## Diagnosis: Lepra Reaction Type 1 (Reversal Reaction) ### Clinical Features Pointing to Type 1 Reaction **Key Point:** Type 1 lepra reaction (reversal reaction) is a delayed-type hypersensitivity (Type IV) response occurring in unstable forms of leprosy (BT, BB, BL) during or shortly after MDT initiation. It is characterized by acute inflammation of existing lesions and nerves. **Clinical Pearl:** The acute onset of nerve pain, swelling, and new sensory loss in a BT patient on MDT—with no systemic fever or nodules—is pathognomonic for Type 1 reaction. ### Distinguishing Features: Type 1 vs Type 2 (ENL) | Feature | Type 1 Reaction | ENL (Type 2) | |---------|-----------------|---------------| | **Leprosy form** | BT, BB, BL (unstable) | LL, BL (high bacillary load) | | **Timing** | At diagnosis or early MDT | During/after MDT (months to years) | | **Pathogenesis** | Type IV (cell-mediated) | Type III (immune complex) | | **Skin lesions** | Plaques/infiltrates become inflamed, not tender | Tender nodules (erythema nodosum) | | **Nerve involvement** | Acute nerve pain, swelling, nerve damage | Neuritis (can occur but not primary) | | **Systemic signs** | Absent (localized to skin/nerves) | Fever, lymphadenitis, iritis, hepatosplenomegaly | | **Lepromin test** | Positive (cell-mediated immunity intact) | Strongly positive | | **Bacillary load** | Low to moderate | High | **High-Yield:** Type 1 reaction is the most common lepra reaction (50–60% of cases) and occurs in intermediate forms. It manifests as acute inflammation of existing lesions and acute neuritis with nerve damage. ### Pathophysiology of Type 1 Reaction 1. **Shift in cell-mediated immunity** — patient's immune system becomes stronger during MDT 2. **Delayed-type hypersensitivity** to mycobacterial antigens in existing lesions 3. **Acute inflammation** of skin lesions and nerves 4. **Nerve damage** from edema and inflammation within the nerve sheath 5. **Acute sensory/motor loss** if nerve compression is severe **Mnemonic:** Type 1 = **T**ype IV = **T**ransition = **T**hickened nerves = **T**ender nerve trunks (not skin lesions) = **T**emporal (early in course) ### Clinical Presentation in This Case - **Acute nerve pain and swelling** → Type 1 reaction hallmark - **New anesthetic patches** → acute nerve damage from inflammation - **Marked nerve thickening and tenderness** → acute neuritis - **No fever, no systemic signs** → excludes ENL - **BT form on MDT** → unstable form at risk for Type 1 ### Management - **Corticosteroids:** Prednisolone 0.5–1 mg/kg/day, taper over 8–12 weeks - **NSAIDs:** For mild cases - **Nerve care:** Splinting, eye care if facial nerve involved - **Continue MDT** throughout reaction treatment - **Urgent intervention** if severe nerve compression (risk of permanent disability) **Clinical Pearl:** Early recognition and aggressive corticosteroid therapy can prevent permanent nerve damage in Type 1 reactions. 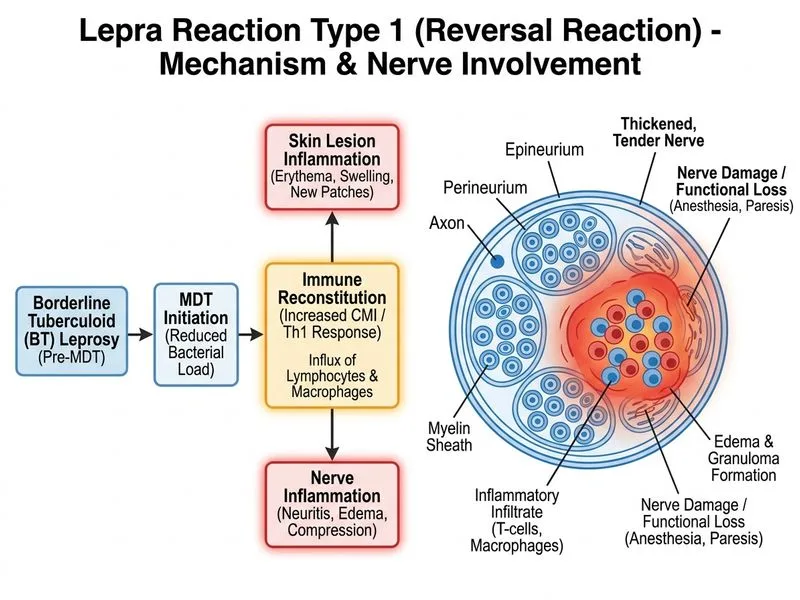
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.