## Clinical Context This patient presents with B symptoms (fever, night sweats), lymphadenopathy, hepatosplenomegaly, elevated LDH, and mediastinal involvement — a classic presentation suggestive of non-Hodgkin lymphoma (NHL), likely a high-grade subtype given the constitutional symptoms. ## Diagnostic Hierarchy in NHL **Key Point:** Tissue diagnosis is mandatory before any treatment in NHL. The diagnosis cannot be established on clinical features, imaging, or laboratory findings alone. **High-Yield:** Excisional (or core needle) biopsy with immunophenotyping (flow cytometry) and immunohistochemistry is the gold standard first step. This provides: - Histologic subtype (diffuse large B-cell, Burkitt, lymphoblastic, etc.) - Immunophenotype (B-cell vs. T-cell, CD5+/− status) - Prognostic markers (Ki-67, TP53 status in some cases) ## Why Excisional Biopsy? Fine-needle aspiration (FNA) is inadequate for lymphoma diagnosis because it cannot assess tissue architecture, which is essential for subtype classification. Excisional biopsy of the most accessible lymph node (avoiding small nodes <1 cm) is preferred. ## Staging Comes After Diagnosis Once histology confirms NHL, staging investigations (CT, PET-CT, bone marrow biopsy if indicated) follow to determine extent of disease and prognosis — but only after tissue diagnosis is secured. **Clinical Pearl:** Mediastinal involvement in a young patient with B symptoms and elevated LDH suggests primary mediastinal B-cell lymphoma (PMBL) or Burkitt lymphoma — both requiring urgent tissue diagnosis and risk stratification before treatment initiation. 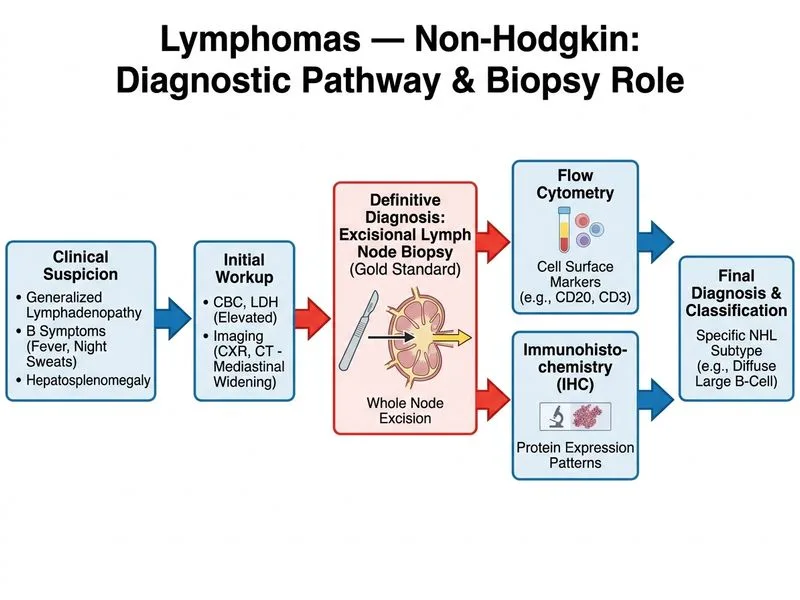
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.