## Confirmatory Investigation for Lichen Planus **Key Point:** Skin biopsy with histopathology is the gold standard for confirming lichen planus. The diagnosis is primarily clinical, but histology provides definitive confirmation when diagnosis is uncertain. ### Histopathological Features The classic histological findings in lichen planus include: | Feature | Description | |---------|-------------| | **Hyperkeratosis** | Thickened stratum corneum | | **Hypergranulosis** | Prominent granular layer | | **Saw-tooth acanthosis** | Irregular, pointed rete ridges | | **Lichenoid infiltrate** | Dense band-like lymphocytic infiltration at dermoepidermal junction | | **Basal cell degeneration** | Liquefactive necrosis of basal layer | | **Absence of spongiosis** | No intercellular edema (distinguishes from dermatitis) | **High-Yield:** The "saw-tooth" pattern of rete ridges and the dense lymphocytic band at the dermoepidermal junction are pathognomonic for lichen planus. ### Why Skin Biopsy? 1. Provides definitive histological diagnosis 2. Excludes mimics (lichenoid drug reactions, lupus erythematosus, lichen nitidus) 3. Indicated when clinical diagnosis is uncertain or atypical presentation 4. Can assess for dysplasia in oral lichen planus (malignant potential) **Clinical Pearl:** While lichen planus is often diagnosed clinically based on the "6 P's" (Purple, Planar, Polygonal, Papules, Plaques, Pruritus), biopsy is essential for oral erosive disease to rule out dysplasia and confirm diagnosis. **Mnemonic: SALT** — Saw-tooth rete ridges, Acanthosis (irregular), Lichenoid infiltrate, Thinned basal layer 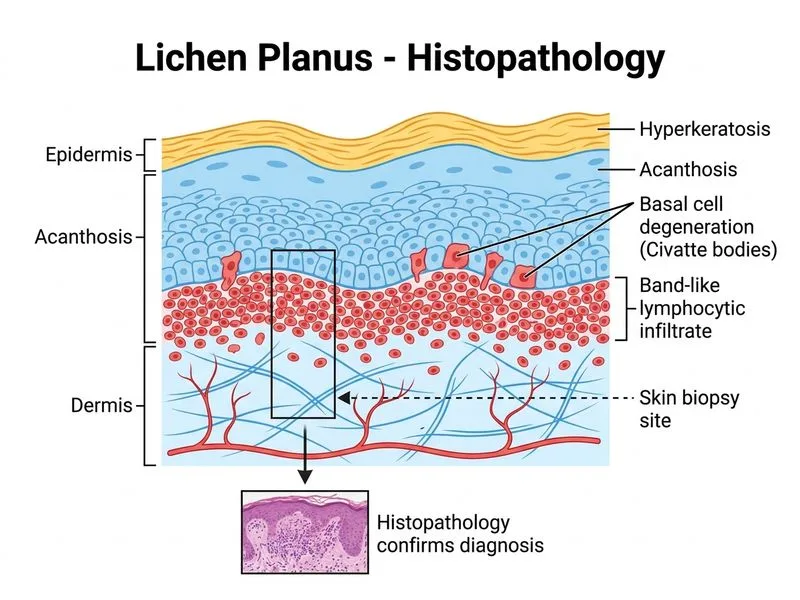
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.