## Diagnosis: Type 2 Lepra Reaction (Erythema Nodosum Leprosum) ### Clinical Presentation **Key Point:** Type 2 lepra reaction (ENL) occurs in lepromatous (LL) and borderline lepromatous (BL) leprosy patients, typically 6–24 months after starting MDT or during treatment. This patient presents with: - Painful nodules on shins (erythema nodosum pattern) - Constitutional symptoms (fever) - Polyarthralgia/arthritis (knees, ankles) - Timing: 6 months into MDT (classic window) ### Pathophysiology **High-Yield:** Type 2 lepra reaction is an **immune complex-mediated (Type III hypersensitivity)** reaction, not a cell-mediated response. 1. Occurs in patients with high bacillary loads (LL/BL) 2. Triggered by release of mycobacterial antigens during MDT 3. Immune complexes (IgG + mycobacterial Ag) deposit in skin, joints, eyes, nerves 4. Complement activation → neutrophilic infiltration → inflammation ### Histopathology **Clinical Pearl:** Neutrophilic infiltration with immune complex deposition (IgG, C3) on immunofluorescence is pathognomonic for ENL. ### Differential: Type 1 vs Type 2 Lepra Reactions | Feature | Type 1 (Reversal Reaction) | Type 2 (ENL) | |---------|---------------------------|---------------| | **Leprosy type** | BT, BL, BL, TT | LL, BL | | **Timing** | During/shortly after MDT | 6–24 months into MDT | | **Pathophysiology** | Cell-mediated (Type IV) | Immune complex (Type III) | | **Clinical signs** | Inflammation of existing lesions, neuritis | Erythema nodosum, arthritis, iritis, neuritis | | **Histology** | Epithelioid granulomas | Neutrophilic infiltration, IC deposition | | **Systemic features** | Rare | Common (fever, constitutional) | | **Treatment** | Corticosteroids ± NSAIDs | Thalidomide (first-line) or corticosteroids | **Mnemonic for ENL timing:** **"6–24 months"** — remember this window; it's the classic presentation period. ### Management **Key Point:** Thalidomide is the drug of choice for ENL (100–400 mg/day), with dramatic response in 24–48 hours. Corticosteroids are second-line. ### Why This Patient Has ENL - High bacillary load at baseline (LL diagnosis) - 6 months into MDT (peak window for ENL) - Immune reconstitution and antigen release trigger IC formation - Systemic involvement (fever, polyarthritis) typical of ENL [cite:Textbook of Dermatology, Valia & Valia Ch 28] 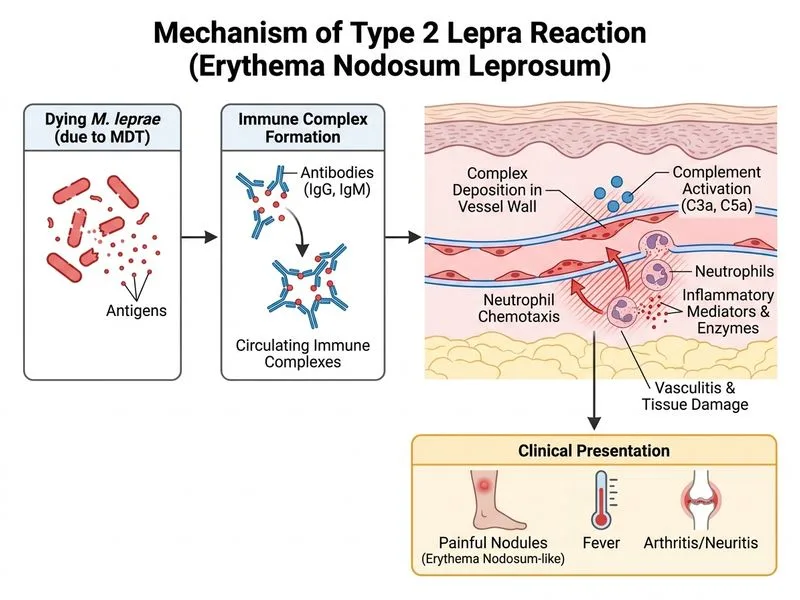
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.