## Diagnosis: Oral Lichen Planus with Cutaneous Involvement ### Clinical Presentation The patient demonstrates the classic dual presentation of lichen planus affecting both mucous membranes and skin: - **Oral involvement:** Painful erosions on buccal mucosa and gingiva with reticular (lacy white) pattern - **Cutaneous involvement:** Violaceous, flat-topped papules on wrists and forearms ### Histopathological Findings **Key Point:** The biopsy shows the pathognomonic "saw-tooth" appearance with: - Dense band-like (lichenoid) lymphocytic infiltrate at the dermoepidermal junction - Basal cell layer degeneration (vacuolar change) - Intact basement membrane (unlike pemphigus) - No subepidermal blister formation ### Diagnostic Criteria (6 Ps) **Mnemonic:** PAPULES — **P**urple, **A**ngled, **P**lanar, **U**rethra/Urticaria (rare), **L**ace-like (oral), **E**rosive (oral), **S**cars (atrophic) ### Oral vs. Cutaneous Lichen Planus | Feature | Oral LP | Cutaneous LP | |---------|---------|-------------| | Presentation | Reticular, erosive, painful | Papular, pruritic, non-erosive | | Malignant potential | 0.5–5% → SCC | Rare | | Duration | Often chronic | Self-limited (months–years) | | Biopsy | Identical histology | Identical histology | **High-Yield:** Oral lichen planus with cutaneous involvement is a single disease entity with mucocutaneous manifestation—not two separate conditions. ### Management Approach 1. Topical corticosteroids (fluocinonide gel for oral lesions) 2. Systemic corticosteroids if severe/erosive 3. Retinoids (acitretin) for resistant cases 4. Regular oral surveillance (malignant transformation risk) **Clinical Pearl:** The presence of erosive oral lesions with reticular pattern + violaceous papules on flexural surfaces is virtually diagnostic of lichen planus without need for additional investigations. [cite:Robbins 10e Ch 25] 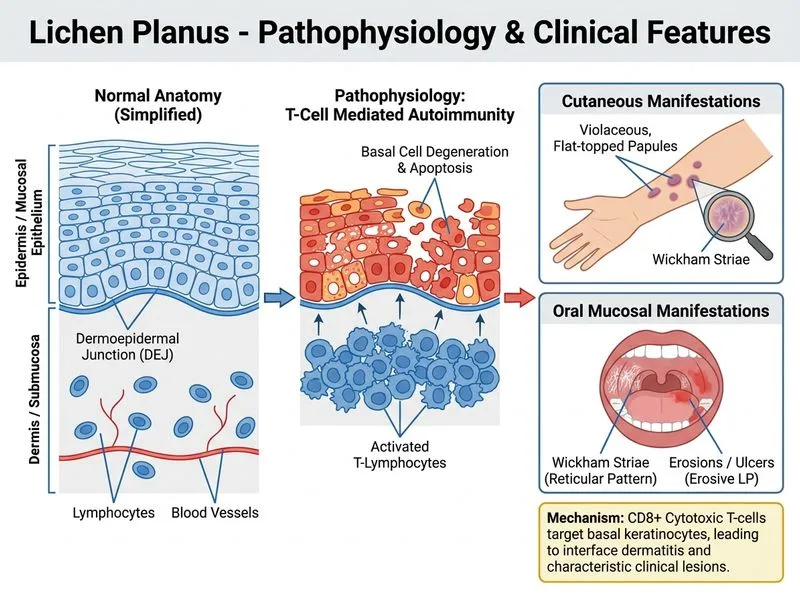
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.