## Diagnosis: Type 1 Lepra Reaction (Reversal Reaction) with Neuritis ### Clinical Presentation **Key Point:** Type 1 lepra reaction (reversal reaction) is a cell-mediated (Type IV hypersensitivity) reaction that occurs in borderline forms of leprosy (BT, BL, LL) during or shortly after starting MDT. This patient has: - Borderline tuberculoid (BT) leprosy - Timing: 3 months into MDT (typical for Type 1) - Inflammation of existing skin lesions (erythema, edema) - **Acute nerve involvement** (ulnar nerve pain, swelling, motor weakness) - **No systemic symptoms** (no fever, constitutional signs) - Negative slit-skin smear (low bacillary load consistent with BT) ### Pathophysiology **High-Yield:** Type 1 lepra reaction is **delayed-type (cell-mediated) hypersensitivity** triggered by: 1. Immune reconstitution as bacillary load decreases 2. Shift from Th2 to Th1 response 3. Activation of CD4+ and CD8+ T cells against mycobacterial antigens 4. Inflammation of existing lesions and nerves ### Clinical Features of Type 1 Reaction | Feature | Details | |---------|----------| | **Leprosy types affected** | BT, BL, LL (borderline forms) | | **Timing** | During or shortly after starting MDT (weeks to months) | | **Skin manifestations** | Erythema, edema, ulceration of existing lesions | | **Nerve involvement** | Acute neuritis, nerve thickening, pain, motor/sensory loss | | **Systemic symptoms** | Absent or minimal | | **Bacillary load** | Usually low (slit-skin smear negative) | | **Histology** | Epithelioid granulomas with edema | ### Management of Type 1 Lepra Reaction **Key Point:** The cornerstone of treatment is **high-dose corticosteroids** (prednisolone 0.5–1 mg/kg/day, tapered over 12 weeks). **Clinical Pearl:** Nerve involvement in Type 1 reaction is a medical emergency because: - Acute inflammation can cause irreversible nerve damage - Early corticosteroid therapy prevents permanent disability - If no improvement in 2 weeks despite corticosteroids, **nerve decompression surgery** may be indicated to prevent permanent loss of function ### Treatment Algorithm for Type 1 Reaction with Neuritis ```mermaid flowchart TD A[Type 1 Lepra Reaction with Neuritis]:::outcome --> B[Start high-dose prednisolone<br/>0.5-1 mg/kg/day]:::action B --> C[Continue MDT without interruption]:::action C --> D[Reassess at 2 weeks]:::decision D -->|Improvement| E[Taper prednisolone over 12 weeks]:::action D -->|No improvement| F[Consider nerve decompression]:::urgent F --> G[Surgical intervention to prevent<br/>permanent disability]:::action ``` **Mnemonic for Type 1 management:** **"CORN"** — **C**orticosteroids, **O**ngoing MDT, **R**eassess at 2 weeks, **N**erve decompression if needed. ### Why MDT Should NOT Be Stopped **High-Yield:** MDT must continue during Type 1 reaction because: - The reaction is triggered by immune reconstitution, not drug toxicity - Stopping MDT allows bacillary regrowth and relapse - Corticosteroids control the inflammatory response while MDT continues ### Differential: Type 1 vs Type 2 Lepra Reactions | Feature | Type 1 (Reversal Reaction) | Type 2 (ENL) | |---------|---------------------------|---------------| | **Pathophysiology** | Cell-mediated (Type IV) | Immune complex (Type III) | | **Leprosy type** | BT, BL, LL | LL, BL | | **Timing** | During/shortly after MDT | 6–24 months into MDT | | **Skin signs** | Inflammation of existing lesions | Erythema nodosum (new lesions) | | **Neuritis** | Common, acute | Less common | | **Systemic symptoms** | Rare | Common (fever, arthritis) | | **Treatment** | Corticosteroids | Thalidomide (first-line) | [cite:Textbook of Dermatology, Valia & Valia Ch 28; WHO Guidelines on Leprosy] 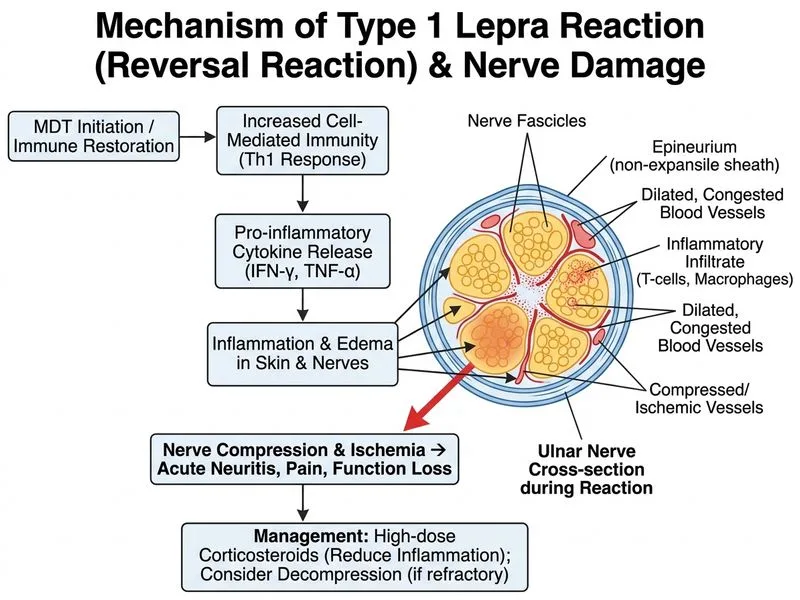
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.