## Investigation of Choice for Suspected Cirrhosis ### Clinical Context The patient presents with: - Chronic alcohol use (10 years) - Clinical signs of portal hypertension (ascites, hepatomegaly) - Predominantly conjugated hyperbilirubinemia (3.1/4.2 mg/dL) - AST:ALT ratio >1.5 (95:58), classic for alcoholic liver disease - Synthetic dysfunction (prolonged PT) This constellation strongly suggests **alcoholic cirrhosis with decompensation**. ### Why Liver Biopsy with Histopathology? **Key Point:** Liver biopsy remains the **gold standard** for: 1. **Confirming cirrhosis** — histological demonstration of bridging fibrosis and regenerative nodules (Metavir F4 / Ishak stage 5–6) 2. **Assessing severity** — fibrosis staging, degree of inflammation, steatohepatitis activity 3. **Identifying etiology** — alcoholic hepatitis features (Mallory-Denk bodies, pericellular fibrosis, neutrophilic infiltrate) 4. **Ruling out superimposed pathology** — e.g., hepatocellular carcinoma, drug-induced injury Per **Harrison's Principles of Internal Medicine (21st ed.)** and **Sherlock's Diseases of the Liver and Biliary System**, liver biopsy is the definitive investigation when the diagnosis of cirrhosis needs histological confirmation and severity grading is required. **High-Yield:** The question specifically asks to "confirm the suspected diagnosis AND assess its severity" — only histopathology achieves both simultaneously. Non-invasive imaging (ultrasound, CT) can suggest cirrhosis but cannot stage fibrosis or confirm the diagnosis histologically. ### Important Note on Bleeding Risk The SME correctly notes that prolonged PT increases bleeding risk with biopsy. In clinical practice, this is managed by: - Correcting coagulopathy (FFP, vitamin K) before the procedure - Using the **transjugular route** (TJLB) when PT is significantly prolonged — this avoids the peritoneal cavity and allows simultaneous HVPG measurement The question asks for the investigation to **confirm and assess severity**, not the safest first-line screening tool — making liver biopsy the correct answer. ### Why Not the Other Options? | Investigation | Role | Limitation | |---|---|---| | **Abdominal ultrasound + Doppler** | First-line screening; detects coarse echotexture, portal hypertension, ascites | Cannot confirm cirrhosis histologically; cannot stage fibrosis | | **CT abdomen with contrast** | Better for HCC detection, vascular anatomy | Second-line imaging; still cannot provide histological diagnosis or fibrosis staging | | **ERCP** | For biliary obstruction (dilated ducts, stones) | Not indicated here; no evidence of biliary obstruction; carries pancreatitis risk | **Clinical Pearl:** While ultrasound is the **first-line imaging** in the workup of jaundice, the question asks specifically for the investigation to **confirm** cirrhosis and **assess its severity** — a distinction that points unambiguously to liver biopsy (Harrison's, 21st ed., Chapter on Cirrhosis). ### Diagnostic Algorithm ``` Jaundice + Clinical cirrhosis features ↓ Ultrasound (screening, rule out obstruction) ↓ Liver Biopsy (confirm diagnosis + fibrosis staging) ↓ [If PT prolonged → Transjugular liver biopsy] ↓ Endoscopy (variceal surveillance if decompensated) ``` **Tip:** Remember the distinction between "first-line screening" (ultrasound) and "gold standard for confirmation and severity assessment" (liver biopsy) — NEET PG frequently tests this nuance. 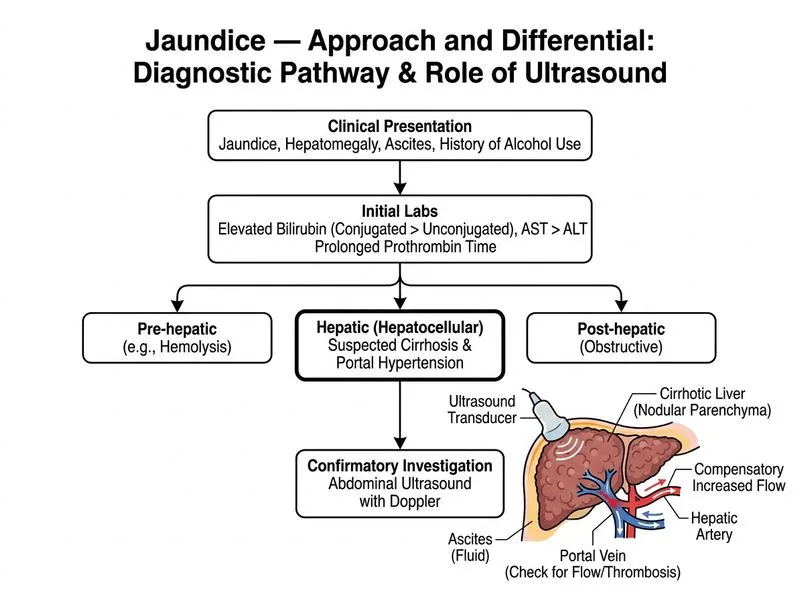
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.