## Classification Basis This patient presents with clinical and histopathological features consistent with **tuberculoid leprosy (TT)**, the most resistant form of the leprosy spectrum. ### Key Clinical Features Present **Key Point:** Tuberculoid leprosy is characterized by a single or very few (typically <5) well-demarcated hypopigmented lesions with complete anesthesia and no nerve thickening. | Feature | Tuberculoid Leprosy | Borderline Tuberculoid | |---------|-------------------|----------------------| | Number of lesions | 1–5, well-defined | 5–20, asymmetric | | Sensory loss | Complete anesthesia | Present but variable | | Nerve thickening | Absent or minimal | Mild to moderate | | Bacillary load | 0–1+ (paucibacillary) | 1–2+ | | Granuloma type | Epithelioid, Langhans cells | Epithelioid, fewer Langhans | | Lepromin test | Strongly positive | Positive | ### Histopathology Correlation **High-Yield:** The presence of epithelioid granulomas with Langhans cells and minimal/absent acid-fast bacilli (negative slit-skin smear) is pathognomonic for the tuberculoid end of the spectrum. The paucibacillary nature (AFB negative) rules out borderline lepromatous and lepromatous forms. ### Immunological Basis **Clinical Pearl:** Tuberculoid leprosy represents a strong cell-mediated immune (Th1) response to *Mycobacterium leprae*, resulting in: - Granulomatous inflammation with epithelioid cells and Langhans cells - Minimal bacillary survival (paucibacillary) - Positive lepromin test (delayed-type hypersensitivity) - Single or few lesions due to localized immunity ### Why Not Borderline Tuberculoid? Borderline tuberculoid (BT) would show: - More numerous lesions (5–20 vs. single) - Variable sensory loss (not complete anesthesia) - Mild nerve thickening (absent here) - Slightly higher bacillary load (1–2+ vs. 0–1+) [cite:Park 26e Ch 8] 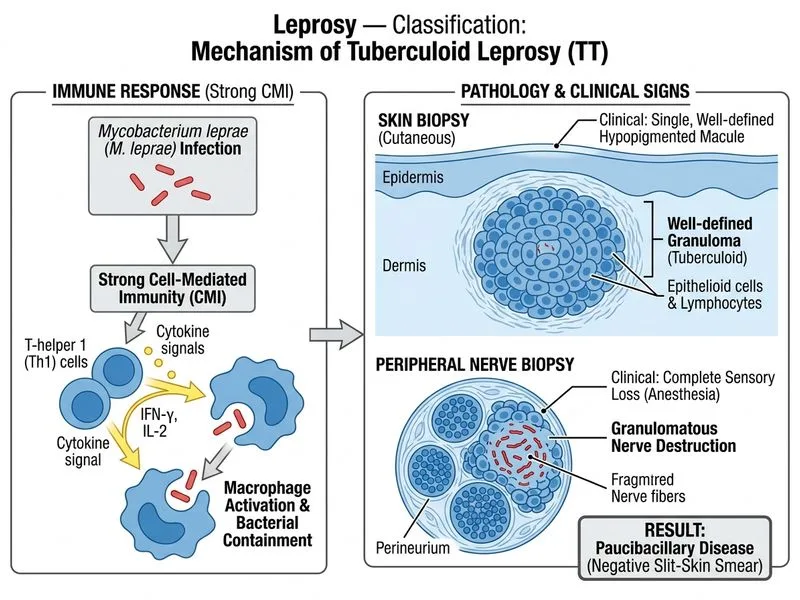
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.