## Assessment of Dysplasia in Oral Lichen Planus **Key Point:** Incisional biopsy with histopathology is the gold standard for assessing dysplasia in oral lichen planus and confirming the diagnosis. Oral lichen planus carries a 0.5–5% risk of malignant transformation to squamous cell carcinoma. ### Why Incisional Biopsy? **High-Yield:** Incisional biopsy (not excisional) is preferred because: 1. Provides adequate tissue for histological examination 2. Allows assessment of epithelial dysplasia grade (mild, moderate, severe) 3. Confirms diagnosis of lichen planus and excludes other conditions 4. Guides treatment intensity and surveillance frequency 5. Does not excise the lesion, allowing for future monitoring ### Dysplasia Grading in Oral Lichen Planus | Grade | Features | Management | |-------|----------|-------------| | **No dysplasia** | Normal maturation, intact basement membrane | Clinical follow-up every 6–12 months | | **Mild dysplasia** | Slight nuclear enlargement, hyperchromasia in basal 1/3 | Follow-up every 3–6 months, consider topical steroids | | **Moderate dysplasia** | Nuclear abnormalities in basal 1/2, increased mitoses | Follow-up every 3 months, systemic therapy, consider excision | | **Severe dysplasia** | Full-thickness nuclear abnormalities, high mitotic rate | Urgent referral, consider surgical excision | **Clinical Pearl:** Erosive oral lichen planus has a higher malignant transformation risk than reticular (non-erosive) disease. Biopsy is mandatory in erosive cases to establish baseline dysplasia grade and plan surveillance. **Mnemonic: BIOPSY for OLP** — Baseline dysplasia assessment, Incisional technique, Oral mucosa sampling, Prognostic grading, Surveillance planning, Yearly follow-up (if no dysplasia) 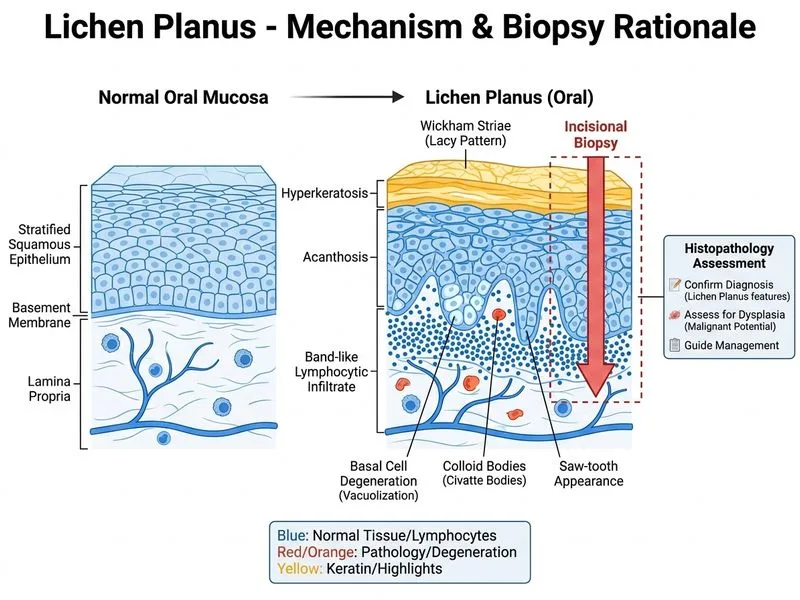
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.