## Pathophysiology of Lichen Planus: Basal Layer Necrosis ### Diagnostic Confirmation **Key Point:** The histopathological triad—saw-tooth hyperkeratosis, liquefactive necrosis of the basal layer, and band-like lymphocytic infiltrate—is pathognomonic for lichen planus. ### Immunopathological Mechanism ### Mechanism of Basal Layer Destruction 1. **CD8+ T-cell recognition:** Cytotoxic T lymphocytes recognize altered self-antigens on basal keratinocytes (possibly keratin 16 or other intracellular antigens) 2. **Lymphocyte infiltration:** Dense band-like infiltrate of CD8+ T cells and macrophages localizes to the dermoepidermal junction 3. **Cytotoxic granule release:** Activated CD8+ cells release perforin and granzyme B, inducing apoptosis of basal keratinocytes 4. **Liquefactive necrosis:** Basal cell death results in loss of cellular architecture ("liquefactive" = cell lysis without inflammation) 5. **Epithelial-mesenchymal separation:** Destruction of basal layer → dermal-epidermal separation and potential erosion **High-Yield:** Lichen planus is a **Type IV hypersensitivity reaction** (delayed cell-mediated immunity), NOT antibody-mediated. ### Histological Correlation with Mechanism | Histological Finding | Mechanism | Immunological Basis | |----------------------|-----------|--------------------| | **Saw-tooth hyperkeratosis** | Reactive epidermal thickening | Response to basal cell loss | | **Liquefactive necrosis of basal layer** | Apoptosis of keratinocytes | CD8+ cytotoxic T-cell attack | | **Band-like lymphocytic infiltrate** | Dense T-cell accumulation | CD8+ and CD4+ T-cell infiltration | | **Melanin incontinence** | Destruction of basal melanocytes | Collateral damage from T-cell attack | ### Immunological Markers ```mermaid flowchart TD A[Lichen Planus Pathogenesis]:::outcome --> B[Antigen presentation]:::action B --> C[Keratinocyte antigen + MHC Class I]:::action C --> D[CD8+ T-cell activation]:::action D --> E[Cytotoxic granule release]:::action E --> F[Perforin + Granzyme B]:::action F --> G[Basal keratinocyte apoptosis]:::action G --> H[Liquefactive necrosis]:::outcome H --> I[Dermal-epidermal separation]:::outcome ``` **Mnemonic: CD8-LP** — **CD8+** cytotoxic T cells drive **L**ichen **P**lanus pathology ### Why NOT the Other Mechanisms? **Viral infection (Option B):** While some viruses (e.g., hepatitis C) are associated with LP, the primary mechanism is not direct viral cytolysis but rather immune cross-reactivity. Viral inclusions are not seen on histology. **Immune complex deposition (Option C):** This is the mechanism in lupus erythematosus (Type III hypersensitivity), not LP. Immunofluorescence in LP is negative for IgG/IgM/C3 deposition at the basement membrane. **Anti-desmoglein 3 antibodies (Option D):** This is the mechanism in pemphigus vulgaris (acantholysis, not basal necrosis). Serology in LP is negative for anti-desmoglein antibodies. ### Clinical Correlations **Clinical Pearl:** The pruritus in lichen planus is driven by cytokine release (TNF-α, IFN-γ) from infiltrating T cells, explaining why antihistamines are often ineffective. **High-Yield:** Lichen planus is associated with: - Hepatitis C (15–60% in endemic regions) - Hepatitis B (rare) - Graft-versus-host disease (GVHD) can mimic LP - Lichenoid drug reactions (NSAIDs, ACE inhibitors, antimalarials) ### Diagnostic Confirmation **Immunohistochemistry:** CD8+ T cells predominate in the infiltrate; CD4+ T cells are also present. Langerhans cells (CD1a+) are increased. [cite:Robbins 10e Ch 25; Harrison 21e Ch 439] 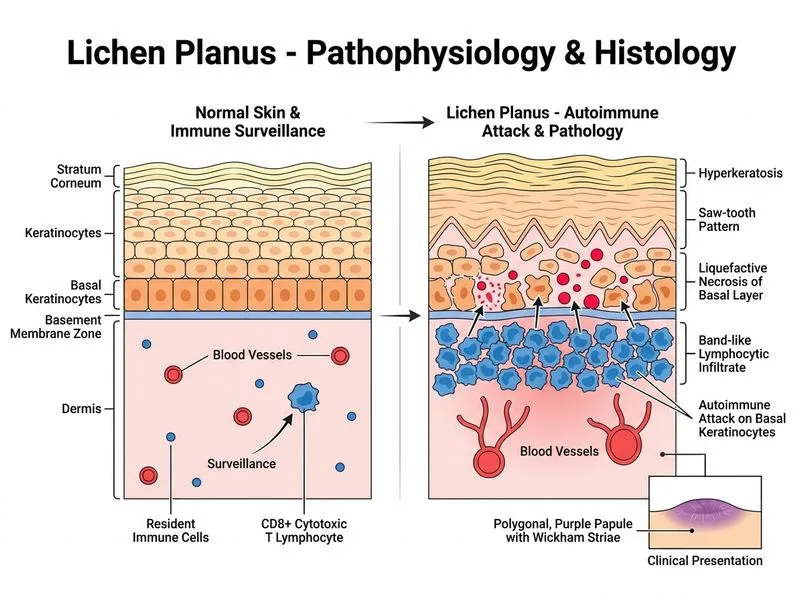
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.