## Clinical Assessment of Meconium Aspiration Syndrome (MAS) ### Pathophysiology Meconium aspiration causes a spectrum of lung injury: 1. **Airway obstruction** — meconium plugging causes ball-valve obstruction, leading to hyperinflation and air trapping 2. **Chemical pneumonitis** — meconium components trigger inflammation 3. **Surfactant inactivation** — meconium impairs surfactant function 4. **Secondary infection risk** — meconium is sterile but increases bacterial colonization ### Clinical Severity Stratification | Feature | Mild MAS | Moderate MAS | Severe MAS | |---------|----------|--------------|------------| | **Respiratory rate** | 40–60/min | 60–80/min | >80/min | | **Retractions** | Mild or absent | Moderate | Severe | | **Oxygen requirement** | Room air or <30% FiO₂ | 30–60% FiO₂ | >60% FiO₂ or mechanical support | | **Chest X-ray** | Normal or mild infiltrates | Patchy infiltrates + hyperinflation | Severe infiltrates, pneumothorax, PPHN | | **Blood gas** | Normal or mild hypoxemia | Moderate hypoxemia + hypercapnia | Severe hypoxemia, acidosis | ### Management Algorithm for This Case ```mermaid flowchart TD A["Meconium-stained delivery<br/>Vigorous infant at birth"]:::outcome --> B{"Respiratory distress<br/>within 2–6 hours?"}:::decision B -->|Yes| C{"Severity assessment"}:::decision C -->|Mild| D["Room air or low-flow O₂<br/>Target SpO₂ 90–95%"]:::action C -->|Moderate| E["Supplemental O₂<br/>Continuous pulse oximetry<br/>Serial blood gas monitoring"]:::action C -->|Severe| F{"Mechanical support<br/>needed?"}:::decision E --> G{"Deterioration?"}:::decision G -->|Yes| H["Consider HFOV or conventional<br/>mechanical ventilation"]:::action F -->|Yes| H F -->|No| E H --> I["Supportive care + address<br/>complications PPHN, air leak"]:::action ``` ### This Patient's Status: **Moderate-to-Severe MAS** **Key Point:** This infant has: - Tachypnea (RR 68/min) with retractions → moderate-to-severe respiratory distress - Hypoxemia (PaO₂ 65 mmHg) and hypercapnia (PaCO₂ 52 mmHg) → gas exchange impairment - Pneumothorax (air leak complication) → requires monitoring but is not immediately life-threatening if small and patient is stable - Vigorous at birth → did NOT require suctioning or intubation (current guidelines do NOT recommend routine intubation for meconium aspiration in vigorous infants) **High-Yield:** Modern MAS management emphasizes: 1. **Selective intubation** — only if severe respiratory failure, not prophylactically 2. **Oxygen titration** — target SpO₂ 90–95% (avoid hyperoxia, which worsens oxidative injury) 3. **Supportive care** — fluids, antibiotics if infection suspected, management of PPHN 4. **Advanced ventilation** — HFOV reserved for failure of conventional support ### Why NOT Immediate Intubation? **Clinical Pearl:** The 2015 AAP/AHA Neonatal Resuscitation Guidelines recommend against routine intubation and suctioning of vigorous infants born through MSAF. Intubation carries risks: - Airway trauma - Ventilator-associated lung injury - Increased PPHN risk if aggressive hyperventilation used This infant is breathing spontaneously and has adequate perfusion (Apgar scores). Intubation is reserved for: - Apnea or gasping - Severe respiratory distress unresponsive to supplemental oxygen - Inability to maintain airway ### Why NOT Prophylactic Surfactant? Surfactant may be considered in severe MAS with respiratory failure, but it is NOT standard prophylaxis in moderate disease. Surfactant is inactivated by meconium, so benefit is limited unless combined with mechanical ventilation. ### Why NOT Immediate Needle Aspiration of Pneumothorax? A **small pneumothorax** (as described) in a stable patient does NOT require immediate intervention. Management is: - Observation with serial chest X-rays - Supplemental oxygen (increases nitrogen washout and resorption) - Needle aspiration or chest tube only if: - Tension pneumothorax (hemodynamic instability, tracheal deviation) - Persistent air leak despite conservative management - Need for mechanical ventilation ### Correct Management Summary **Option B** is correct: Supplemental oxygen (titrated to SpO₂ 90–95%), continuous monitoring, supportive care, and escalation to HFOV if deterioration occurs. **Reasoning:** - Addresses hypoxemia and hypercapnia without over-oxygenation - Allows spontaneous breathing and natural clearance of meconium - Provides a clear escalation pathway if the infant worsens - Avoids unnecessary intubation in a vigorous infant [cite:Nelson Textbook of Pediatrics 21e Ch 97] 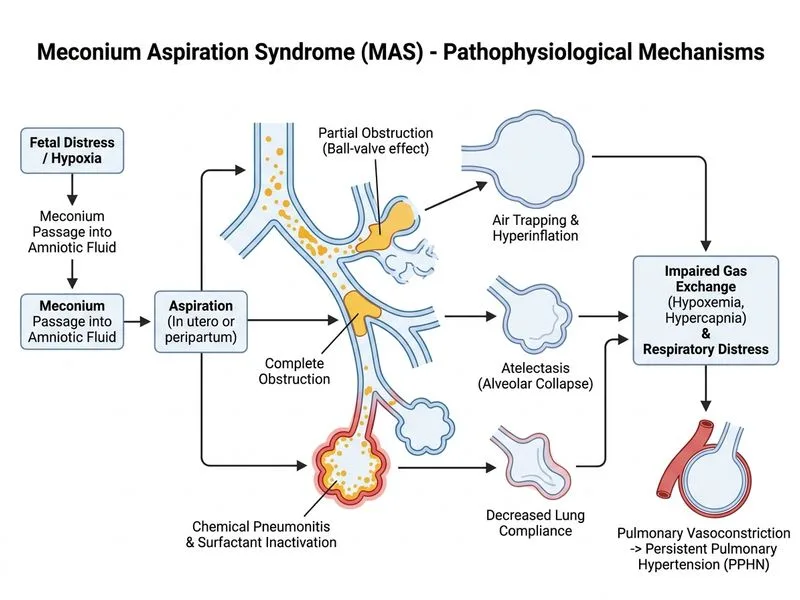
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.