## MDT Regimen Distinction in Multibacillary Leprosy ### Clinical Classification This patient has **>5 skin lesions (8) and >5 nerve trunks (3 is actually ≤5, but with high bacillary index 3+)** — however, the **>5 lesions criterion alone classifies him as MB leprosy**. **Key Point:** Multibacillary leprosy requires a **more intensive and prolonged regimen** compared to paucibacillary leprosy, specifically the addition of a third agent and extension of duration. ### Comparison of MDT Regimens | Component | PB MDT (6 months) | MB MDT (12 months) | |-----------|-------------------|-------------------| | **Rifampicin** | 600 mg monthly (supervised) | 600 mg monthly (supervised) | | **Dapsone** | 100 mg daily (unsupervised) | 100 mg daily (unsupervised) | | **Clofazimine** | — | 300 mg monthly (supervised) + 50 mg daily (unsupervised) | | **Duration** | 6 months | 12 months | | **Infectivity reduction** | Rapid (within 2 weeks) | Slower; requires full course | **High-Yield:** The **addition of clofazimine** is the cardinal distinguishing feature of MB MDT. Clofazimine: - Is a lipophilic antimycobacterial with slow onset (weeks to months) - Accumulates in fatty tissues and mycobacteria - Reduces relapse risk in high bacillary-load disease - Causes reversible skin pigmentation (blue-black discoloration) **Clinical Pearl:** Clofazimine is **NOT used in PB leprosy** because the lower bacillary load and shorter treatment duration do not justify its slow kinetics and cosmetic side effects. **Mnemonic: "MB = More Bacilli = More drugs (add Clofazimine) + More time (12 months)"** 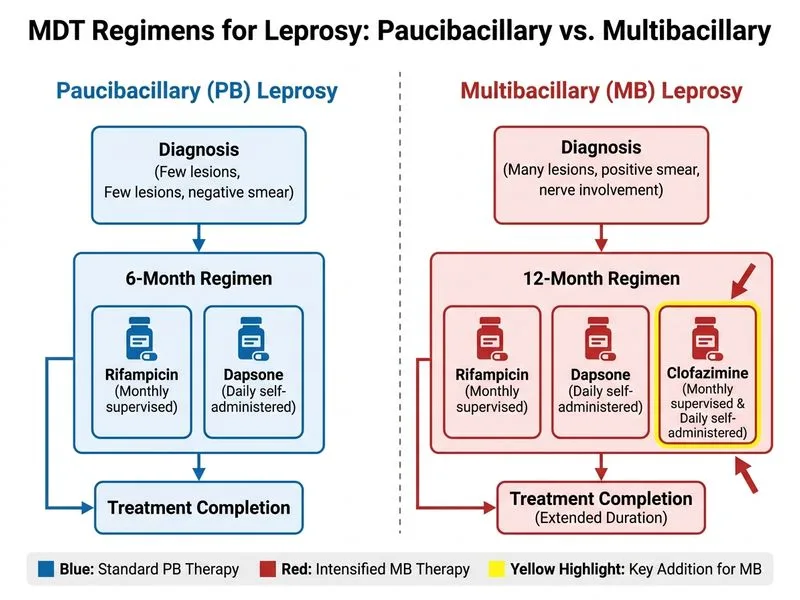
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.