## Clinical Scenario Analysis This case represents **pathological IUGR with placental insufficiency** in the context of maternal hypertension: - Fetal weight at 3rd percentile (severe IUGR) - **Oligohydramnios** (AFI 6 cm; normal >8 cm) - **Abnormal Doppler:** elevated pulsatility index (PI) with preserved end-diastolic flow (EDF) - Reassuring CTG (normal rate, normal variability) ## Doppler Classification and Prognostic Significance | Doppler Pattern | Significance | Management | |---|---|---| | Normal PI/RI | Low risk | Expectant; weekly surveillance | | **Elevated PI with preserved EDF** | **Moderate risk; early placental insufficiency** | **Inpatient monitoring; deliver ≥34 weeks** | | Absent end-diastolic flow (AEDF) | High risk; severe insufficiency | Deliver ≥32 weeks or urgent if <32 weeks | | Reversed end-diastolic flow (REDF) | Critical; fetal decompensation imminent | Urgent delivery regardless of gestation | **Key Point:** Elevated PI with preserved EDF represents **early-stage placental insufficiency** and warrants intensified surveillance but does not mandate immediate delivery if CTG is reassuring and gestation is <34 weeks. ## Management Strategy at 29 Weeks with Abnormal Doppler ```mermaid flowchart TD A["IUGR + Oligohydramnios<br/>+ Abnormal Doppler<br/>at 29 weeks"]:::outcome --> B{"CTG reassuring?"}:::decision B -->|Yes| C["Administer betamethasone<br/>Admit for inpatient monitoring"]:::action C --> D["Daily CTG<br/>Repeat Doppler in 3-4 days"]:::action D --> E{"Deterioration?<br/>AEDF/REDF/FHR abnormality?"}:::decision E -->|Yes| F["Deliver immediately"]:::urgent E -->|No| G["Continue monitoring<br/>Plan delivery at 34 weeks"]:::action B -->|No| H["Urgent delivery"]:::urgent ``` **High-Yield:** The presence of **preserved end-diastolic flow** (not absent or reversed) with a reassuring CTG permits expectant management until 34 weeks, provided there is **inpatient monitoring** with daily CTG and repeat Doppler in 3–4 days to detect progression. ## Rationale for Inpatient Admission 1. **Oligohydramnios + abnormal Doppler:** Risk of acute deterioration (loss of EDF, reversed flow, or FHR decelerations) is significant. 2. **Betamethasone:** Indicated because delivery may be necessary before 34 weeks if fetal condition worsens; fetal lung maturity is critical at 29 weeks. 3. **Daily CTG:** Detects FHR abnormalities (loss of variability, decelerations) that would prompt immediate delivery. 4. **Repeat Doppler in 3–4 days:** Identifies progression to AEDF or REDF, which mandates delivery regardless of gestation. 5. **Planned delivery at 34 weeks:** If stable, delivery at 34 weeks reduces neonatal morbidity while allowing fetal maturation. **Clinical Pearl:** The transition from preserved to absent/reversed EDF can occur over days to weeks; inpatient surveillance is essential to capture this change and avoid fetal death *in utero*. [cite:RCOG Green-top Guideline 31; Cunningham Obstetrics 26e Ch 42] 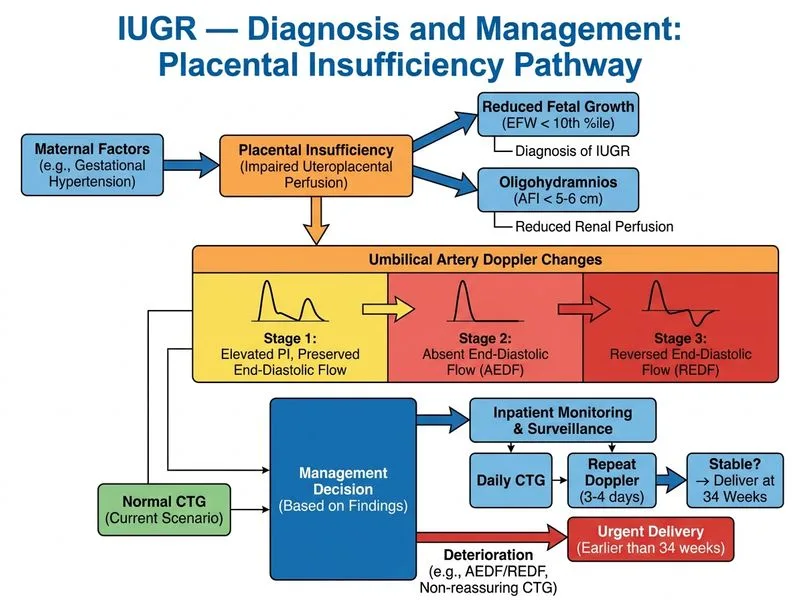
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.