## Clinical Context: Type A Lactic Acidosis in Decompensated Cirrhosis This patient has **Type A lactic acidosis** (tissue hypoperfusion/hypoxia) secondary to advanced cirrhosis with hepatic failure. The **Cori cycle is broken** — the liver cannot convert lactate back to glucose due to: 1. Severe hepatocellular dysfunction (synthetic failure) 2. Portal hypertension and splanchnic shunting 3. Hypoglycemia (glucose 68 mg/dL) indicating loss of hepatic glucose production ### Pathophysiology: Why the Cori Cycle Fails **Key Point:** In cirrhosis, lactate accumulates because the liver has **lost the enzymatic capacity** to perform gluconeogenesis and lactate clearance. Unlike exertional rhabdomyolysis (where the liver is intact but overwhelmed), cirrhotic lactic acidosis reflects **hepatic failure itself**. **High-Yield:** The Cori cycle requires: - Intact hepatic mitochondria (pyruvate carboxylase, PEPCK, glucose-6-phosphatase) - Adequate ATP and cofactors (NAD⁺, Mg²⁺) - Normal hepatic blood flow All three are compromised in decompensated cirrhosis. ### Why Dextrose Bolus is the Best Next Step | Finding | Implication | Action | |---|---|---| | **Hypoglycemia (68 mg/dL)** | Loss of hepatic glucose production; brain and RBC glucose demand unmet | **IV dextrose 50% bolus immediately** | | **Elevated lactate (6.8 mmol/L)** | Lactate clearance impaired; lactate will clear slowly as hepatic perfusion improves | Supportive care; monitor trend | | **Severe hepatic dysfunction** | Liver cannot perform Cori cycle; lactate will NOT be converted to glucose | Dextrose must be exogenous | | **Elevated ammonia + pH 7.25** | Hyperammonemia worsens CNS depression; acidosis exacerbates ammonia toxicity | Dextrose + supportive care; lactulose secondary | **Clinical Pearl:** In cirrhotic lactic acidosis, **hypoglycemia is the immediate life threat**. Dextrose bolus followed by continuous infusion (to maintain glucose 100–150 mg/dL) prevents: - Cerebral hypoglycemia and seizures - Worsening of hepatic encephalopathy (hypoglycemia impairs ammonia detoxification) - Increased lactate production (stress response) **Mnemonic: FAIL** — **F**ructose-1,6-bisphosphatase loss, **A**mmonia accumulation, **I**ncreased lactate, **L**oss of glucose production → dextrose is the bridge. ### Why Other Options Are Secondary or Wrong 1. **Sodium bicarbonate:** Alkalinization may worsen hypokalemia and does NOT address the root cause (hepatic failure). It is used only if pH < 7.15 and after dextrose/supportive care. 2. **Lactulose/rifaxomicin:** Important for ammonia reduction but do NOT correct hypoglycemia or lactate accumulation. They are adjunctive, not first-line for lactic acidosis. 3. **Liver transplant evaluation:** Correct long-term strategy, but immediate management is supportive (dextrose, fluids, monitoring) while awaiting transplant assessment. **Key Point:** Dextrose addresses the **immediate metabolic emergency** (hypoglycemia) while allowing time for hepatic perfusion to improve and lactate to clear. The Cori cycle cannot be restored in cirrhosis without liver transplant, so exogenous glucose is the only option. 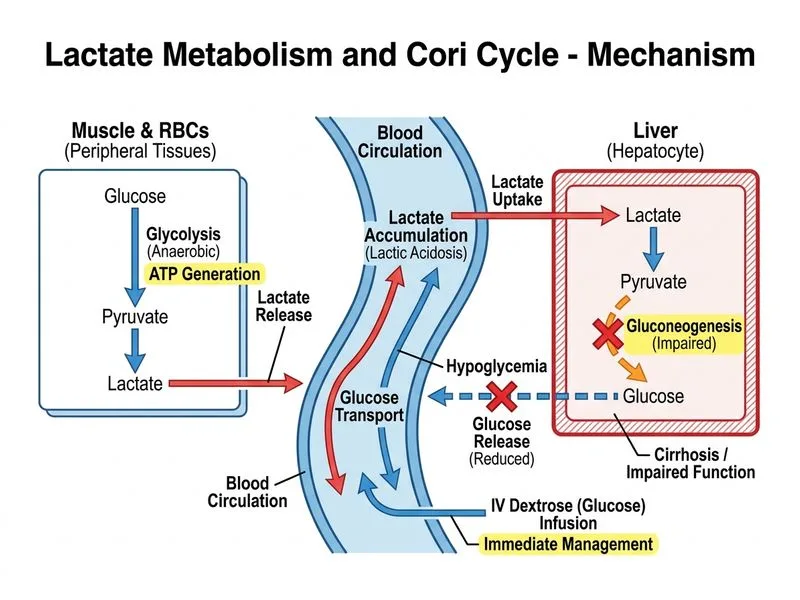
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.