## Diagnosis: Euglycemic DKA (EDKA) This patient presents with a **rare but serious** complication of SGLT2 inhibitor therapy: - Metabolic acidosis (pH 7.32, HCO₃⁻ 18) with **elevated ketones** - **Near-normal or mildly elevated glucose** (180 mg/dL, not > 250 mg/dL) - Positive urine ketones - Recent initiation of SGLT2 inhibitor (empagliflozin) - Acute illness (ACS) as a precipitant **Key Point:** This is NOT classic DKA — the glucose is not severely elevated, yet ketones are high. This is **euglycemic DKA**, a distinct entity. ## Pathophysiology: How SGLT2 Inhibitors Cause Euglycemic DKA ```mermaid flowchart TD A[SGLT2 Inhibitor]:::action --> B[Increased urinary glucose excretion]:::outcome B --> C[Osmotic diuresis]:::outcome C --> D[Volume depletion]:::outcome D --> E[Activation of counter-regulatory hormones]:::outcome E --> F[Glucagon ↑, Cortisol ↑, Catecholamines ↑]:::outcome F --> G[Lipolysis ↑]:::outcome G --> H[FFA → Hepatic β-oxidation ↑]:::outcome H --> I[Ketone body production ↑]:::outcome J[Acute stress: ACS, infection]:::urgent --> K[Further ↑ counter-regulatory hormones]:::outcome K --> G I --> L[Metabolic acidosis]:::outcome L --> M[BUT glucose remains near-normal]:::outcome M --> N[Because SGLT2 inhibitors ↓ glucose reabsorption]:::outcome N --> O[Euglycemic DKA]:::outcome ``` ## Mechanism of Ketone Accumulation in EDKA 1. **SGLT2 inhibitors** increase urinary glucose excretion → osmotic diuresis → volume depletion 2. **Volume depletion** activates the sympathetic nervous system and renin-angiotensin-aldosterone system 3. **↑ Glucagon and catecholamines** stimulate hormone-sensitive lipase → massive lipolysis 4. **Hepatic β-oxidation** of FFA increases exponentially 5. **Acetyl-CoA exceeds TCA cycle capacity** → ketogenesis accelerates 6. **β-hydroxybutyrate and acetoacetate accumulate** → metabolic acidosis 7. **BUT glucose remains near-normal** because: - SGLT2 inhibitors promote urinary glucose loss - Acute illness may suppress hepatic gluconeogenesis - Insulin (though reduced) still has some effect **Clinical Pearl:** The **absence of severe hyperglycemia despite high ketones** is the diagnostic clue to euglycemic DKA. Classic DKA presents with glucose > 250 mg/dL AND high ketones. ## Management: Why Discontinue SGLT2 Inhibitor? **High-Yield:** The SGLT2 inhibitor is the **precipitant**, not the treatment. Discontinuing it: 1. **Stops osmotic diuresis** → restores intravascular volume 2. **Reduces counter-regulatory hormone activation** → decreases lipolysis 3. **Allows insulin to work more effectively** → suppresses ketogenesis 4. **Prevents recurrence** of euglycemic DKA **Key Point:** IV insulin infusion is still needed because: - The underlying defect is still **relative insulin deficiency** (despite normal glucose) - Insulin suppresses lipolysis and ketogenesis - Insulin promotes peripheral ketone utilization - Even though glucose is near-normal, ketones are being produced at a pathological rate ## Why NOT Continue SGLT2 Inhibitor? **Warning:** Continuing the SGLT2 inhibitor would perpetuate the osmotic diuresis and volume depletion, worsening the metabolic acidosis and ketone production. The drug must be stopped immediately. 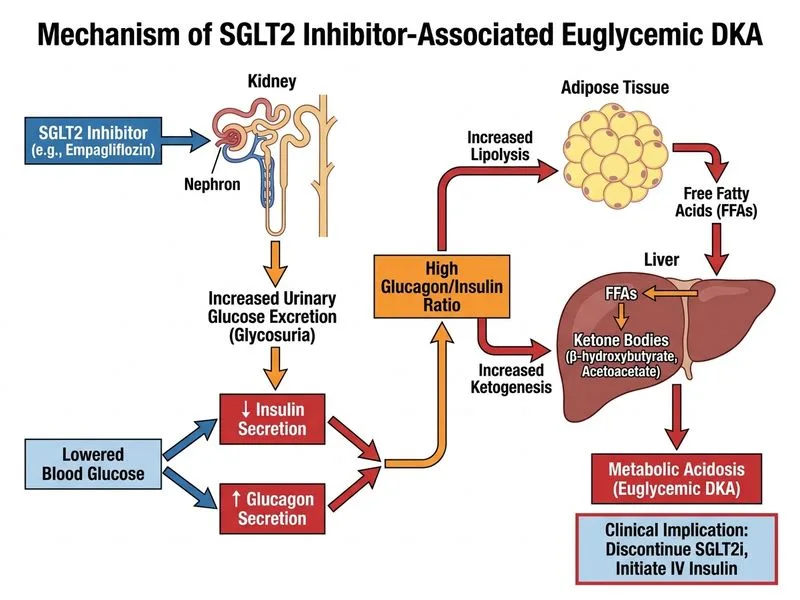
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.