## Diagnosis: Type 2 Lepra Reaction (Erythema Nodosum Leprosum) ### Clinical Presentation The patient presents with: - Acute onset painful nodules and plaques (not existing lesions) - Systemic symptoms: fever, malaise - Timing: 8 months into treatment (typical onset 6 months to 2 years) - High bacillary load (lepromatous leprosy) ### Type 2 Lepra Reaction (ENL) — Key Features **Key Point:** Type 2 lepra reaction (ENL) is an **immune complex-mediated (Type III hypersensitivity)** reaction occurring in lepromatous (LL) and borderline lepromatous (BL) leprosy patients, typically 6 months to 2 years after starting treatment. **High-Yield:** ENL occurs in approximately 50% of LL and 10% of BL patients. It is characterized by: 1. **Acute nodules** — tender, painful, often on face, trunk, and limbs 2. **Systemic symptoms** — fever, malaise, lymphadenopathy 3. **Extracutaneous involvement** — neuritis, iritis, orchitis, glomerulonephritis 4. **Timing** — typically months into therapy (antigen-antibody complexes form as bacilli die) ### Pathogenesis ENL is triggered by **antigen–antibody immune complex deposition** in tissues. As bacilli die during treatment, soluble antigens are released, forming complexes with IgG antibodies. These deposit in skin, nerves, eyes, and kidneys, activating complement and causing inflammation. ### Differential: Type 1 vs Type 2 Lepra Reaction | Feature | Type 1 (Reversal Reaction) | Type 2 (ENL) | |---------|---------------------------|---------------| | **Mechanism** | Cell-mediated (Type IV hypersensitivity) | Immune complex (Type III hypersensitivity) | | **Leprosy type** | BT, BL, BB (unstable) | LL, BL (high bacillary load) | | **Onset** | Any time (often within 1 year) | 6 months to 2 years after treatment | | **Lesion character** | Existing lesions become inflamed | NEW tender nodules | | **Systemic signs** | Mild or absent | Prominent (fever, malaise) | | **Bacillary load** | Variable | High (LL/BL) | | **Slit-skin smear** | May decrease | Remains high | | **Treatment** | Corticosteroids ± continue MDT | NSAIDs, corticosteroids, thalidomide | **Clinical Pearl:** The distinction is critical—Type 1 reactions show inflammation of *existing* lesions, while Type 2 shows *new* painful nodules with systemic toxicity. ### Management of ENL 1. **Mild ENL** — NSAIDs (aspirin, ibuprofen) + continue MDT 2. **Moderate to severe ENL** — Corticosteroids (prednisolone 0.5–1 mg/kg/day, taper over weeks) 3. **Recurrent/severe ENL** — Thalidomide (100–400 mg/day) — highly effective but teratogenic 4. **Continue MDT** — Do NOT stop antileprosy drugs **Warning:** Do not confuse ENL with drug resistance or superinfection. The high bacillary count and systemic inflammation are hallmarks of an immune reaction, not treatment failure. 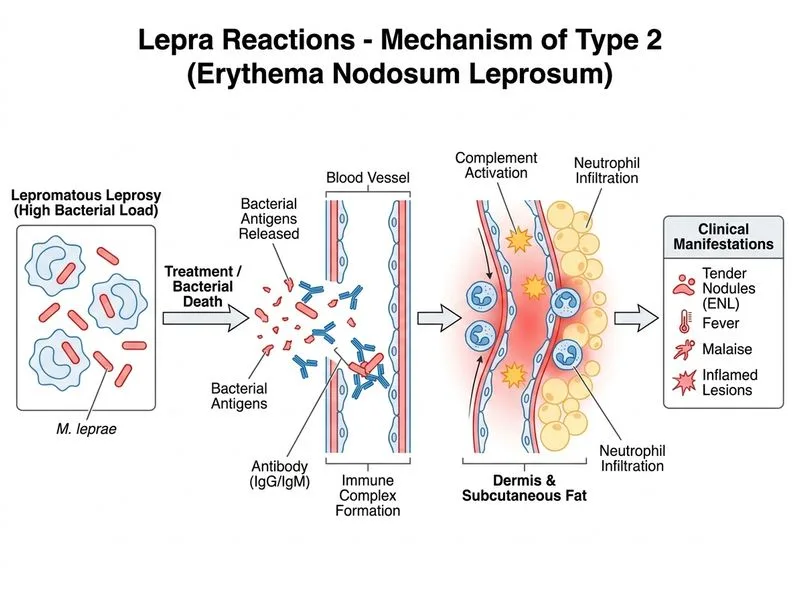
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.