## Diagnostic Confirmation in Hodgkin Lymphoma **Key Point:** Histopathology with immunohistochemistry (IHC) of excised lymph node tissue is the gold standard for diagnosis and subtype classification of Hodgkin lymphoma. ### Why Histopathology + IHC is Definitive 1. **Morphological identification** of diagnostic cells: - Reed-Sternberg (RS) cells — large multinucleated cells with "owl's eye" nuclei - Hodgkin cells — mononuclear variants - Background of small lymphocytes, eosinophils, and plasma cells 2. **Immunophenotype confirmation:** - CD30^+^, CD15^+^ (RS/Hodgkin cells) - CD45^−^, CD20^−^ (typically B-cell marker negative) - CD3^−^ (T-cell marker negative) 3. **Histological subtype classification** (essential for prognosis and treatment): - Nodular sclerosis (most common, ~70%) - Mixed cellularity (~15%) - Lymphocyte-rich (~5%) - Lymphocyte-depleted (rare, ~1%) **High-Yield:** The combination of **morphology + IHC phenotype** is diagnostic; neither alone is sufficient. Excisional biopsy (not needle core) is preferred because it preserves tissue architecture needed to assess background cellularity and fibrosis. ### Investigation Hierarchy | Investigation | Role | Diagnostic? | |---|---|---| | **Histopathology + IHC** | **Definitive diagnosis + subtype** | **YES** | | Flow cytometry | Useful in lymphoid neoplasms; poor for HL (sparse RS cells) | No | | Serum LDH, ESR | Prognostic markers, not diagnostic | No | | PET-CT | Staging and treatment response; not diagnostic | No | **Clinical Pearl:** Flow cytometry is often unhelpful in Hodgkin lymphoma because RS cells are sparse in the background of reactive cells, making them difficult to gate and identify by flow alone. Tissue architecture is critical. **Mnemonic — HL Diagnosis:** **SHIP** = **S**ternberg cells, **H**istology (architecture), **I**mmunohistochemistry (CD30/CD15+, CD45−), **P**henotype confirmation. 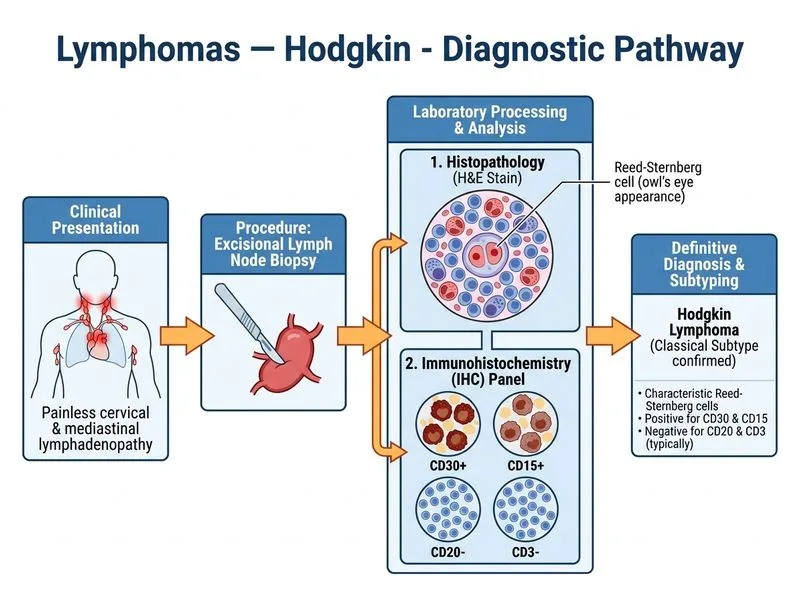
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.