## Clinical Classification & Management Approach **Key Point:** This patient presents with a single skin lesion, negative nerve involvement, and a positive slit-skin smear (2+). According to the Ridley-Jopling classification and WHO operational classification, this constellation of findings is consistent with **tuberculoid leprosy (TT)**. ### Why Immediate MDT for Tuberculoid Leprosy? **High-Yield:** The WHO operational classification divides leprosy into: | Feature | Tuberculoid (TT) | Borderline (BT/BL/BB) | Lepromatous (LL) | |---------|------------------|----------------------|------------------| | Number of lesions | 1–5 | 5–many | >5, ill-defined | | Bacillary load | Scanty (1–2+) | Moderate (3–4+) | Heavy (4–6+) | | Nerve involvement | Early, asymmetric | Variable | Late, symmetric | | Sensory loss | Early, well-demarcated | Moderate | Late, ill-defined | | Treatment duration | 6 months | 12 months | 12 months | **Clinical Pearl:** A single lesion with positive smear does NOT mean lepromatous leprosy. The bacillary load in tuberculoid disease is low (1–2+), and this patient's single lesion with no nerve thickening fits the tuberculoid pattern perfectly. ### Rationale for Immediate Treatment 1. **Early diagnosis is confirmed** — clinical features + slit-skin smear positivity establish the diagnosis. 2. **No additional nerve studies are needed** — the clinical examination (no nerve thickening, normal sensation on the lesion border) is sufficient for classification. 3. **Delay increases disability risk** — early MDT prevents nerve damage and skin lesion progression. 4. **MDT regimen is standardized** — 6-month WHO MDT for tuberculoid leprosy is the standard of care. **Mnemonic: SINGLE lesion + Scanty bacilli + Sensory loss = Start tuberculoid MDT** ### Why Not the Other Options? See distractor reasoning below. 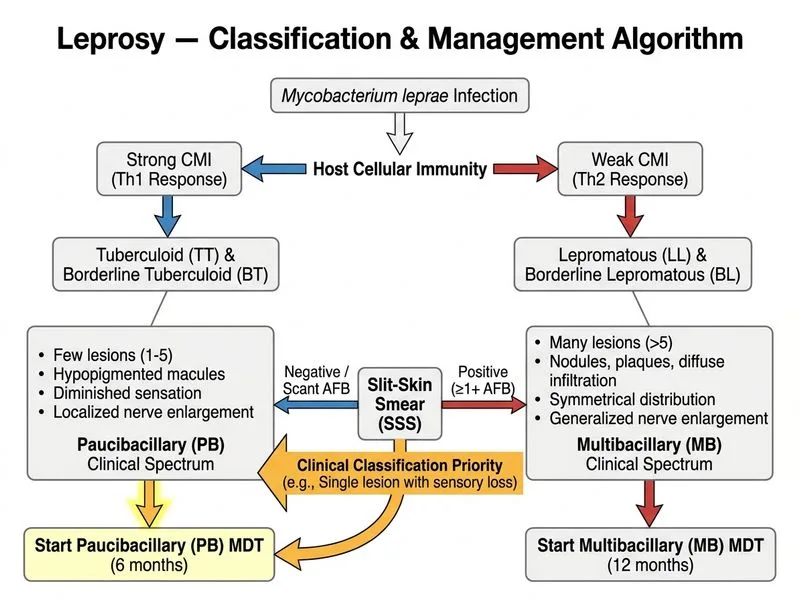
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.