## Lactate Accumulation in Cirrhosis: Impaired Cori Cycle Function ### Pathophysiology of Type B Lactic Acidosis in Liver Disease **Key Point:** Lactate accumulation in cirrhosis results from impaired hepatic clearance (lactate → pyruvate → glucose), NOT from increased production. This is **Type B lactic acidosis** — lactate accumulation without tissue hypoxia or hypoperfusion. ### Why the Liver Fails to Clear Lactate 1. **Loss of hepatocytes**: Cirrhosis destroys functional liver parenchyma, reducing the number of cells available for lactate uptake and metabolism. 2. **Reduced gluconeogenic enzyme expression**: Cirrhotic livers show downregulation of key gluconeogenic enzymes: - Lactate dehydrogenase (LDH) — reduced activity - Phosphoenolpyruvate carboxykinase (PEPCK) — suppressed expression - Glucose-6-phosphatase — diminished in cirrhotic nodules 3. **Impaired NAD⁺/NADH ratio**: Chronic alcohol metabolism depletes NAD⁺, shifting the lactate dehydrogenase equilibrium toward lactate formation and away from pyruvate. 4. **Portal hypertension and shunting**: Portosystemic shunts bypass the liver, allowing lactate-rich blood to enter systemic circulation without hepatic processing. 5. **Mitochondrial dysfunction**: Alcohol-induced mitochondrial damage reduces oxidative capacity and ATP generation needed for gluconeogenesis. ### The Broken Cori Cycle in Cirrhosis ```mermaid flowchart TD A["Muscle: Lactate production"] -->|Lactate via portal blood| B{"Cirrhotic Liver"} B -->|Impaired uptake & clearance| C["Lactate accumulates in blood"] B -->|Portosystemic shunts| D["Lactate bypasses liver"] C --> E["Metabolic acidosis + Type B lactic acidosis"] D --> E F["Reduced NAD+, mitochondrial dysfunction"] -.->|Impairs gluconeogenesis| B style B fill:#ffebee style C fill:#ffcdd2 style E fill:#c62828 ``` ### Type A vs. Type B Lactic Acidosis | Feature | Type A (Tissue Hypoxia) | Type B (No Hypoxia) | |---------|------------------------|---------------------| | **Cause** | Shock, sepsis, hypoxemia | Liver disease, metformin, malignancy | | **Lactate source** | Increased production from anaerobic metabolism | Normal/increased production, impaired clearance | | **Hemodynamics** | Hypotension, poor perfusion | Normal or hypertensive | | **Response to O₂** | Improves with oxygenation/perfusion | Does NOT improve with O₂ alone | | **Prognosis** | Depends on underlying shock | Often poor in cirrhosis | **High-Yield:** This patient has **Type B lactic acidosis** because: - Blood pressure is not mentioned as low (suggesting no shock) - Liver disease (cirrhosis) is the primary cause - Lactate accumulation is due to impaired hepatic clearance, not tissue hypoxia ### Clinical Pearl: The NAD⁺ Problem Chronic alcohol metabolism generates excess NADH, depleting NAD⁺ pools. This shifts the lactate dehydrogenase reaction: $$\text{Lactate} + \text{NAD}^+ \rightleftharpoons \text{Pyruvate} + \text{NADH} + \text{H}^+$$ With depleted NAD⁺, the reaction is driven toward lactate accumulation. Additionally, pyruvate cannot be efficiently converted to oxaloacetate (the first step of gluconeogenesis) without adequate NAD⁺-dependent oxidation. **Warning:** Do NOT confuse Type B lactic acidosis with sepsis-induced lactic acidosis. In sepsis (Type A), lactate rises because of tissue hypoxia and anaerobic metabolism; in cirrhosis (Type B), lactate rises because the liver cannot clear it, even though tissues are not hypoxic. [cite:Harrison 21e Ch 297; Robbins 10e Ch 18] 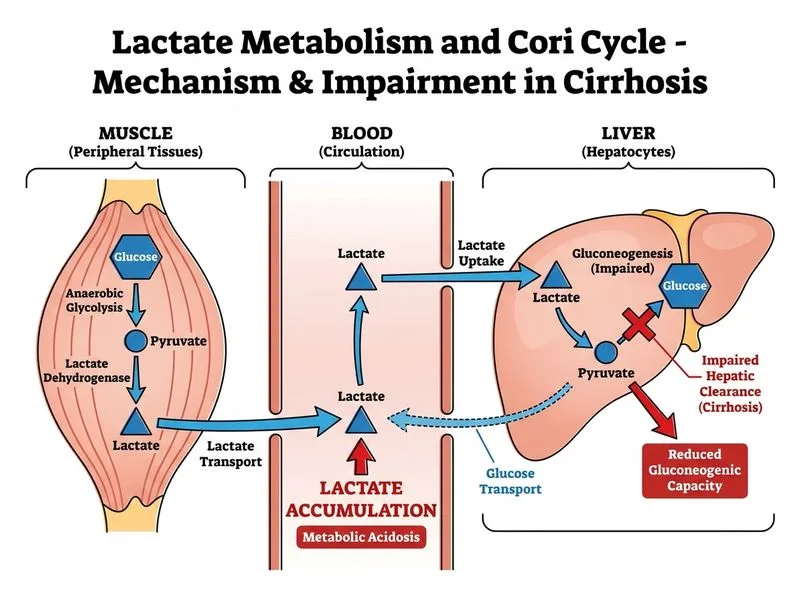
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.