## Meconium Aspiration Syndrome and Persistent Pulmonary Hypertension of the Newborn (PPHN) ### Pathophysiology of PPHN in MAS **Key Point:** PPHN is the most serious complication of MAS, occurring in 5–10% of MAS cases. The mechanism is: 1. **Meconium-induced pulmonary inflammation** → vasoconstriction and remodeling of pulmonary arterioles 2. **Hypoxia and acidosis** → further pulmonary vasoconstriction 3. **Loss of normal postnatal pulmonary vasodilation** → right ventricular afterload increases 4. **Right-to-left shunting** → blood bypasses ventilated lung via foramen ovale and ductus arteriosus 5. **Refractory hypoxemia** — oxygen alone cannot overcome the shunt ### Clinical Features of PPHN | Feature | Present in This Case? | |---------|----------------------| | **Severe hypoxemia (SpO₂ <85% despite high FiO₂)** | ✓ Yes (SpO₂ 82% on FiO₂ 0.80) | | **Hypotension / poor perfusion** | ✓ Yes (MAP 35 mmHg) | | **Right-to-left shunting on echo** | ✓ Yes (across PFO and PDA) | | **Elevated RV pressures** | ✓ Yes (confirmed on echo) | | **Labile oxygenation** | ✓ Expected (worsens with agitation, suctioning) | | **Metabolic acidosis** | ✓ Expected (from tissue hypoxia) | ### Why This Is NOT ARDS or Sepsis **Clinical Pearl:** ARDS and sepsis are diagnoses of exclusion in neonates with refractory hypoxemia and MAS: - **ARDS** presents similarly but does NOT explain the right-to-left shunting pattern on echo or the elevated RV pressures - **Sepsis** is possible but would not cause acute hemodynamic collapse with pulmonary hypertension within 6 hours; meconium is sterile at birth - **PPHN** is the primary pathophysiology here, confirmed by echo findings ### Management Algorithm for Severe MAS with PPHN ```mermaid flowchart TD A["Severe MAS + Respiratory Distress"]:::outcome --> B{"Refractory hypoxemia<br/>SpO₂ <85% on FiO₂ >0.60?"}:::decision B -->|Yes| C{"Echo findings?"}:::decision C -->|PPHN confirmed<br/>Right-to-left shunt| D["Urgent intervention needed"]:::action D --> E{"Air leak present?"}:::decision E -->|Tension pneumothorax| F["Needle decompression<br/>or chest tube"]:::urgent E -->|No air leak| G["Proceed to iNO"]:::action F --> G G --> H["Initiate inhaled nitric oxide<br/>20 ppm initial dose"]:::action H --> I{"Response to iNO?"}:::decision I -->|Good| J["Continue iNO + supportive care"]:::action I -->|Poor| K["Consider ECMO evaluation"]:::urgent B -->|No| L["Continue conventional support"]:::action ``` ### Step-by-Step Management in This Case #### **Step 1: Urgent Decompression of Tension Pneumothorax** **High-Yield:** A **tension pneumothorax** is a life-threatening emergency that must be addressed FIRST, before any other intervention: - **Clinical signs:** Hypotension, poor perfusion, tracheal deviation (if present), unilateral decreased breath sounds - **Management:** - Needle decompression (22–24 G needle, 2nd intercostal space, midclavicular line) for immediate relief - Followed by chest tube placement (36–40 Fr) for definitive drainage - Do NOT delay for imaging confirmation if clinically suspected **Tip:** In this case, the tension pneumothorax is contributing to the hypotension and poor perfusion. Decompression will improve cardiac output and allow better response to subsequent therapies. #### **Step 2: Initiate Inhaled Nitric Oxide (iNO)** **Key Point:** iNO is the gold standard for PPHN management: | Mechanism | Effect | |-----------|--------| | **Selective pulmonary vasodilation** | Decreases RV afterload, improves RV function | | **Selective action** | Acts only on ventilated lung; does NOT cause systemic hypotension | | **Reduces right-to-left shunting** | By lowering pulmonary vascular resistance | | **Improves oxygenation** | Allows blood to perfuse ventilated areas | **Dosing & Administration:** - **Initial dose:** 20 ppm (parts per million) - **Titration:** Increase by 5–10 ppm every 15–30 min if inadequate response, up to 80 ppm - **Weaning:** Once oxygenation improves, reduce gradually over hours to days - **Monitoring:** Methemoglobin levels (target <5%), NO₂ levels, continuous pulse oximetry **Clinical Pearl:** iNO response is rapid (minutes to hours). If no improvement after 4 hours at maximum dose, consider ECMO evaluation. #### **Step 3: Optimize Ventilation Strategy** **Warning:** Aggressive hyperventilation (high pressures, high rates) worsens PPHN by: - Causing barotrauma and air leak - Increasing oxidative stress - Paradoxically worsening pulmonary vasoconstriction **Correct approach:** - **Gentle ventilation:** Permissive hypercapnia (PaCO₂ 45–55 mmHg acceptable) - **Avoid excessive FiO₂:** Target SpO₂ 90–95% (not >95%, which increases oxidative injury) - **Synchronized ventilation:** SIMV or assist-control to reduce patient-ventilator dyssynchrony - **Consider HFOV:** If conventional ventilation fails (better lung recruitment, lower tidal volumes) #### **Step 4: Supportive Measures** - **Sedation & analgesia:** Reduce agitation (which worsens pulmonary vasoconstriction) - **Maintain normothermia:** Hypothermia worsens pulmonary hypertension - **Correct acidosis:** Metabolic acidosis increases PVR; use sodium bicarbonate if pH <7.20 - **Maintain systemic blood pressure:** Inotropes (dopamine, dobutamine) if MAP <40 mmHg - **Avoid hypoxia & hypercarbia:** Both worsen pulmonary vasoconstriction ### Why NOT Increase FiO₂ to 1.0 and Increase Ventilator Pressures? **Option A is incorrect** because: - **FiO₂ 1.0** increases oxidative stress and does NOT address the underlying problem (pulmonary hypertension with right-to-left shunting) - **Increasing ventilator pressures** risks barotrauma, worsens air leak, and paradoxically worsens PPHN - **iNO** is the proven therapy for PPHN, not aggressive ventilation ### Why NOT Start Antibiotics Immediately? **Option C is incorrect** because: - Meconium is sterile at birth; sepsis is unlikely within 6 hours - The clinical picture (acute pulmonary hypertension with echo confirmation) is pathognomonic for PPHN, not sepsis - Antibiotics may be started empirically if sepsis is suspected clinically, but they do NOT address the primary problem ### Why NOT Restrict Fluids? **Option D is incorrect** because: - Pulmonary edema is NOT the primary mechanism here; PPHN is - Fluid restriction may worsen hypotension (MAP already 35 mmHg) - Diuretics are contraindicated in PPHN with hypotension ### Correct Answer Summary **Option B is correct:** The complication is **PPHN** (confirmed by echo findings of right-to-left shunting and elevated RV pressures). The next step is: 1. **Urgent decompression** of the tension pneumothorax (life-threatening emergency) 2. **Initiate iNO** therapy (gold standard for PPHN) 3. Optimize ventilation and supportive care [cite:Nelson Textbook of Pediatrics 21e Ch 97; Avery's Diseases of the Newborn 11e Ch 48] 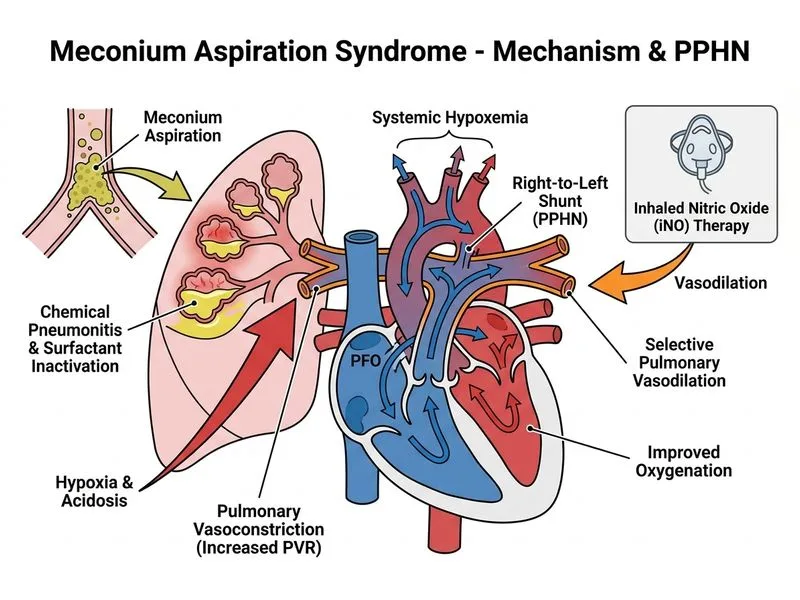
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.