## Diagnosis & Staging Approach **Key Point:** Small cell lung cancer (SCLC) is a neuroendocrine malignancy with aggressive biology and high propensity for early metastatic spread. Staging and treatment decisions hinge on distinguishing **limited-stage disease (LD-SCLC)** from **extensive-stage disease (ED-SCLC)**. ### Histopathological Confirmation The biopsy findings—small round cells, scant cytoplasm, finely dispersed chromatin, high mitotic rate, and positive neuroendocrine markers (chromogranin, synaptophysin)—are pathognomonic for SCLC. This is NOT adenocarcinoma, squamous cell, or large cell carcinoma. ### Staging Workup for SCLC | Investigation | Purpose | Rationale | |---|---|---| | **Brain MRI** | Detect CNS metastases | Present in ~10–15% at diagnosis; asymptomatic in 50% | | **Bone scan or PET-CT** | Detect skeletal metastases | Common site of spread; affects prognosis and treatment | | **Chest/abdominal imaging** | Assess locoregional and visceral involvement | Defines stage and resectability | | **PFTs & cardiac assessment** | Assess operability if LD-SCLC | Needed before any surgical consideration | **High-Yield:** The presence of mediastinal lymphadenopathy and hilar involvement in this case suggests at least **N2 disease**. However, absence of documented distant metastases (brain, bone, liver, adrenal) means this could still be **limited-stage SCLC** (defined as disease confined to one hemithorax and regional lymph nodes, treatable with curative intent). ### Treatment Decision Tree ```mermaid flowchart TD A[SCLC Diagnosis Confirmed]:::outcome --> B[Complete Staging Workup]:::action B --> C{Brain MRI + Bone Scan + Imaging}:::decision C -->|No Distant Metastases| D[Limited-Stage SCLC]:::outcome C -->|Distant Metastases Present| E[Extensive-Stage SCLC]:::outcome D --> F[Concurrent Chemoradiotherapy]:::action D --> G[Consider Surgery if Early T1-2 N0-1]:::action E --> H[Chemotherapy ± Palliative RT]:::action F --> I[Improved OS vs Sequential]:::outcome G --> J[Adjuvant Chemotherapy]:::action ``` ### Why Brain MRI & Bone Scan First? 1. **Prognostic impact:** Presence of brain or bone metastases immediately reclassifies the patient as extensive-stage, shifting treatment from curative to palliative intent. 2. **Treatment planning:** If limited-stage, concurrent chemoradiotherapy (cisplatin + etoposide + thoracic RT) is the standard of care and offers the best survival (median OS ~20–25 months vs ~12 months for sequential therapy). 3. **CNS prophylaxis:** If LD-SCLC achieves remission, prophylactic cranial irradiation (PCI) reduces brain relapse from ~40% to ~15%. **Clinical Pearl:** SCLC has a doubling time of ~30 days and metastasizes early via lymphatic and hematogenous routes. Delays in staging and treatment initiation directly worsen outcomes. ### Why Not Proceed to Surgery? Although the patient has a central mass with mediastinal involvement, **SCLC is rarely resectable for cure** even in early-stage disease. Surgery is considered only in highly selected T1–2 N0–1 cases (≤3 cm, no mediastinal involvement) and would require neoadjuvant chemotherapy. The presence of N2 disease here makes surgery inappropriate as primary therapy. **High-Yield:** SCLC is a **chemotherapy-sensitive tumor**. Even extensive-stage disease responds initially to platinum-based chemotherapy, but median OS remains ~10–12 months without maintenance or immunotherapy. 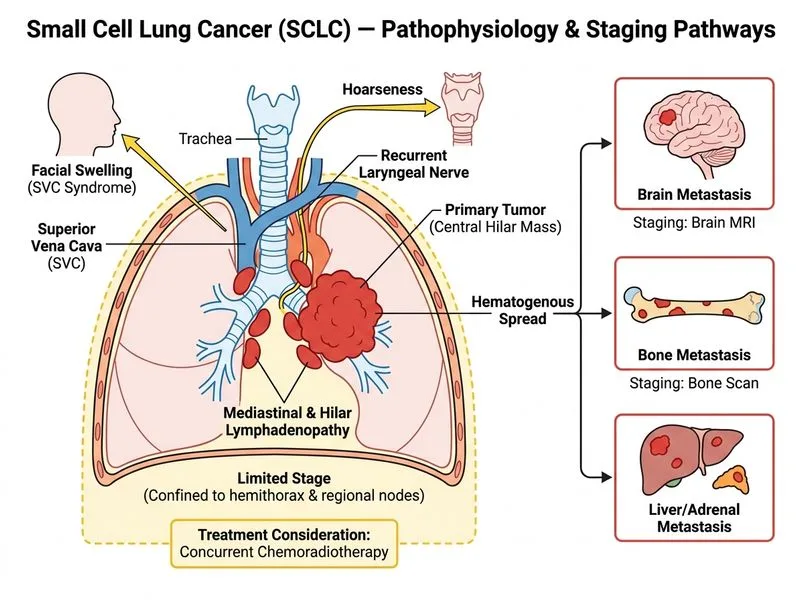
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.