## Pathophysiology of Meconium Aspiration Syndrome **Key Point:** The **primary** pathophysiological mechanism of meconium aspiration syndrome (MAS) is **direct chemical pneumonitis from meconium-induced surfactant inactivation**. Meconium contains bile salts, free fatty acids, and pancreatic enzymes that directly inactivate surfactant and trigger an intense inflammatory response in the lung parenchyma. ### Primary Mechanism: Chemical Pneumonitis & Surfactant Inactivation Meconium is a potent chemical irritant. Upon aspiration: 1. **Surfactant inactivation** — Bile acids and free fatty acids in meconium directly inhibit surfactant function, reducing alveolar surface tension regulation and causing diffuse alveolar collapse and non-uniform ventilation. 2. **Chemical pneumonitis** — Meconium activates complement, stimulates cytokine release (IL-1β, IL-6, IL-8, TNF-α), and causes direct epithelial injury, leading to an inflammatory pneumonitis that begins almost immediately after aspiration. 3. **Persistent pulmonary hypertension (PPHN)** — The inflammatory mediators cause pulmonary vasoconstriction, which is a major driver of hypoxemia in MAS. ### Secondary Mechanical Component The ball-valve/airway obstruction mechanism (Option B) is a **contributing** but secondary mechanism. Larger meconium particles can cause partial airway plugging and air trapping, but this is not the *primary* driver of the pathophysiology as described in major pediatric references. **High-Yield (Nelson's):** Nelson Textbook of Pediatrics (21e, Ch. 102) identifies chemical injury to the lung parenchyma — via surfactant inactivation and inflammatory pneumonitis — as the central pathophysiological mechanism of MAS, with mechanical obstruction as an additional contributor. ### Why Other Options Are Incorrect - **B (Ball-valve/air trapping):** A real but secondary mechanism; not the primary pathophysiology per standard references. - **C (Pulmonary edema from L→R shunting):** This is a consequence of PPHN (right-to-left shunting occurs, not left-to-right), not a primary mechanism. - **D (Bacterial superinfection):** A potential late complication, not the primary or immediate mechanism. **Clinical Pearl:** The diffuse haziness and hyperinflation on CXR in MAS reflect both surfactant dysfunction (atelectasis) and air trapping, but the underlying driver is chemical injury — which is why surfactant replacement therapy has a role in management. [cite: Nelson Textbook of Pediatrics 21e Ch 102; Fanaroff & Martin's Neonatal-Perinatal Medicine 11e] 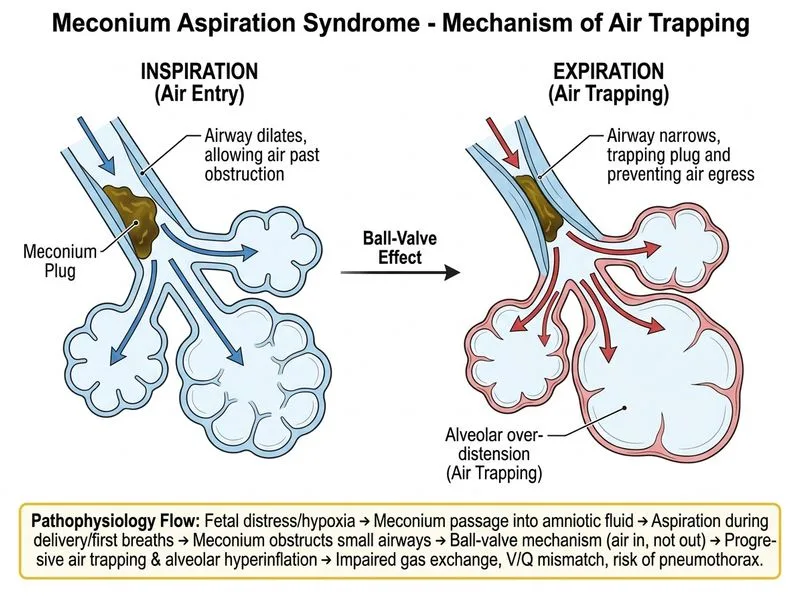
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.