## Clinical Context This patient presents with **early-onset IUGR (< 34 weeks)** with **abnormal umbilical artery Doppler** (elevated PI of 1.8 vs. normal < 1.2) and a **borderline cerebroplacental ratio of 1.1** (normal > 1.0 — technically still within normal limits but at the lower boundary). The key management decision hinges on gestational age (32 weeks), abnormal UA Doppler, and the absence of immediate delivery triggers (no absent/reversed end-diastolic flow, no severe fetal compromise). ## Diagnosis of IUGR **Key Point:** IUGR is diagnosed when estimated fetal weight is < 10th percentile for gestational age. This patient's EFW of 1400 g at 32 weeks confirms IUGR. Decreased fetal movements and a fundal height 4 cm below expected further support placental insufficiency. ## Doppler Interpretation | Doppler Parameter | Significance | Clinical Action | |---|---|---| | Normal UA PI | Reassuring | Expectant management, weekly surveillance | | Elevated UA PI (abnormal, no AREDF) | Placental insufficiency | Steroids + plan delivery at 34 weeks | | Absent/Reversed UA diastolic flow | Severe compromise | Deliver immediately (after steroids if time permits) | | CPR < 1.0 | Fetal hypoxemia / brain-sparing | Expedite delivery | | CPR 1.0–1.2 (borderline) | Early redistribution | Intensify surveillance; plan delivery at 34 weeks | **High-Yield:** In early-onset IUGR (< 34 weeks) with **elevated UA PI but intact end-diastolic flow** and a **borderline (not clearly abnormal) CPR**, the standard of care per RCOG Green-top Guideline No. 31 and ACOG Practice Bulletin No. 204 is: 1. **Administer antenatal corticosteroids (betamethasone 12 mg IM × 2 doses, 24 hours apart)** to accelerate fetal lung maturity. 2. **Plan delivery at 34 weeks** (or earlier if further Doppler deterioration — absent/reversed EDF, biophysical profile ≤ 4, or maternal deterioration). This strategy balances the risks of prematurity at 32 weeks (severe RDS, IVH, NEC) against the risk of ongoing placental insufficiency. ## Important Clarification on CPR The SME correctly noted that a CPR of **1.1 is borderline, not clearly abnormal** (threshold < 1.0). The original explanation incorrectly stated CPR < 1.0 as a finding in this case. The CPR here is 1.1 — technically normal but at the lower limit. This does **not** trigger immediate delivery; it reinforces the need for close surveillance and planned delivery at 34 weeks after steroid administration. ## Management Algorithm - **Abnormal UA PI + intact EDF + CPR borderline (1.0–1.2) at 32 weeks** → Betamethasone + plan delivery at 34 weeks ✅ - **Absent/Reversed EDF or CPR < 1.0 or BPP ≤ 4** → Immediate delivery (after steroids if feasible) - **Normal UA PI** → Weekly CTG + Doppler, deliver at 37 weeks **Clinical Pearl (RCOG / ACOG):** Betamethasone administration is mandatory before planned preterm delivery < 34 weeks to reduce neonatal RDS, IVH, and necrotizing enterocolitis. Delivering at 32 weeks without steroids (option B) unnecessarily exposes the neonate to severe morbidity. ## Why Not Other Options? - **Option A — Expectant management with twice-weekly CTG/Doppler alone:** Inappropriate because the UA PI is clearly elevated (1.8 vs. normal < 1.2), indicating active placental insufficiency. Passive surveillance without a delivery plan risks sudden fetal deterioration. - **Option B — Immediate cesarean at 32 weeks:** Premature without corticosteroid cover. At 32 weeks, the risks of severe RDS and IVH are substantial. Immediate delivery is reserved for absent/reversed EDF, BPP ≤ 4, or severe maternal compromise — none of which are present here. - **Option D — Fetal blood sampling (FBS):** Largely obsolete in modern obstetric practice. Doppler velocimetry (UA PI, MCA PI, CPR, ductus venosus) has replaced FBS as the gold standard for fetal surveillance in IUGR (RCOG 2013; Lees et al., TRUFFLE trial). **Key Point (KD Tripathi / Dutta's Obstetrics):** In early-onset IUGR with abnormal but not critically deranged Doppler, the goal is to gain fetal lung maturity with corticosteroids and deliver at 34 weeks — the gestational age at which neonatal outcomes improve substantially. 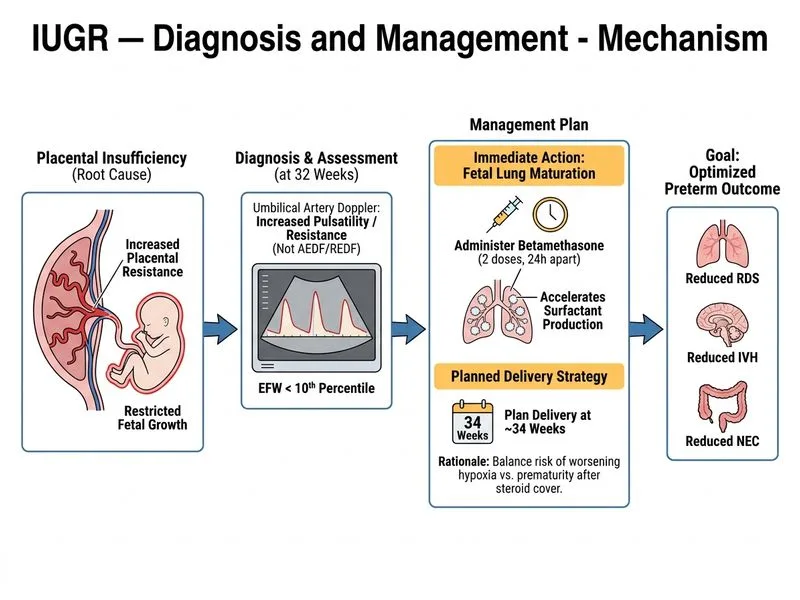
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.