## Clinical Context This is a non-vigorous term neonate with severe MAS, now on mechanical ventilation with an air leak complication (pneumothorax). The infant has persistent hypoxemia and hypercapnia despite moderate ventilator settings. ## Pathophysiology of Severe MAS **Key Point:** Meconium is a chemical irritant that causes: 1. Direct airway obstruction (ball-valve effect) 2. Chemical pneumonitis with surfactant inactivation 3. Increased airway resistance and decreased compliance 4. Ventilation-perfusion mismatch and intrapulmonary shunting 5. Air trapping → barotrauma → air leak syndromes (pneumothorax, pneumomediastinum) ## Management Strategy for Severe MAS on Ventilation ```mermaid flowchart TD A[Severe MAS on mechanical ventilation]:::outcome --> B{Adequate oxygenation?}:::decision B -->|No, PaO₂ < 80 on FiO₂ 0.6| C[Consider surfactant]:::action C --> D{Response to surfactant?}:::decision D -->|Improved| E[Continue conventional ventilation]:::action D -->|No improvement| F[Escalate to HFOV]:::action B -->|Yes| G[Optimize conventional settings]:::action H[Air leak present?]:::decision H -->|Small pneumothorax, stable| I[Observe, supplemental O₂]:::action H -->|Tension pneumothorax| J[Emergency needle aspiration]:::urgent ``` **High-Yield:** Exogenous surfactant in severe MAS: - Restores surfactant function inactivated by meconium - Improves lung compliance and oxygenation - Reduces need for high ventilator pressures - Decreases risk of air leak syndromes - Evidence supports use in severe MAS (PaO₂ < 80 on FiO₂ > 0.5) ## Management of Pneumothorax in MAS | Type | Clinical Features | Management | |------|-------------------|-------------| | Small, asymptomatic | Incidental finding, stable vitals, SpO₂ adequate | Supplemental O₂, observation, serial CXR | | Symptomatic/tension | Hypotension, bradycardia, unilateral breath sounds, tracheal deviation | Emergency needle aspiration (2nd ICS, midclavicular line) | | Persistent/enlarging | Worsening despite treatment | Chest tube placement | **Clinical Pearl:** In this case, the pneumothorax is small and the infant is on mechanical ventilation (positive pressure will worsen it). However, the primary issue is inadequate oxygenation and ventilation—surfactant addresses the underlying problem (surfactant inactivation) and may reduce further air leak. ## Why NOT Increase Pressure/FiO₂ First? **Warning:** Aggressive increase in ventilator pressures in MAS worsens air trapping and increases barotrauma risk. Surfactant replacement is more physiologic. **Key Point:** The sequence is: 1. Optimize conventional ventilation (current settings are moderate) 2. Add surfactant to restore compliance and reduce pressure requirements 3. If still hypoxemic → HFOV (uses lower tidal volumes, reduces air leak risk) [cite:Nelson Essentials of Pediatrics 21e Ch 95, Cloherty et al. Manual of Neonatal Care 9e] 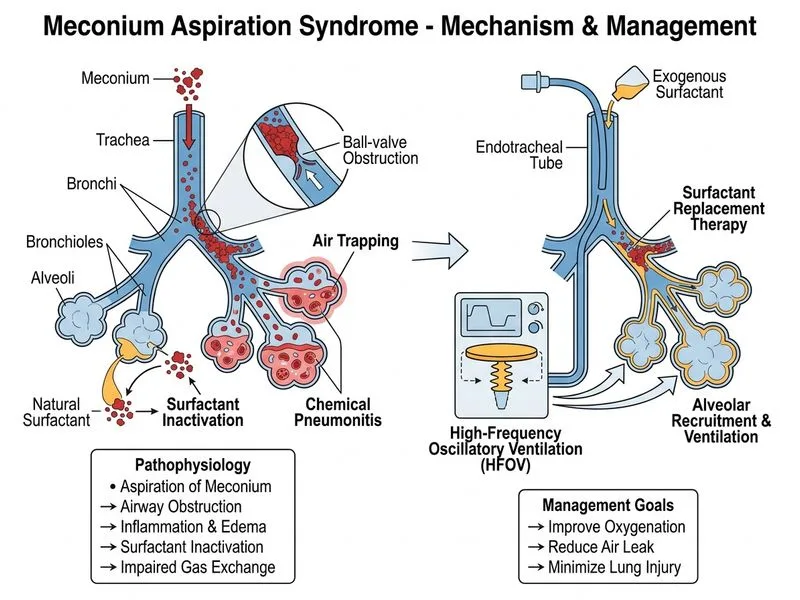
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.