## Early vs. Late Pathological IUGR: The Role of Diastolic Flow ### Key Discriminator: Preservation of End-Diastolic Velocity (EDV) **Key Point:** The presence of preserved end-diastolic velocity (EDV) in the umbilical artery, despite elevated PI, is the critical discriminator between early-stage IUGR (still compensated) and late-stage IUGR with severe placental insufficiency. Preserved EDV indicates the fetus is still tolerating placental insufficiency; absent or reversed EDV (AEDV/REDV) signals decompensation and imminent fetal compromise. ### Doppler Progression in Pathological IUGR ```mermaid flowchart TD A["Placental Insufficiency Begins"]:::outcome --> B["Elevated UA PI<br/>Preserved EDV"]:::action B --> C{"Fetal Compensation<br/>Adequate?"}:::decision C -->|"Yes<br/>Early IUGR"| D["Normal MCA Doppler<br/>Normal CPR"]:::action C -->|"No<br/>Decompensation"| E["Absent EDV<br/>AEDV/REDV"]:::urgent E --> F["Brain Sparing<br/>Elevated MCA PSV"]:::urgent E --> G["Abnormal CPR<br/>High perinatal risk"]:::urgent D --> H["Serial monitoring<br/>Delivery at 34-37 wks"]:::action G --> I["Urgent delivery<br/>Consider <34 wks if severe"]:::urgent ``` ### Comparison Table: Early vs. Late Pathological IUGR | Parameter | Early-Stage IUGR | Late-Stage IUGR (Severe) | | --- | --- | --- | | **UA PI** | Elevated (>1.3) | Markedly elevated (>2.0) | | **UA EDV** | **Preserved** | **Absent or reversed** | | **MCA Doppler** | Normal PSV | Elevated PSV (brain sparing) | | **Cerebroplacental Ratio** | Normal (>1.08) | Abnormal (<1.08) | | **Ductus Venosus** | Normal | Abnormal (reversed flow) | | **Amniotic Fluid** | May be normal or reduced | Usually oligohydramnios | | **Fetal Status** | Compensated, stable | Decompensated, at risk | | **Delivery Timing** | 34–37 weeks | <34 weeks or urgent | | **Perinatal Mortality** | Low (1–2%) | High (10–20%) | ### Hemodynamic Interpretation **Preserved EDV in UA:** - Indicates diastolic flow continues throughout the cardiac cycle - Reflects that placental vascular resistance, though elevated, has not reached critical levels - Fetus is still perfusing vital organs (brain, heart, kidneys) - Compensatory mechanisms (brain sparing) have NOT yet activated - Prognosis: relatively stable if monitored; delivery can be planned at 34–37 weeks **Absent or Reversed EDV (AEDV/REDV):** - Indicates diastolic flow has ceased or reversed - Reflects severe placental vascular obstruction - Fetus has exhausted compensatory capacity - Brain-sparing response is active (elevated MCA PSV, abnormal CPR) - Prognosis: high risk of fetal compromise; urgent delivery indicated **High-Yield:** The transition from preserved to absent EDV marks the shift from early (compensated) to late (decompensated) IUGR. This is the single most important Doppler threshold in IUGR management and determines delivery timing. **Clinical Pearl:** A fetus with elevated UA PI but preserved EDV can be managed expectantly with intensive surveillance (twice-weekly NST, twice-weekly Doppler). Once EDV is lost, delivery should be expedited (within 48 hours if >34 weeks; consider steroids and delivery at 32–34 weeks if <34 weeks with severe findings). ### Why Other Features Are Not Discriminators - **Elevated UA PI with normal MCA:** This pattern alone does not distinguish early from late IUGR; the key is whether EDV is preserved - **Oligohydramnios:** While more common in late IUGR, it can occur in early IUGR and is not a reliable discriminator - **Maternal hypertension:** The etiology does not predict the stage of IUGR; hypertensive IUGR can present at any stage 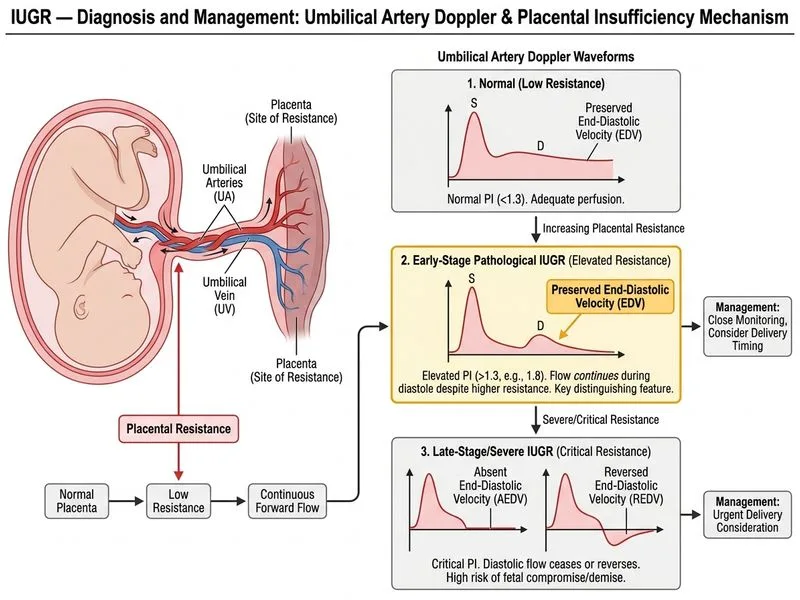
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.