## Clinical Presentation & Pathophysiology This patient has **diabetic ketoacidosis (DKA)**, a life-threatening complication of type 1 diabetes characterized by: - Severe hyperglycemia (450 mg/dL) - Metabolic acidosis (pH 7.18, HCO₃⁻ 12 mEq/L) - Elevated serum and urine ketones (β-hydroxybutyrate and acetoacetate) - Rapid breathing (Kussmaul respiration) — compensatory hyperventilation to blow off CO₂ ### Pathophysiology of Ketone Body Accumulation in DKA **Key Point:** In the absence of insulin, lipolysis accelerates uncontrollably, releasing free fatty acids (FFAs) from adipose tissue. These FFAs undergo β-oxidation in hepatic mitochondria, generating excessive acetyl-CoA. When acetyl-CoA exceeds the capacity of the TCA cycle, it is shunted into ketogenesis, producing β-hydroxybutyrate and acetoacetate. $$\text{Lipolysis} \xrightarrow{\text{no insulin}} \text{↑ FFAs} \xrightarrow{\beta\text{-oxidation}} \text{↑ Acetyl-CoA} \xrightarrow{\text{ketogenesis}} \text{Ketone bodies}$$ Unlike physiologic ketosis (fasting, low-carb diet), DKA ketosis is **uncontrolled and accompanied by severe acidosis** because ketone bodies (β-hydroxybutyrate and acetoacetate) are strong acids. ### Management Algorithm for DKA ```mermaid flowchart TD A[Suspected DKA: High glucose + Low pH + Elevated ketones]:::outcome --> B{Confirm diagnosis}:::decision B -->|Arterial pH < 7.35, HCO₃⁻ < 18| C[DKA confirmed]:::outcome C --> D[Immediate interventions]:::action D --> E[IV insulin infusion 0.1 U/kg/hr]:::action D --> F[IV fluid resuscitation: 0.9% saline]:::action D --> F --> G[Monitor K⁺, electrolytes, glucose q1-2h]:::action E --> H[Reduce insulin rate when glucose < 250 mg/dL]:::action H --> I[Continue until ketosis resolves and pH normalizes]:::action I --> J[Transition to subcutaneous insulin]:::action ``` ## Why Option 0 (Correct Answer) is Best **High-Yield:** The cornerstone of DKA management is **insulin + fluids + electrolyte monitoring**: 1. **IV Insulin Infusion (0.1 U/kg/hr):** Inhibits lipolysis → ↓ FFA mobilization → ↓ ketone production. Insulin also promotes ketone body utilization by peripheral tissues and suppresses hepatic ketogenesis. 2. **IV Fluid Resuscitation (0.9% saline):** Corrects hypovolemia, improves renal perfusion, and enhances ketone body clearance via urine. 3. **Electrolyte Monitoring:** Insulin drives K⁺ intracellularly (risk of hypokalemia); glucose correction may cause cerebral edema if too rapid (target: 50–100 mg/dL/hr). **Clinical Pearl:** Do NOT give insulin bolus in DKA — only continuous infusion. Bolus insulin can cause rapid osmotic shifts and cerebral edema. **Key Point:** Ketone bodies are cleared by the kidneys and metabolized by peripheral tissues (brain, heart, skeletal muscle). Insulin-mediated suppression of lipolysis is the primary mechanism to halt ketone production. ## Timing & Monitoring | Parameter | Frequency | Target | |-----------|-----------|--------| | Blood glucose | Every 1–2 hours | Decrease 50–100 mg/dL/hr | | Arterial pH | Every 2–4 hours | > 7.30 | | Serum K⁺ | Every 2–4 hours | 4.0–5.0 mEq/L | | Serum HCO₃⁻ | Every 2–4 hours | > 18 mEq/L | | Ketones (serum/urine) | Every 4–6 hours | Negative | ## Why Other Options Are Wrong See **whyEachDistractorIsWrong** section below. 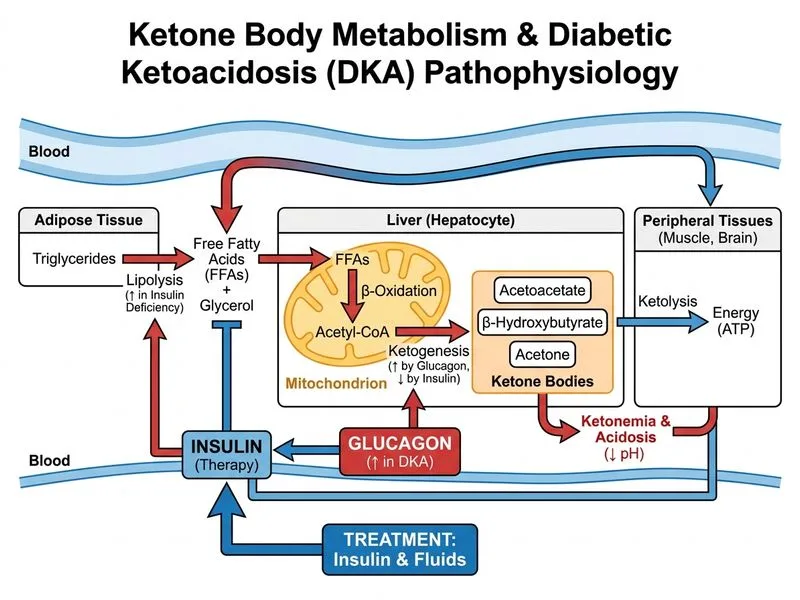
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.