## Classification and MDT Selection This patient presents with **tuberculoid (TT) leprosy**, classified as **paucibacillary (PB) leprosy** based on: - Single lesion (≤5 lesions) - Negative slit-skin smear (smear-negative) - Positive lepromin test (strong cell-mediated immunity) - Well-demarcated lesion with clear sensory loss - Nerve involvement (thickened radial nerve) ### PB vs MB Classification Criteria | Criterion | Paucibacillary (PB) | Multibacillary (MB) | |---|---|---| | **Number of lesions** | ≤5 | >5 | | **Slit-skin smear** | Negative or 1+ | 2+ or more | | **Lepromin test** | Positive | Negative or weakly positive | | **MDT regimen** | Rifampicin + Dapsone | Rifampicin + Dapsone + Clofazimine | | **Duration** | 6 months | 12 months | | **Relapse rate** | <1% | 1-3% | **Key Point:** This patient has **smear-negative disease with a single lesion**, which unequivocally classifies her as **paucibacillary leprosy**, requiring the **2-drug regimen (RFP + DDS) for 6 months**. ### PB MDT Regimen (6 Months) 1. **Rifampicin** 600 mg monthly (supervised) 2. **Dapsone** 100 mg daily (self-administered) + 100 mg monthly (supervised) **High-Yield:** **Smear-negative status is a hallmark of PB leprosy.** Even if a patient has multiple lesions but is smear-negative, they are classified as PB and receive the 6-month regimen. **Clinical Pearl:** Patients with TT leprosy have the best prognosis and lowest relapse rates. Nerve damage may still occur during treatment (Type 1 reaction), requiring corticosteroid therapy, but the infection itself responds rapidly to MDT. **Mnemonic:** **RD for PB** — Rifampicin + Dapsone for Paucibacillary (6 months). **RDC for MB** — Rifampicin + Dapsone + Clofazimine for Multibacillary (12 months). 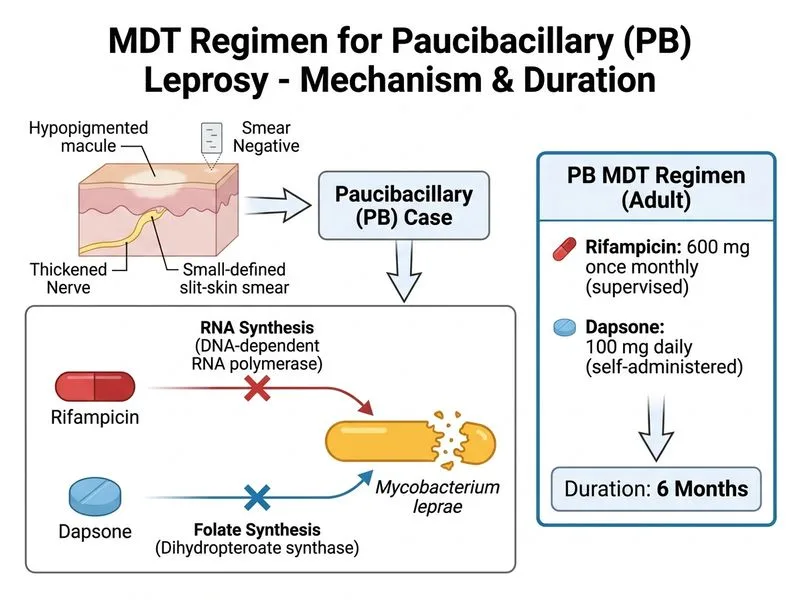
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.