## Clinical Diagnosis: Lichen Planus with Oral Involvement ### Key Diagnostic Features **Key Point:** Lichen planus is a chronic inflammatory condition that classically presents with the "6 Ps": Purple, Planar (flat-topped), Polygonal, Papules, Plaques, and Pruritus. ### Clinical Presentation in This Case | Feature | Finding | Significance | |---------|---------|-------------| | **Oral manifestation** | Wickham's striae (reticular white lines) + erosions | Pathognomonic for oral lichen planus | | **Skin lesions** | Shiny, flat-topped purple papules on flexural surfaces | Classic distribution and morphology | | **Dermoscopy** | Reticular pattern with white dots and lines | Confirms lichen planus diagnosis | | **Duration** | 3 months (chronic) | Consistent with LP's indolent course | | **Symptom profile** | Pruritus + oral pain | Typical presentation | ### Pathophysiology 1. **T-cell mediated autoimmune response** against basal keratinocytes 2. **Cytotoxic CD8+ T lymphocytes** infiltrate the dermoepidermal junction 3. **Liquefactive necrosis** of basal layer → saw-tooth appearance on histology 4. **Oral involvement** occurs in ~50% of cutaneous LP cases ### Histopathological Hallmarks **High-Yield:** The classic triad on histology: - Saw-tooth (acanthotic) hyperkeratosis - Liquefactive degeneration of basal layer - Dense band-like lymphocytic infiltrate at dermoepidermal junction ("lichenoid" pattern) ### Oral Lichen Planus Subtypes - **Reticular (most common):** Wickham's striae, asymptomatic - **Erosive:** Painful ulcerations, higher malignant transformation risk (~1%) - **Atrophic:** Thin erythematous areas - **Bullous:** Rare, severe form **Clinical Pearl:** Erosive oral lichen planus carries a 0.5–1% risk of malignant transformation to oral squamous cell carcinoma; regular monitoring is essential. ### Differential Diagnosis Exclusion ```mermaid flowchart TD A[Oral erosions + skin rash]:::outcome --> B{Wickham's striae present?}:::decision B -->|Yes| C[Lichen planus]:::action B -->|No| D{Flaccid bullae + positive Nikolsky?}:::decision D -->|Yes| E[Pemphigus vulgaris]:::outcome D -->|No| F{Target lesions + mucositis?}:::decision F -->|Yes| G[Erythema multiforme]:::outcome F -->|No| H{Pseudomembrane + candida on KOH?}:::decision H -->|Yes| I[Oral candidiasis]:::outcome ``` ### Management Approach **Key Point:** Treatment is symptom-driven; no cure exists. Goals are to reduce inflammation and prevent malignant transformation. 1. **First-line:** Topical corticosteroids (triamcinolone 0.1% paste for oral, clobetasol for skin) 2. **Second-line:** Intralesional corticosteroids or topical calcineurin inhibitors (tacrolimus) 3. **Systemic therapy:** Oral corticosteroids or retinoids for severe/erosive disease 4. **Monitoring:** Regular oral examination, especially erosive cases **Mnemonic: LPLP** — **L**iquefactive necrosis, **P**urple papules, **L**ymphocytic infiltrate, **P**ruritus [cite:Robbins 10e Ch 25] 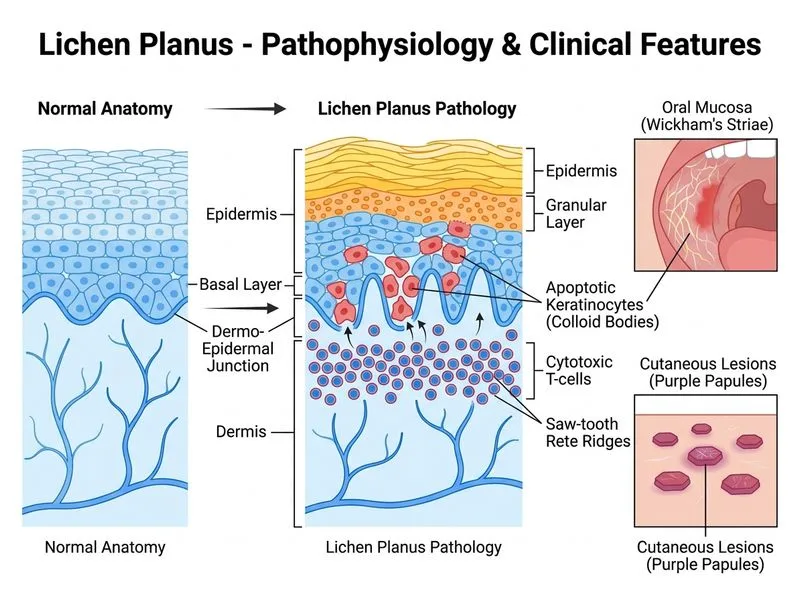
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.