## Mechanism of Jaundice in Cirrhosis ### Bilirubin Metabolism Pathway ```mermaid flowchart LR A[Heme breakdown]:::outcome --> B[Unconjugated bilirubin]:::outcome B --> C[Hepatic uptake]:::action C --> D[Conjugation by UDP-glucuronosyltransferase]:::action D --> E[Conjugated bilirubin]:::outcome E --> F[Excretion into bile]:::action F --> G[Biliary drainage]:::action H[Cirrhosis]:::urgent --> I[Hepatocellular necrosis]:::urgent I --> J[Loss of conjugating enzymes]:::urgent I --> K[Impaired synthetic function]:::urgent J --> D K --> L[↓ Albumin, ↑ PT-INR]:::outcome ``` ### Laboratory Pattern Analysis | Parameter | Value | Interpretation | |-----------|-------|----------------| | Total bilirubin | 9.5 mg/dL | Marked elevation | | Indirect bilirubin | 6.2 mg/dL (65% of total) | **Predominantly unconjugated** | | Direct bilirubin | 3.3 mg/dL (35% of total) | Mild conjugated component | | AST | 180 U/L | Hepatocellular injury | | ALT | 65 U/L | AST > ALT (alcoholic pattern) | | ALP | 95 U/L | Normal (no cholestasis) | | Albumin | 2.8 g/dL | Severe synthetic dysfunction | | PT-INR | 2.1 | Impaired coagulation synthesis | **Key Point:** The **predominance of indirect (unconjugated) bilirubin** is the diagnostic clue. This indicates impaired **conjugation**, not cholestasis or hemolysis. ### Why Reduced Conjugation? **High-Yield:** In cirrhosis, hepatocellular necrosis destroys the functional liver parenchyma and reduces the number of viable hepatocytes. This leads to: 1. **Loss of UDP-glucuronosyltransferase (UDPGT) enzyme** — the enzyme responsible for conjugating bilirubin 2. **Reduced hepatocyte mass** — fewer cells available to conjugate bilirubin 3. **Unconjugated hyperbilirubinemia** — bilirubin accumulates because it cannot be conjugated efficiently **Clinical Pearl:** The low albumin (2.8 g/dL) and elevated PT-INR (2.1) confirm severe hepatocellular synthetic dysfunction, which is the root cause of the conjugation defect. ### Differential Mechanisms in Jaundice ```mermaid flowchart TD A[Jaundice]:::outcome --> B{Bilirubin type?}:::decision B -->|Indirect > Direct| C[Unconjugated hyperbilirubinemia]:::outcome B -->|Direct > Indirect| D[Conjugated hyperbilirubinemia]:::outcome C --> E{Mechanism?}:::decision E -->|Overproduction| F[Hemolysis]:::outcome E -->|Impaired uptake| G[Gilbert syndrome, hepatitis]:::outcome E -->|Impaired conjugation| H[Cirrhosis, severe hepatitis]:::outcome D --> I{Mechanism?}:::decision I -->|Intrahepatic| J[Cholestasis, PBC, ICP]:::outcome I -->|Extrahepatic| K[Biliary obstruction]:::outcome ``` ### Why Not the Other Options? **Impaired hepatic uptake (Option A):** While cirrhosis does impair uptake, uptake defects produce only mild unconjugated hyperbilirubinemia (e.g., Gilbert syndrome: 1–3 mg/dL). This patient has severe hyperbilirubinemia (9.5 mg/dL) with significant conjugated component, indicating a downstream conjugation defect. **Cholestasis and bile duct obstruction (Option C):** Cholestasis would elevate ALP and GGT (both normal here) and produce predominantly conjugated hyperbilirubinemia. The normal ALP rules out cholestasis. **Hemolysis (Option D):** Hemolysis produces unconjugated hyperbilirubinemia but would show: - Elevated reticulocyte count - Elevated LDH, low haptoglobin - Normal or mildly elevated conjugated bilirubin - Normal liver synthetic function (albumin, PT-INR) This patient has severe synthetic dysfunction, not hemolysis. **Mnemonic:** **CHIME** — Causes of Unconjugated Hyperbilirubinemia - **C**onjugation defects (cirrhosis, severe hepatitis, Crigler-Najjar) - **H**emolysis - **I**mpaired uptake (Gilbert, Dubin-Johnson) - **M**assive overproduction (rare) - **E**xtra-hepatic (none — unconjugated is always hepatic or pre-hepatic) 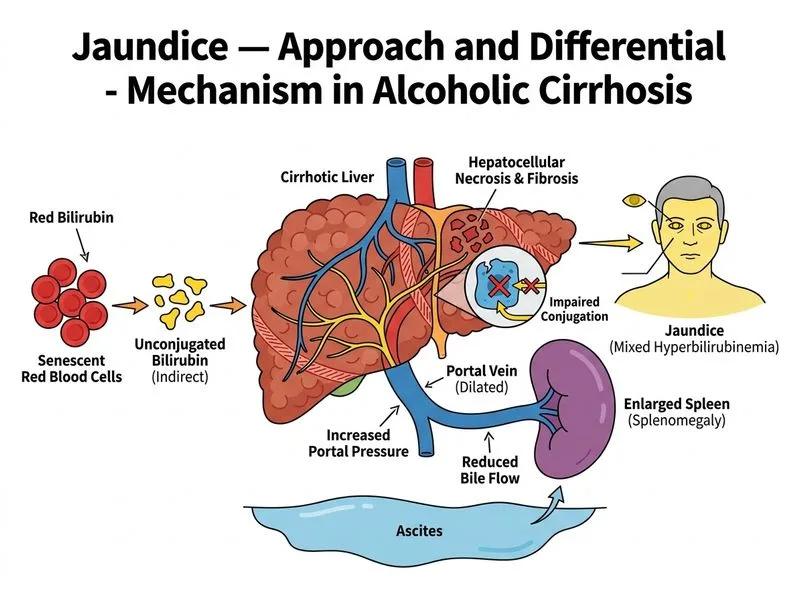
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.