## Severe Meconium Aspiration Syndrome with Complications ### Clinical Scenario Analysis This neonate presents with **severe MAS** complicated by: - Non-vigorous status at birth (Apgar 4/6) → required intubation - Severe hypoxemia (PaO₂ 65 mmHg on FiO₂ 0.8) - Respiratory acidosis (pH 7.18, PaCO₂ 58 mmHg) - Extensive bilateral infiltrates with severe hyperinflation - **Pneumothorax** (right-sided) — a critical air leak complication ### Immediate Management Priority: Pneumothorax **Key Point:** A pneumothorax in a mechanically ventilated neonate is a medical emergency. It must be addressed urgently because: 1. It worsens gas exchange and hypoxemia 2. It increases intrathoracic pressure, reducing venous return and cardiac output 3. It can progress to tension pneumothorax, causing cardiovascular collapse 4. Continued positive pressure ventilation will worsen the pneumothorax ### Management Algorithm ```mermaid flowchart TD A[Severe MAS + Pneumothorax]:::outcome --> B{Hemodynamically stable?}:::decision B -->|Yes| C[Needle aspiration or chest tube]:::action B -->|No| D[Immediate needle aspiration]:::urgent C --> E[Optimize ventilation settings]:::action D --> E E --> F{Refractory hypoxemia?}:::decision F -->|Yes| G[Consider iNO + high-frequency ventilation]:::action F -->|No| H[Continue conventional management]:::action G --> I{Still failing?}:::decision I -->|Yes| J[ECMO consideration]:::urgent I -->|No| K[Supportive care]:::outcome ``` ### Treatment Steps | Intervention | Rationale | |--------------|----------| | **Needle aspiration or chest tube** | Immediate decompression of pneumothorax; relieves pressure on lungs and heart | | **Reduce ventilator pressures** | Lower peak inspiratory pressure (PIP) and PEEP to reduce further air trapping | | **Inhaled nitric oxide (iNO)** | Selective pulmonary vasodilator; improves ventilation-perfusion matching and reduces pulmonary hypertension in severe MAS | | **High-frequency oscillatory ventilation (HFOV)** | Alternative if conventional ventilation worsens air trapping; uses smaller tidal volumes | | **Surfactant** | May be considered but is NOT the immediate priority when pneumothorax is present | **High-Yield:** The sequence in severe MAS with air leak: 1. **First:** Decompress the pneumothorax (needle or chest tube) 2. **Second:** Optimize conventional ventilation (gentle ventilation strategy) 3. **Third:** Add iNO if persistent hypoxemia and pulmonary hypertension 4. **Fourth:** Consider HFOV or ECMO only if refractory to above **Clinical Pearl:** Exogenous surfactant in MAS is controversial and NOT standard first-line. While some studies suggest benefit in severe cases, the immediate life threat here is the pneumothorax, not surfactant deficiency. Surfactant can be considered *after* stabilization of the pneumothorax. ### Why NOT Other Options **Increasing FiO₂ and ventilator rate (Option A):** - Worsens air trapping and pneumothorax - Does not address the underlying mechanical problem - Increases barotrauma risk **Surfactant alone (Option B):** - Does not address the pneumothorax - Surfactant is not first-line in MAS and will not improve the air leak - Delaying pneumothorax management is dangerous **ECMO immediately (Option D):** - Premature; ECMO is reserved for refractory respiratory failure after optimization of conventional management - Not indicated before attempting needle aspiration, iNO, and HFOV - Requires specialized centers and carries significant morbidity [cite:Cloherty et al. Manual of Neonatal Care 9e Ch 25; Goldsmith et al. Assisted Ventilation of the Neonate 6e Ch 12] ## Summary The correct answer is **needle aspiration or chest tube placement for pneumothorax and consider inhaled nitric oxide (iNO)** because the pneumothorax is the immediate life-threatening complication that must be decompressed urgently, followed by optimization of ventilation and addition of iNO for refractory hypoxemia. 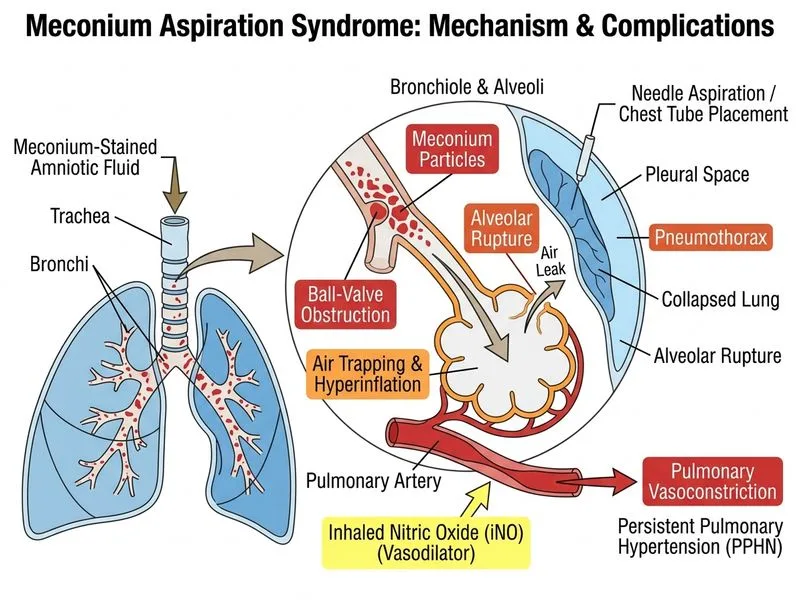
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.