## Prophylactic Cranial Irradiation (PCI) in Limited-Stage SCLC **Key Point:** Prophylactic cranial irradiation (PCI) is the standard of care for patients with limited-stage SCLC who achieve a complete or good partial response to initial chemoradiotherapy. It reduces the cumulative incidence of brain metastases from ~40% to ~15% and improves overall survival by ~5%. ### Evidence and Rationale **High-Yield:** The landmark trial (Aupérin et al., 1999) demonstrated that PCI in SCLC patients with complete response reduces brain relapse risk and improves 3-year overall survival (15% → 20.7%). This benefit is seen across both limited-stage and extensive-stage disease. **Clinical Pearl:** SCLC has a natural propensity for CNS sanctuary disease due to: - High growth fraction and early hematogenous dissemination - Chemotherapy and radiotherapy penetration into the brain is limited - Microscopic disease in the brain is present in ~25% of patients at diagnosis despite negative MRI ### Timing and Technique **Mnemonic:** **PCI = Post-Chemoradio Intervention** — delivered after completion of chemotherapy and thoracic radiotherapy, typically within 4–6 weeks of completing systemic treatment. - **Dose:** 25 Gy in 10 fractions (standard) or 30 Gy in 12 fractions - **Timing:** Within 4–6 weeks of completing chemotherapy (while disease control is optimal) - **Indication:** Complete or near-complete response to induction therapy - **Contraindication:** Extensive-stage disease with brain metastases (use therapeutic whole-brain RT instead) ### Comparison: PCI vs. Observation vs. Therapeutic WBRT | Scenario | Intervention | Rationale | |----------|--------------|----------| | LD-SCLC, complete response | PCI 25 Gy | Reduces brain relapse; improves OS | | LD-SCLC, no response | Observation or salvage therapy | PCI not indicated; poor prognosis | | ED-SCLC, brain mets present | Therapeutic WBRT 30 Gy | Treatment of established disease | | ED-SCLC, no brain mets, CR | PCI (controversial) | May be considered; less robust benefit than LD-SCLC | **Warning:** Common pitfalls: - Delaying PCI beyond 6 weeks reduces efficacy (increased risk of occult brain disease progression) - Confusing PCI (prophylactic, in responders) with therapeutic WBRT (in patients with brain metastases) - Omitting PCI in LD-SCLC responders—this significantly worsens prognosis ### Why Other Options Are Incorrect **Observation alone:** Without PCI, ~40% of LD-SCLC patients will develop brain metastases within 2 years, leading to poor quality of life and shortened survival. Observation is not standard of care after complete response. **Adjuvant topotecan:** There is no evidence for maintenance or adjuvant chemotherapy in SCLC after complete response to induction therapy. Topotecan is used for relapsed disease, not consolidation. **Therapeutic WBRT:** Reserved for patients with symptomatic or imaging-detected brain metastases, not for prophylaxis in asymptomatic patients. [cite:Harrison 21e Ch 111; NCCN Guidelines on Small Cell Lung Cancer] 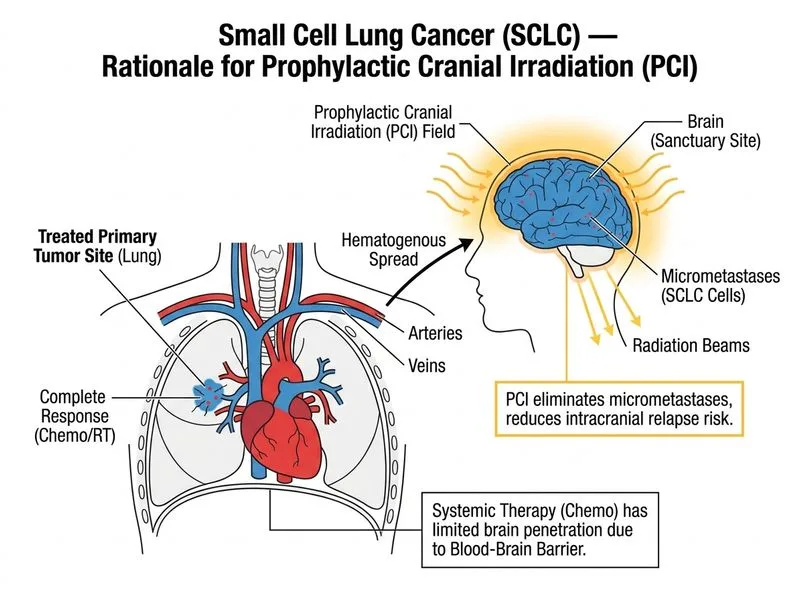
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.