## Meconium Aspiration Syndrome (MAS): Acute Management ### Clinical Context This vigorous neonate with MSAF and respiratory distress represents **mild-to-moderate MAS**. The key distinguishing feature is that the infant was vigorous at birth (Apgar ≥8), which changes the management paradigm. **Key Point:** Routine intubation and suctioning of the trachea is NO LONGER recommended for vigorous infants born through MSAF. The 2015 Neonatal Resuscitation Program (NRP) guidelines emphasize selective intervention based on vigour. ### Pathophysiology of MAS Meconium aspiration causes: 1. **Airway obstruction** — mechanical plugging of small airways 2. **Chemical pneumonitis** — inflammatory response to meconium components 3. **Surfactant inactivation** — meconium impairs surfactant function 4. **Air trapping** — ball-valve mechanism → hyperinflation and barotrauma 5. **Pulmonary hypertension** — hypoxia and inflammation trigger vasoconstriction ### Management Algorithm for MAS ```mermaid flowchart TD A[Meconium-stained amniotic fluid]:::outcome --> B{Vigorous infant?}:::decision B -->|Yes| C[Routine care, NO routine intubation]:::action B -->|No| D[Intubate, visualize cords, suction if meconium present]:::action C --> E[Monitor for respiratory distress]:::action E --> F{RDS develops?}:::decision F -->|Mild| G[Supplemental O₂ + supportive care]:::action F -->|Moderate-Severe| H[Consider CPAP or mechanical ventilation]:::action D --> I[Assess need for further resuscitation]:::action ``` ### Immediate Management for This Case | Feature | This Case | Management | |---------|-----------|-------------| | Vigour at birth | Apgar 8/10 (vigorous) | No routine intubation | | Current SpO₂ | ~65 mmHg on RA | Supplemental O₂ to target 90–95% | | Respiratory distress | Mild-moderate (RR 68, retractions, grunting) | CPAP or observation with O₂ | | CXR findings | Patchy infiltrates + hyperinflation | Consistent with MAS; not severe | | Blood gas | Mild respiratory acidosis (pH 7.28, PaCO₂ 52) | Responsive to oxygenation | **High-Yield:** The goal is to: - Maintain SpO₂ 90–95% (avoid hyperoxia → oxidative stress) - Provide PEEP/CPAP to recruit alveoli and prevent collapse - Avoid unnecessary intubation (reduces barotrauma) - Monitor for deterioration (persistent pulmonary hypertension, pneumothorax) ### When to Escalate Care - Worsening hypoxemia despite supplemental O₂ - Rising PaCO₂ (>60 mmHg) with respiratory acidosis - Signs of air leak (pneumothorax, pneumomediastinum) - Pulmonary hypertension with right-to-left shunting **Clinical Pearl:** Surfactant therapy (exogenous) may be considered in moderate-to-severe MAS requiring mechanical ventilation, but is NOT first-line for mild disease. Prophylactic surfactant in vigorous infants is not indicated. [cite:NRP 2015 Guidelines, Cloherty et al. Manual of Neonatal Care 8e Ch 6] 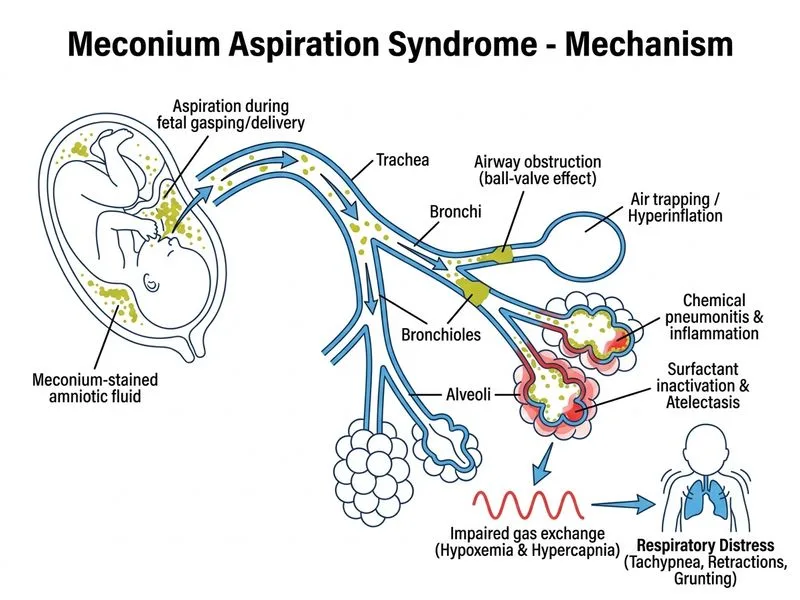
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.