## Clinical Context This is a case of **severe IUGR with abnormal umbilical artery Doppler** (absent end-diastolic flow indicates placental insufficiency) at 32 weeks gestation. ## Key Diagnostic Features - **Fundal height < gestational age** → clinical suspicion of IUGR - **Estimated fetal weight < 10th centile** → confirmed IUGR - **AEDF on umbilical artery Doppler** → severe placental dysfunction, high risk of intrauterine fetal death (IUFD) and neonatal complications - **Normal amniotic fluid** → rules out oligohydramnios (which would further worsen prognosis) ## Management Algorithm for IUGR with Abnormal Doppler ```mermaid flowchart TD A[IUGR confirmed + Abnormal UA Doppler]:::outcome --> B{Gestational age?}:::decision B -->|< 24 weeks| C[Offer counseling: poor prognosis]:::action B -->|24-34 weeks| D[Admit for close monitoring]:::action D --> E[Administer corticosteroids]:::action E --> F[Continuous CTG monitoring]:::action F --> G{Signs of fetal distress or<br/>further deterioration?}:::decision G -->|Yes| H[Deliver immediately]:::urgent G -->|No| I[Plan delivery at 34 weeks<br/>or earlier if deterioration]:::action B -->|≥ 34 weeks| J[Deliver within 24-48 hours]:::action ``` **Key Point:** At 32 weeks with AEDF, the risk of IUFD is significant (~5–10% per week). The standard approach is **admission for continuous fetal monitoring + corticosteroids + planned delivery at 34 weeks** unless there is acute deterioration (abnormal CTG, reverse flow in umbilical vein, reverse flow in ductus venosus), which mandates immediate delivery. **High-Yield:** AEDF is an ominous sign. The fetus is at high risk of sudden death in utero. Expectant management beyond 34 weeks is NOT recommended; delivery should occur by 34 weeks at the latest unless there is earlier deterioration. **Clinical Pearl:** Corticosteroids (betamethasone 12 mg IM × 2 doses, 24 hours apart) are given to accelerate fetal lung maturity, improving neonatal outcomes. This is standard of care even in IUGR with abnormal Doppler, as it reduces respiratory distress syndrome, intraventricular hemorrhage, and neonatal mortality. ## Why NOT Immediate Delivery at 32 Weeks? - At 32 weeks, a 2-week course of corticosteroids significantly improves neonatal morbidity and mortality. - Immediate delivery without corticosteroids exposes the neonate to higher risk of respiratory distress, intraventricular hemorrhage, and death. - If the fetus remains stable on continuous monitoring, waiting until 34 weeks (after corticosteroids) is justified. ## Why NOT Delay Until 37 Weeks? - AEDF is a sign of severe placental insufficiency; the risk of IUFD increases with each passing week. - Waiting until 37 weeks is inappropriate and increases perinatal mortality. - Antihypertensive therapy is irrelevant here (no mention of maternal hypertension). 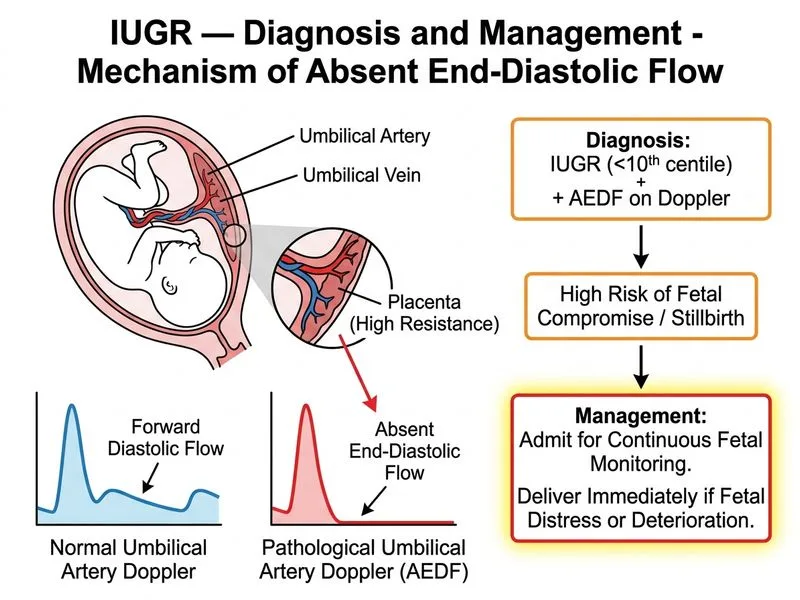
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.