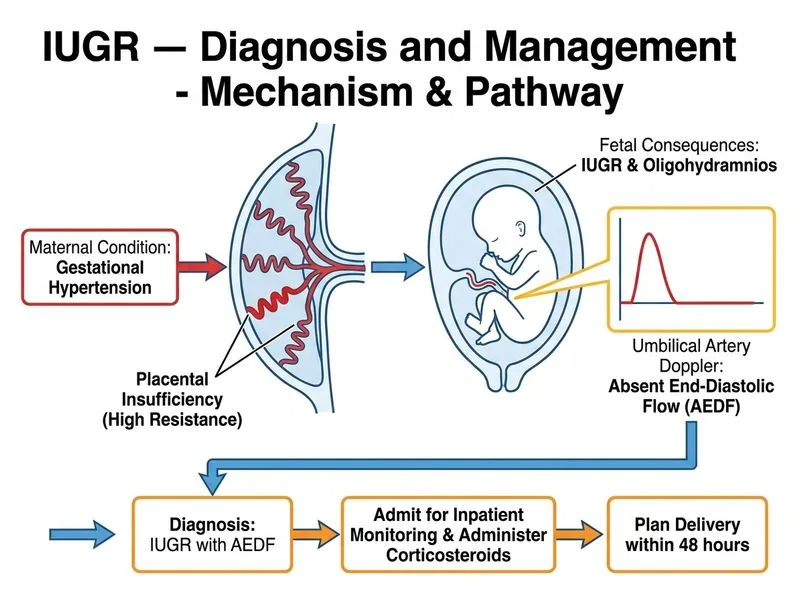
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.