## Type B Lactic Acidosis in Cirrhosis: Impaired Lactate Clearance ### Clinical Context This patient has advanced cirrhosis with metabolic derangement. The elevated lactate with metabolic acidosis (pH 7.28, HCO~3~^−^ 14) in the setting of liver disease represents **Type B lactic acidosis** — lactate accumulation due to impaired hepatic clearance, not tissue hypoxia. ### Pathophysiology of Lactate Metabolism in Cirrhosis **Key Point:** The liver is the primary organ for lactate clearance via two pathways: 1. **Gluconeogenesis:** Lactate → pyruvate → glucose (Cori cycle) 2. **Oxidation:** Lactate → pyruvate → TCA cycle → CO~2~ + H~2~O In cirrhosis, both pathways are impaired due to: - Loss of hepatocyte mass and synthetic function - Mitochondrial dysfunction in remaining hepatocytes - Reduced NAD^+^ availability (shunting to ethanol metabolism if applicable) - Impaired oxidative phosphorylation ### Why the Correct Answer is Correct **High-Yield:** Type B lactic acidosis occurs when lactate **production is normal or only mildly elevated**, but **clearance is severely impaired**. This is the hallmark of cirrhosis. In this patient: - Hepatocytes cannot efficiently oxidize lactate to pyruvate due to mitochondrial dysfunction - The Cori cycle is blocked because the liver cannot perform gluconeogenesis (synthetic failure) - Lactate accumulates despite normal tissue perfusion (no shock, normal blood pressure not stated but no hypotension clues) - The combination of elevated lactate + metabolic acidosis + hepatic encephalopathy is pathognomonic for Type B lactic acidosis in liver disease **Clinical Pearl:** Type B lactic acidosis in cirrhosis carries a poor prognosis and is often a marker of acute-on-chronic liver failure. Lactate levels >4 mmol/L correlate with increased mortality. ### Mnemonic **TYPE A vs TYPE B LACTIC ACIDOSIS** | Feature | Type A | Type B | |---------|--------|--------| | **Cause** | Tissue hypoxia/hypoperfusion | No tissue hypoxia; impaired lactate clearance | | **Clinical Setting** | Shock, sepsis, MI, cardiac arrest | Liver disease, malignancy, metformin + renal failure | | **Lactate Source** | Increased production (anaerobic metabolism) | Normal/mildly increased production | | **Lactate Clearance** | Normal (if perfusion restored) | Severely impaired | | **Prognosis** | Better if underlying cause reversed | Worse; often irreversible | | **In Cirrhosis** | Rare unless variceal bleed/shock | Common; independent mortality predictor | ### Why Each Distractor is Wrong | Option | Reason | |--------|--------| | Impaired gluconeogenesis alone | While true, this explains only part of the problem. The key issue is **impaired lactate oxidation** (mitochondrial dysfunction), not just blocked gluconeogenesis. Both pathways are affected. | | Type A (tissue hypoperfusion) | Type A requires evidence of shock: hypotension, oliguria, elevated creatinine, or sepsis. This patient has no stated hypotension or shock markers. Type A is ruled out by the clinical context of stable cirrhosis without acute decompensation/bleeding. | | Increased muscle lactate production | Hyperglycemia and insulin resistance do not significantly increase lactate production. Muscle lactate production is driven by exercise or anaerobic metabolism, not by hyperglycemia alone. This is a minor contributor. | [cite:Harrison Principles of Internal Medicine 21e Ch 382; Robbins & Cotran Pathologic Basis of Disease 10e Ch 20] 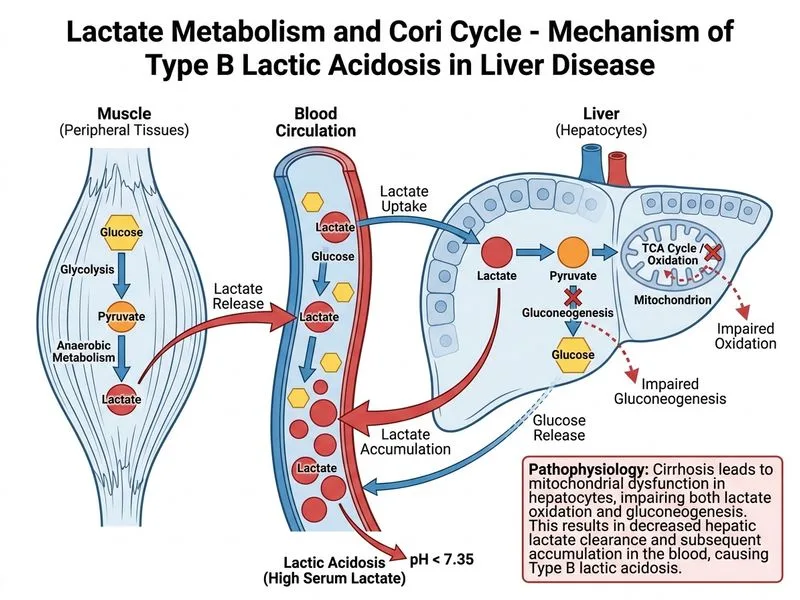
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.