## Neuroendocrine Markers in SCLC **Key Point:** Chromogranin A and synaptophysin are the most sensitive and specific immunohistochemical markers for confirming the neuroendocrine differentiation of small cell lung cancer. ### Diagnostic Immunohistochemistry Panel for SCLC | Marker | Sensitivity | Specificity | Role | |--------|-------------|-------------|------| | **Chromogranin A** | 85–90% | High | Gold standard for neuroendocrine differentiation | | **Synaptophysin** | 80–95% | High | Confirms neural origin; most sensitive | | **CD56 (NCAM)** | 85–95% | Moderate | Neuroendocrine marker; less specific than above | | Calcitonin | <10% | High | Rare in SCLC; seen in medullary thyroid carcinoma | | Somatostatin | Occasional | Moderate | Paraneoplastic secretion, not diagnostic | | Gastrin | Rare | High | Zollinger-Ellison syndrome; not SCLC marker | **High-Yield:** At least 2 of the 3 markers (chromogranin A, synaptophysin, CD56) must be positive for diagnosis of SCLC. Synaptophysin is often the most consistently positive. ### Paraneoplastic Syndromes vs. Diagnostic Markers **Warning:** Calcitonin, somatostatin, gastrin, and VIP are secreted by SCLC cells and cause paraneoplastic syndromes (SIADH, Cushing syndrome, diarrhea) but are NOT used for diagnosis. Their presence indicates hormone secretion, not diagnostic confirmation. **Clinical Pearl:** SCLC is the most common cause of paraneoplastic syndromes in lung cancer, including SIADH (15% of cases) and Cushing syndrome (5% of cases), but these are consequences of tumor biology, not diagnostic criteria. [cite:Robbins 10e Ch 15] 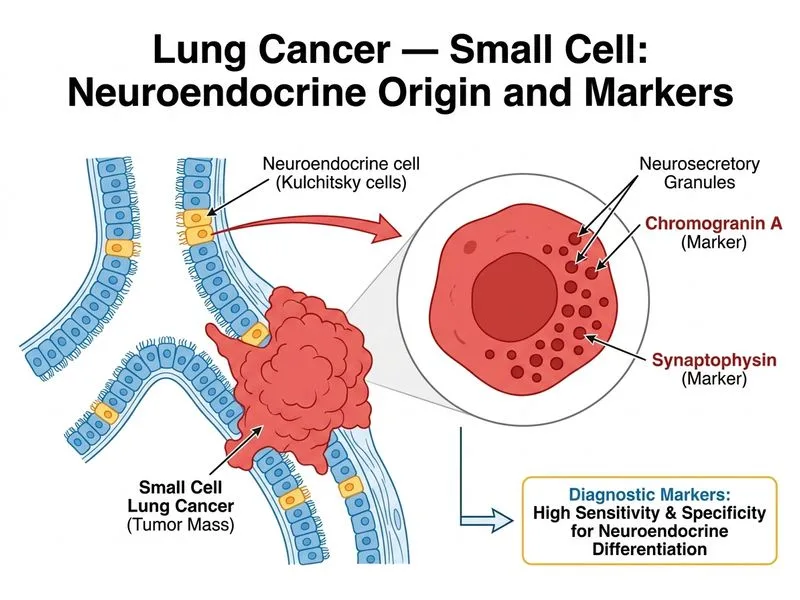
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.