## Clinical Context This patient has **hepatocellular (hepatic) jaundice** secondary to alcoholic cirrhosis. The clinical picture — 20-year alcohol history, ascites, spider angiomata, AST:ALT ratio >2 (120:45), low albumin (2.8 g/dL), and no ductal dilatation on ultrasound — confirms hepatocellular dysfunction with portal hypertension. ## Key Point: **In cirrhotic jaundice without biliary obstruction, the immediate priority is risk stratification for variceal bleeding and initiation of non-selective beta-blockers if indicated.** ERCP and PTC are reserved for obstructive (cholestatic) jaundice with dilated intrahepatic/extrahepatic ducts — neither is present here. ## High-Yield: The AST:ALT ratio >2 is a classic marker of alcoholic liver disease. In established cirrhosis, hyperbilirubinemia is typically **mixed** (both conjugated and unconjugated), reflecting impaired hepatic uptake, conjugation, and excretion. A predominantly unconjugated pattern may be seen in earlier or less severe hepatocellular dysfunction; in advanced cirrhosis, conjugated fraction often rises as well. Regardless of the bilirubin fractionation, the absence of ductal dilatation on ultrasound excludes obstructive jaundice and makes biliary intervention inappropriate. ## Management Algorithm ```mermaid flowchart TD A[Jaundiced patient]:::outcome --> B{Ultrasound findings?}:::decision B -->|Dilated ducts| C[Obstructive jaundice]:::outcome B -->|No ductal dilatation| D[Hepatic jaundice]:::outcome C --> E[ERCP ± sphincterotomy]:::action D --> F{Cirrhosis present?}:::decision F -->|Yes| G[Assess variceal risk + beta-blockers if indicated]:::action F -->|No| H[Investigate parenchymal cause]:::action ``` ## Clinical Pearl: **Variceal bleeding is the leading cause of acute mortality in cirrhosis.** All cirrhotic patients should be screened for esophageal varices by upper GI endoscopy. Non-selective beta-blockers (propranolol, nadolol, or carvedilol) are the standard of care for primary prophylaxis when medium/large varices are present or when hepatic venous pressure gradient ≥12 mmHg. They reduce portal pressure by 10–15% and prevent first variceal bleed in ~45% of high-risk patients. ## Why Not the Other Options? - **A (ERCP with sphincterotomy):** Indicated for choledocholithiasis or biliary obstruction with dilated ducts — not present here. - **B (Percutaneous transhepatic cholangiography):** Used for proximal biliary obstruction inaccessible to ERCP — no indication without ductal dilatation. - **C (Immediate liver transplantation workup):** Transplant evaluation is appropriate for end-stage liver disease, but is not the *immediate* next step; acute risk stratification (variceal bleeding) takes priority in the emergency setting. [cite: Harrison's Principles of Internal Medicine, 21e, Ch. 297; Sherlock & Dooley, Diseases of the Liver and Biliary System, 12e] 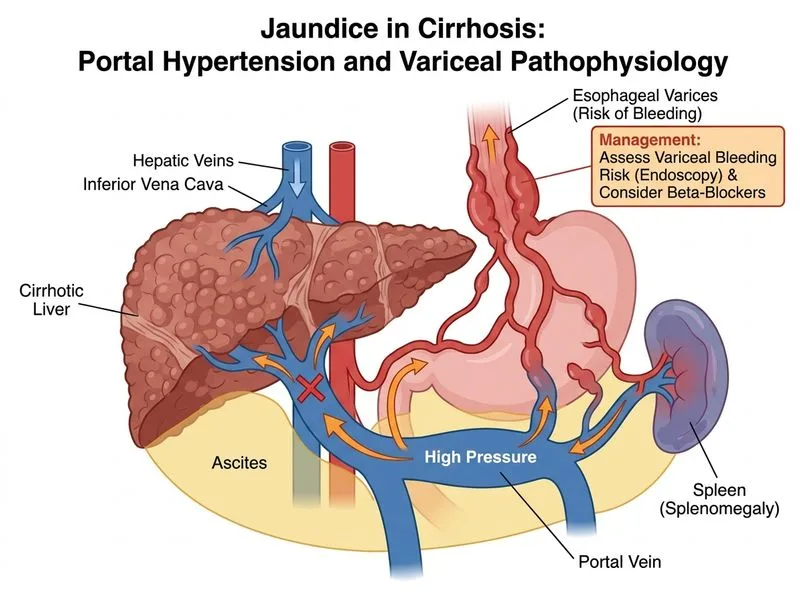
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.