## Severe Meconium Aspiration Syndrome with Pulmonary Hypertension ### Clinical Recognition This case represents **severe MAS with secondary pulmonary hypertension (PH)**. The key features are: - Non-vigorous birth requiring intubation - Meconium visualized and suctioned from trachea - Severe hypoxemia (SpO₂ 78–82%) despite high FiO₂ and mechanical ventilation - Clinical signs of PH: loud P₂, hepatomegaly - Severe CXR findings with bilateral infiltrates and hyperinflation **High-Yield:** Persistent pulmonary hypertension of the newborn (PPHN) is a major complication of severe MAS and is the primary driver of mortality and morbidity in these infants. ### Pathophysiology: MAS → PPHN ```mermaid flowchart TD A[Meconium aspiration]:::outcome --> B[Airway obstruction + chemical pneumonitis]:::outcome B --> C[Hypoxemia + hypercarbia]:::outcome C --> D[Pulmonary vasoconstriction]:::action D --> E[Increased pulmonary vascular resistance]:::outcome E --> F[Right-to-left shunting]:::outcome F --> G[Severe hypoxemia refractory to O₂]:::urgent G --> H{Conventional ventilation adequate?}:::decision H -->|No| I[iNO + consider ECMO]:::action H -->|Yes| J[Continue supportive care]:::action ``` ### Management of Severe MAS with PPHN | Intervention | Rationale | Evidence | |--------------|-----------|----------| | **Optimize ventilation** | Reduce hypercarbia, normalize pH | Alkalosis reduces PVR | | **Inhaled nitric oxide (iNO)** | Selective pulmonary vasodilator; reduces PVR without systemic effects | First-line for PPHN; improves oxygenation in 50–60% of cases | | **Gentle ventilation strategy** | Avoid barotrauma and volutrauma in already-damaged lungs | Permissive hypercarbia acceptable if pH >7.20 | | **Sedation + paralysis** | Reduce agitation, synchronize with ventilator, reduce oxygen demand | Improves ventilation-perfusion matching | | **ECMO** | Provides gas exchange while lungs recover; allows "lung rest" | Indicated if iNO fails or FiO₂ requirement >0.8 with SpO₂ <85% | | **Avoid hyperoxia** | Excessive O₂ → oxidative stress, free radical injury | Target SpO₂ 90–95% even in severe cases | **Key Point:** In severe MAS with PPHN, the goal is NOT to achieve "normal" oxygenation at any cost. Instead, the strategy is: 1. Optimize ventilation (correct hypercarbia, maintain pH >7.20) 2. Reduce pulmonary vascular resistance with iNO 3. If iNO fails → ECMO for bridging support ### Why iNO is First-Line for PPHN in MAS **Mechanism:** - Nitric oxide (NO) is an endogenous pulmonary vasodilator - Acts on soluble guanylate cyclase → ↑ cGMP → smooth muscle relaxation - Selective effect on ventilated lung units (where it is produced) - Does NOT cause systemic hypotension (rapidly inactivated by hemoglobin) **Dosing:** 5–20 ppm inhaled; titrate based on response **Response:** Improves oxygenation in ~50–60% of infants with PPHN; reduces need for ECMO by ~40% ### ECMO Indications in Neonatal PPHN - Failure of iNO (SpO₂ remains <85% despite iNO + optimal ventilation) - FiO₂ requirement >0.8 with persistent hypoxemia - Severe hypercapnia (PaCO₂ >80 mmHg) despite ventilation - Severe metabolic acidosis (pH <7.15) unresponsive to therapy - Acute deterioration with shock **Clinical Pearl:** ECMO is a "rescue" therapy, not first-line. It allows the lungs to rest while providing systemic gas exchange, giving time for inflammation to resolve and pulmonary vascular tone to normalize. ### Why Other Options Are Suboptimal **Increasing FiO₂ to 1.0:** - Already on FiO₂ 0.8 with inadequate response - Further hyperoxia increases oxidative stress and free radical injury - The problem is not oxygenation delivery but pulmonary vasoconstriction causing right-to-left shunting **Sildenafil alone:** - Phosphodiesterase-5 inhibitor; reduces PVR - Slower onset than iNO; not first-line for acute severe PPHN - Can be used as adjunctive therapy but does not replace iNO **Surfactant lavage:** - Not standard therapy for MAS - May cause additional lung injury and airway obstruction - No evidence base for this approach [cite:Cloherty et al. Manual of Neonatal Care 8e Ch 6; Harrison 21e Ch 297; Goldsmith et al. Assisted Ventilation of the Neonate 6e Ch 12] 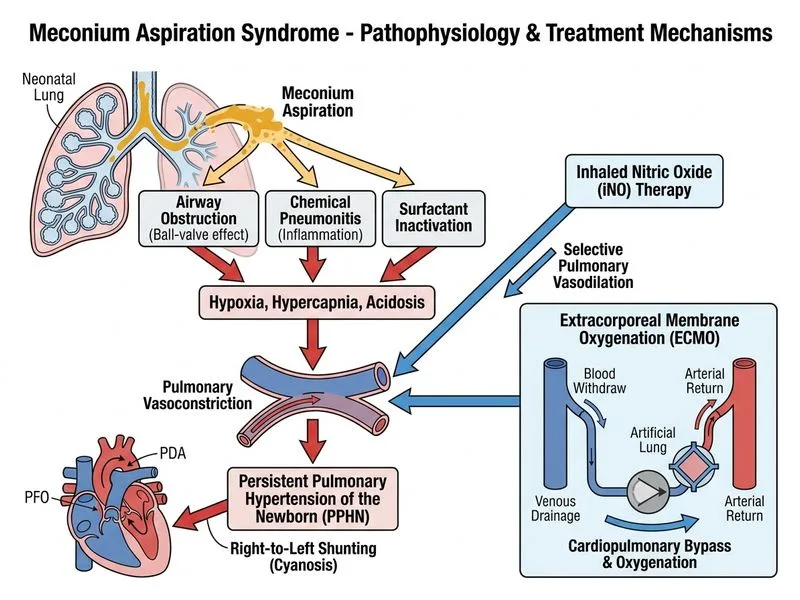
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.